Midfoot Fusion: Surgery for Arthritis Foot Pain
What is a midfoot fusion?
Midfoot fusion (also known as midfoot arthrodesis) is an orthopedic surgery that permanently fixes or “fuses” the bones of one or more joints in the midfoot. It may include a tarsometatarsal, navicular-cuneiform, and/or talonavicular fusion.
Bones and joints of the midfoot
The midfoot bones include the navicular, the cuboid and three cuneiform bones. They bridge the metatarsal bones in the forefoot and the talus and calcaneus of the hindfoot. These bones create the bony arch of the foot.
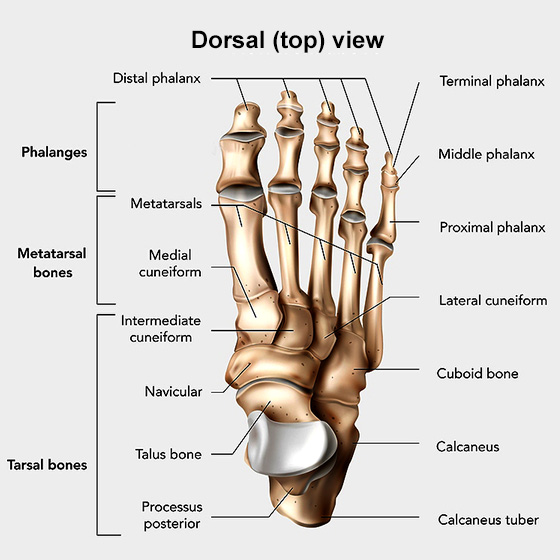
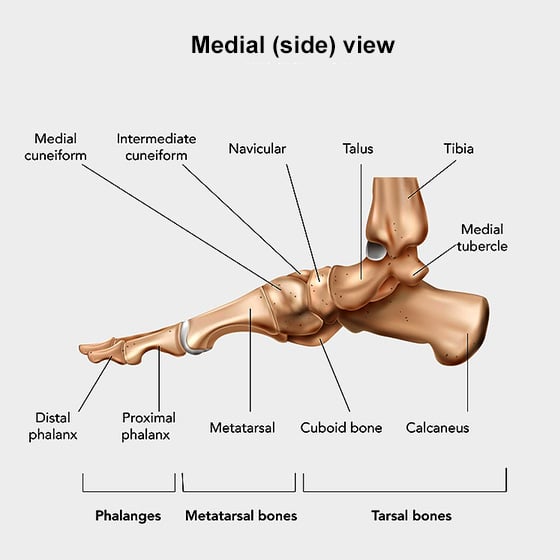
What conditions does midfoot fusion surgery treat?
Midfoot fusion is used to treat joint pain caused by midfoot arthritis or, in some cases, severe injury to the ligaments that creates instability in the arch. The joints of the midfoot do not have much motion, even when they are not damaged. Fusing them can reduce or eliminate foot pain without significantly compromising your activity level or ability to walk and run.
What bones are fused in a midfoot fusion?
This depends on which midfoot joints are affected. Most often the cuneiform bones are fused to the metatarsal bones or to the navicular bone. Your surgeon would recommend fusion of joints where you have pain and arthritis.
How does midfoot fusion surgery work?
Accessing the joints from the top of the foot, the orthopedic surgeon first removes damaged cartilage and joint surfaces. Portions of the surfaces of the affected bones are then removed, and the bones are connected with metal plates and screws, which hold the bones in place and allow them to grow together (“fuse”). Sometimes the surgeon will add bone graft either from another bone in your body, like your iliac crest (near the hip) or heel, or they will use synthetic or cadaver derived bone graft. This helps accelerate bone healing.
Most midfoot fusions are done using a nerve block (regional anesthesia) while you under mild twilight sedation. First, the anesthesiologist will sedate you with propofol. Once you are in a light sleep, they will perform a popliteal fossa block. This will numb your leg from the knee down. It is typically a long-acting block that may last from 24 to 48 hours. On rare instances, it can last as long as three days. This is done for pain control and comfort during and after the procedure. Sometimes, the anesthesiologist will also do an epidural, or “spinal,” in addition to the medication behind the knee. This will numb you from the waist down during the procedure and wears off in the recovery room.
How long does midfoot fusion surgery take?
The surgery itself takes about two hours, but this can vary depending on how severe the damage is to your foot and how many joints are involved in the surgery. You should anticipate more time for presurgical preparation (two hours) and postsurgical recovery (two hours) before going home.
Does the metal hardware used in midfoot fusion stay in your foot?
The metal can remain in your foot forever without causing any harm. We only take the hardware out if it bothers you or there is a strong personal preference. Hardware removal requires a minor procedure in the operating room once the bone is fully healed, typically 6 to 12 months after the original procedure after the bones have healed.
