Rheumatoid Arthritis in the Foot and Ankle
Summary: Rheumatoid arthritis (RA) is a chronic, autoimmune disease that multiple attacks joints in the body, commonly including the feet and ankles. In fact, foot symptoms are the first sign of RA in some patients, and 9 out of 10 people with RA eventually experience them.
This article reviews the signs, symptoms, diagnosis and treatments for RA in the feet and ankles.

The exact cause of RA is still unknown. It is thought to be genetic (inherited), and doctors also think it may be triggered by infections, viruses and/or bacteria. RA affects about 1% of the population. Women are affected three times more than men, and symptoms most often appear between the age of 40 to 60.
Which joints are affected by rheumatoid arthritis?
RA commonly affects small joints in the hands, wrists and feet, but it can also affect the ankles and larger joints such as knees or elbows.
How does rheumatoid arthritis affect your foot and ankle?
Rheumatoid arthritis in the foot and ankle is common. RA often starts in the small joints of the hands, wrists, and feet. More than 90% of people with RA acquire foot and ankle symptoms over the course of the disease. In about 20% of patients, foot and ankle symptoms are the first signs of RA.
The joints of your body are covered with a lining known as synovium that lubricates the joint and makes it easier to move. In RA, the immune system attacks your body’s own tissues, including the synovium. It swells, gets inflamed, and destroys the surfaces of the bones that comprise the joint, along with the ligaments and other tissues that support it. Damaged, weakened ligaments can lead to claw toes or hammertoes. Bones can also lose density and become soft. Bone density conditions (osteopenia and osteoporosis) can cause stress fractures or bone collapse.
What are the symptoms of rheumatoid arthritis in the foot and ankle?
The most common symptoms are pain, swelling, and stiffness. While osteoarthritis of the foot or ankle most often affects one joint, RA usually occurs in both feet, typically in the same joint on each foot. Here’s a table that gives you an idea of how RA presents in your feet.
Rheumatoid arthritis symptoms of the foot and ankle by location
Ankle
- Where it is/What it does: Provides up-and-down motion of the foot.
- Early signs and symptoms: Trouble with ramps and inclines.
- Later-stage symptoms: Painful to walk or stand.
Hindfoot
- Where it is/What it does: Heel region of the foot; its main function is side-to-side motion.
- Early signs and symptoms: Difficulty walking on uneven ground, grass, or gravel.
- Later-stage symptoms: Alignment of the foot may shift as bones move out of their normal positions. This can result in pain in the posterior tibial tendon (the main tendon that supports the arch) and may lead to acquired flatfoot deformity .
Midfoot
- Where it is/What it does: Top of the foot.
- Early signs and symptoms: Ligaments that support the midfoot become weak, which can lead to collapsed arches.
- Later-stage symptoms: Once the arch collapses, the front of the foot may start to point outward. Rheumatoid arthritis can also damage cartilage, causing arthritic pain. Over time, the shape of the foot may change, such as the development of a large bony bump on the arch.
Forefoot
- Where it is/What it does: Toes and ball of the foot.
- Early signs and symptoms: Changes may include bunions, claw toes, and pain under the ball of the foot. While each of these problems is common, in rheumatoid arthritis they often occur together.
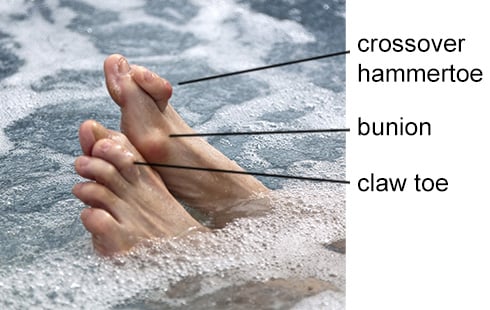
- Later-stage symptoms: Bunions are usually severe, with the big toe crossing over the second toe. Painful bumps may form on the ball of the foot, leading to calluses. Dislocations of toes 2 through 5 can cause rigid claw toes. In severe cases, ulcers may form due to abnormal pressure.
Can rheumatoid arthritis cause problems with tendons?
Yes. Tendons surround the joints of the foot and ankle. Often, a tight Achilles tendon worsens a flatfoot condition, so, exercise as best you can to help keep tendons flexible and strong.
How can I tell if my foot pain is caused by rheumatoid arthritis?
First, your healthcare team will talk to you about your symptoms, discuss your health, and review your medical history. Then your doctor will perform an exam of your foot and ankle, and then possibly order tests.
The exam
Your doctor will check your skin for calluses. The most common place for these is on the ball of the foot. They will look at your foot’s shape. Are there bunions, hammertoes, claw toes or flatfeet? Are the joints still flexible or are they stiff?
In more advanced RA, there may be a total loss of cartilage and the joints could get very stiff. Do your joints feel tender with pressure? Your doctor will apply gentle pressure at your joints to figure out which ones are involved and need treatment.
