Stress Fractures of the Foot and Ankle
- What is a stress fracture?
- Causes of a stress fracture in the foot and ankle
- What bones in the foot and ankle are affected by a stress fracture?
- What are the symptoms of a stress fracture in the foot and ankle?
- How are stress fractures diagnosed?
- How do you treat a stress fracture?
- How long does it take for a stress fracture to heal?
- Will I need surgery?
- Preventing stress fractures
What is a stress fracture?
A stress fracture is a type of bone break or crack in the bone. Stress fractures occur when a small or moderate amount of force is applied to a bone repeatedly and over time. This is different from a traumatic fracture, in which a significant amount of force is applied suddenly, such as in the case of a severe ankle twisting injury, which can cause acute ankle fractures, or in a car collision, when bones in the foot may be broken or crushed).
Stress fractures are common in foot and ankle bones because we continually place force on them by standing, walking, running and jumping. In a stress fracture, the bone breaks but usually does not shift position (become "displaced").
The forces that cause a stress fracture in the foot or ankle are similar to those when you bend a paper clip. If you gently bend a paper clip once, it will not break. But if you continue to bend it back and forth multiple times, the metal becomes weakened (or "fatigued") and eventually breaks. Bones that are subjected to repetitive force can experience a similar type of fatigue called a "stress reaction." This increases the risk that the bone will eventually break, that is, suffer a stress fracture.
Causes of a stress fracture in the foot and ankle
Stress fractures generally occur by one of two ways:
- People with healthy bones overuse the foot and ankle by frequent, repetitive motion. This is particularly the case in athletes who participate in high-impact sports such as running track and field, football, basketball, soccer, tennis, gymnastics or cheerleading.
- People who have very weak bones from a separate, underlying condition (such as osteoporosis) sustain a stress fracture in the foot even from fairly low-impact activities such as frequent walking. This type of stress fracture is called an "insufficiency fracture" because it happens in a bone that does not have "sufficient" density or strength to withstand normal impact forces. Insufficiency fractures can sometimes affect younger, otherwise healthy women who exercise excessively, because such activity can lead to irregular or absent menstrual cycles, which in turn affects the strength of their bones.
The foot and ankle are the most common parts of the body to experience a stress fracture because we are constantly on our feet. Foot and ankle stress fractures often occur in people who begin a new activity that involves any impact of the feet on the ground, such as hiking or running. Stress fractures also occur in people who quickly increase the amount of a certain kind of activity. For example, somebody who normally runs twice a week for 30 minutes who then suddenly begins to run seven days a week for one hour has an increased risk of getting a stress fracture.
Shoes that provide poor support, such as high heels – which place a lot of pressure on the toes – as well as old, stiff shoes can put a person at risk. Finally, people with foot deformities that change their load bearing can develop stress fractures. For example, in a foot with a bunion, the big toe may be repositioned such that stops supporting the weight it should normally should bear. This places more load force on the other toes, which can lead to a stress fracture in one or more of them. In such cases, the second toe (next to the big toe) is the most likely to fracture.
What bones in the foot and ankle are affected by a stress fracture?
Any of the bones of the lower leg, ankle and foot can experience a stress fracture. The most commonly affected bones are:
- The metatarsals, which connect the toes to the midfoot.
- The calcaneus (heel bone).
- The navicular, a bone near the ankle. Navicular stress fractures take a long time to heal.
- The bones that make up the ankle joint – particularly the tibia and fibula.
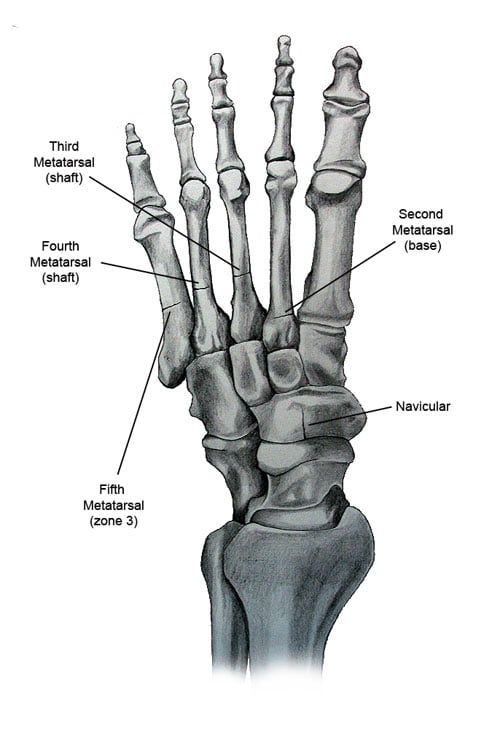
Anatomical drawing of the foot, showing the metatarsal and navicular bones. (Illustration by Joseph Yu, BS.)