Do I have to stay overnight for a midfoot fusion?
No. Most of our surgeries are ambulatory (outpatient procedures). You typically come in two hours before your procedure and stay about one to two hours after the procedure, however, you should leave your whole day open.
What is the recovery time for a midfoot fusion?
Swelling, pain, and bruising are all normal after surgery. Elevating the foot and icing regimens during the first two weeks are extremely important to reduce swelling and control postsurgical pain. Postoperative pain typically lasts two to three days. You would take Tylenol and NSAIDs every six to eight hours as your primary pain control for three days. If pain becomes severe you may need a few opioid pills.
What is the recovery like for midfoot fusion?
Swelling, pain, and bruising are all normal after surgery. Elevating the foot and icing regimens during the first two weeks are extremely important to reduce swelling and control postsurgical pain.
You may notice swelling and bruising that also travels into the toes, even on those which were not involved in the surgery. This swelling will go up and down depending on how much you elevate. The bruising may also change location or color. This is normal. A small amount of drainage is also normal after surgery. You may have good days and bad days. Try to limit your activity.
Elevation and icing protocols
I recommend elevating 80% of the time during the first week and 50% of the time the second week. Placing your leg on two or three pillows should be sufficient, but the higher the better.
You should ice (20 minutes on, 20 minutes off) several times a day after surgery. You will not feel the ice through the splint, so first try icing behind your knee. When you return for your first post-op appointment, your dressing will be removed, and you will be able to ice the foot directly.
Is physical therapy necessary after midfoot fusion?
Yes. Physical therapy is necessary after surgery to regain motion of the ankle, break up scar tissue, and to decrease swelling. You may find that you have some muscle weakness after surgery so regaining your strength is also important. A physical therapist will also help you with your gait and balance. This is typically started three to four weeks after the procedure and is continued until your goals are met.
Will I need to take pain medication after a midfoot fusion?
For the first several days after surgery, you should take ibuprofen (Advil) and acetaminophen (Tylenol) strictly every six hours. This will reduce and/or eliminate the need for opioid medications, but you will have a prescription for 5 to 15 tablets of 5mg oxycodone, depending on the procedure. Most patients do not require opioids past the third day after surgery. You will also take aspirin daily for two to six weeks after surgery to help prevent blood clots. If you have a history of blood clots in your family or are at high risk for blood clots, you may receive a different medication.
Some patients may also need to take anti-nausea medication (Zofran) and/or medications to alleviate constipation caused by anesthesia and/or opioid use. Usually, this means taking sodium docusate (Colace), although you may also be prescribed senna glycoside.
Supplements for bone health
After surgery, you should take calcium citrate with vitamin D3 supplements daily for three months after surgery to assist with your recovery.
What are the risks of midfoot fusion surgery?
All surgery has some risk, but complications are very rare in foot and ankle surgery. Nonunion, where the bones do not heal properly, requiring a second surgery, affects about 2% to 5% of healthy patients who follow recovery guidelines. Some people also experience postsurgical numbness longer than the typical timeframe of two to three weeks. Less than 1% of people who undergo midfoot fusion may experience one of the following problems: blood clots, infection, or poor wound healing at the incision site.
Patients who have slow or poor wound healing may have to wait longer than usual before allowing their foot to get wet, and/or a larger scar than anticipated. While very rare, if infection occurs, you will need antibiotics and, possibly, additional surgery.
If the bones do not heal correctly (nonunion), the surgery may need to be repeated. Smoking, nicotine use, placing weight on your foot too soon after surgery, and diabetes all increase this risk. In an otherwise healthy patient who is compliant with the post-op recovery, the risk is about 2% to 5%.
What is the success rate of midfoot fusion surgery?
Successful union of the affected bones is achieved about 90% to 95% of the time.1 The true measure of success, however, lies in the reduction of elimination of pain, which is the goal of the surgery. Continued pain is always possible, as surgery is not 100% guaranteed to eliminate it.
If you continue to have pain, or develop new pain after surgery, we will continue to evaluate and monitor you throughout your recovery and work to address it. Depending on how long pain continues, it may help to remove the hardware (as described in the next section), to alleviate the pain. If this does not help, we will look into it further to see if you require more PT, additional therapy (shockwave therapy, injections), or an additional surgery.
References
- Fraser TW, Miles DT, Huang N, Davis FB, Dunlap BD, Doty JF. Radiographic Outcomes, Union Rates, and Complications Associated With Plantar Implant Positioning for Midfoot Arthrodesis. Foot Ankle Orthop. 2021 Jul 14;6(3):24730114211027115. doi: 10.1177/24730114211027115. PMID: 35097463; PMCID: PMC8702960.