Tests
Based on what your doctor finds, they may order some tests to get a clear image of what’s going on in order to decide how best to treat your foot.
These tests may include X-rays to show the position of the bones. They may ask you to bear weight on the foot during the X-ray to see what the bones look like during normal use. They may also order computerized tomography, also known as a CT scan, of your foot. These special, cross-sectional images can provide a closer look at each joint when the foot is severely deformed.
MRI (magnetic resonance imaging) scans show soft tissue, ligaments and tendons, and can identify if they are inflamed (tendonitis) or torn.
What kind of doctor can treat rheumatoid arthritis of the foot and ankle?
If your primary care doctor suspects you have rheumatoid arthritis, they may refer you to a rheumatologist. It could also be that you have another, less inflammatory type of arthritis, but a rheumatologist is best able to make a diagnosis. If a rheumatologist determines you have osteoarthritis instead, they may recommend you meet with an orthopedist (orthopedic surgeon) who specializes in foot and ankle conditions. Rheumatoid arthritis patients who experience inflammation in the foot and ankle are often treated by a multidisciplinary team that includes their primary care physician, a rheumatologist, a podiatrist and an orthopedist. Other healthcare clinicians who may be of help include physical and occupational therapists, and social workers.
How is rheumatoid arthritis in the foot or ankle treated?
There is no cure for RA, but there are many nonsurgical and surgical treatment options that enable people to manage pain, stay active, and live full lives. Medical/conservative management is the mainstay. Surgery is a last resort if medical treatments are unsuccessful.
How can rheumatoid arthritis in the foot be treated without surgery?
Orthopedic treatment may provide symptom relief but does not stop the disease process. Still, many patients will have symptom relief without surgery. One such option is a steroid injection. Corticosteroids can reduce inflammation and pain in the short term. Your doctor may also prescribe disease modifying anti-rheumatic drugs (DMARDs), such as methotrexate. There are also NSAIDs (nonsteroidal anti-inflammatory drugs) such as ibuprofen or naproxen which can reduce pain and inflammation. Always check with your doctor before you take any medication- even over the counter.
Sometimes, it’s the simple things such as rest or icing the joint that may be the most effective. Rest your foot by taking a break from things that make the pain worse. Place ice on the area of pain for 20 minutes. Always wrap the ice pack in a washcloth or something so that it does not contact your skin directly.
Relief may also come from things you wear. Firm shoes with a wide toe box and arch support are usually best. An orthotic is a shoe insert that can help to reduce pressure and decrease pain and calluses from forming. Watch out for hard orthotics as they may actually cause more pain. A customized, prescription orthotic is made of softer material and best relieves pressure on the foot. If you need support at the back of foot and ankle, a lace-up ankle brace made of plastic or leather can help.
Depending on the damage to cartilage, your doctor may suggest surgery.
What surgery is there for rheumatoid arthritis of the foot and ankle?
Fusion surgery in the foot (such as a midfoot fusion) or ankle is the most common. These procedures provide rheumatoid arthritis foot and/or ankle pain relief, but can compromise flexibility. Other procedures include total ankle replacement and toe joint resections. The appropriate option depends on each patient’s condition and the joints that are affected.
Midfoot surgery for RA
Midfoot fusion is the most reliable surgery for the joints of the midfoot. It helps to restore the arch, lessen prominences, reduce pain, and improve chance for normal footwear.
Forefoot surgery for RA
For forefoot issues, the options range from joint sparing procedures that preserve motion to fusion of the toes. The appropriate surgery depends on your flexibility and the health of your cartilage. These procedures can provide good function and improve odds for normal footwear.
Ankle surgery for RA
The most common surgery for RA is ankle fusion. This is when two or more bones that form the ankle joint are fused together using hardware such as screws and plates. An ankle fusion relieves pain but results in loss of the up-and-down motion of the ankle. This requires nearby joints to compensate for this loss of motion.
Total ankle replacement is another surgical option. Patients with other joint issues around the heel or those who already had fusions may be well suited for ankle replacements. It avoids adjacent joint arthritis caused by overcompensation for loss of movement in another joint.
Preparing for foot and ankle surgery and your recovery
Many medications that help with RA affect the body’s ability to heal and fight infection. Your surgeon can work with your rheumatologist to decide what to stop taking prior to surgery and when to resume the medication(s). Typically, foot surgeries require that no weight be placed on the foot for about two-six weeks. Since these surgeries are planned, it is good to know this in advance to prepare your home and line up your support system to help you as you recover.
Key takeaways
- The best means to manage your RA are through medical care and newer medications. Surgery can help but should be a last resort.
- The main goal is to get rid of the pain. Keep in mind, even if one finds relief and can begin to wear sandals or mid height heels with ease, it is still best that these types of shoes are not worn often.
This article was based on a presentation by Dr. Behrens to the HSS Early RA Support and Education Program.