What are the symptoms of a stress fracture in the foot and ankle?
The key symptom of a stress fracture is pain. Depending on the bone affected, it tends to hurt in very specific, pinpoint areas, and it will hurt when you touch the exact area where the bone is broken.
If you have recently changed or increased your activity and have pain in a specific area of the foot or ankle, you may have a stress fracture. The pain usually becomes more intense when you do impact activities and gets better during periods of rest.
If you think you may have a stress fracture in your foot or ankle, the most important thing to do is to immediately stop all activities that cause pain. If an untreated stress fracture worsens (gets bigger), you will start feeling the pain more quickly during activity that puts stress on the affected bones than when the stress fracture first appeared.
If your pain continues after several days of rest or if your pain goes away but then returns even after several weeks of rest, you should see an orthopedic foot and ankle surgeon (also called an "orthopedist" or "orthopaedist").
How are stress fractures diagnosed?
Your doctor will first ask you questions about your pain and level of activity to evaluate you for the risk factors discussed above.
Next, he or she will examine you and order X-rays for the area where you experience pain. When a stress fracture is present, it is actually not uncommon for the X-rays to appear normal and show no break in the bone. This is because sometimes the bone reacts and grows new bone to heal the crack. (However, the injured bone is still vulnerable to being rebroken.) When new bone grows, the final step is for it to calcify. A radiologist or orthopedist often confirms the stress fracture diagnosis by seeing the calcification of new bone growth on your X-ray.
In certain cases your doctor may order a bone scan or MRI to provide more information than does a standard X-ray. However, these more expensive tests are not routinely needed to diagnose a stress fracture.
How do you treat a stress fracture?
Most stress fractures will heal on their own if you reduce your level of activity and wear protective footwear for a period of time. As mentioned above, the most important thing to do if you have or think you may have a stress fracture in your foot or ankle, is to cease the activity that caused your problem in the first place. You should stop all high-impact activity for a time, typically for about six weeks.
Icing and elevating the affected leg immediately following a stress fracture can help decrease swelling and pain. As for pain, it is best to take acetaminophen (Tylenol) instead of nonsteroidal anti-inflammatory drugs (NSAIDs ), which includes ibuprofen (Advil) and naproxen (Aleve). This is because some data suggests that taking NSAIDs can reduce the ability of bone to heal.
Your orthopedist may recommend that you wear a stiff-soled shoe, a wooden-soled sandal, or a removable "walking boot," also known as a short leg-fracture brace shoe.
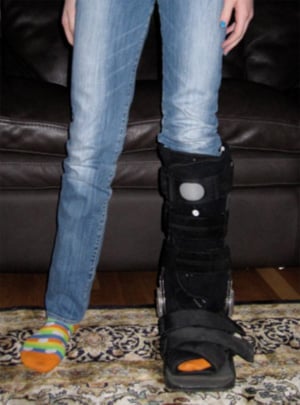
A typical fracture brace or "walking boot" worn to allow a nondisplaced fracture to heal.
How long does it take for a stress fracture to heal?
Many stress fractures of the foot or ankle will heel in 4 to 6 weeks. However, healing times vary, depending on which bone is broken. Some foot bones, such as the navicular or the fifth metatarsal, can take a much longer time to heal than do others.
After weeks of rest, and once the pain is completely gone, you may gradually ease back into physical activity and sports. This gradual reintroduction period should span about 4 to 6 weeks. Switch to a sport that puts less stress on the foot and leg until you have fully recovered. Examples of appropriate low-impact activity include:
- Swimming
- Cycling (bicycle riding or spin classes)
The worst choices for resumed activity while you recover from a foot or ankle stress fracture are running or even walking on hard surfaces. You can easily reopen your fracture and have to begin the recovery process again.
During recovery, wear comfortable, supportive shoes without a raised heel. Footwear should be flexible, not stiff. If you are a runner, after you have resumed low-impact activity for 4 to 6 weeks, begin a conservative jogging regimen. Increase your running mileage very slowly over time. Do not do too much, too soon.
Will I need surgery?
Surgery is rarely needed and is recommended usually only after conservative, nonsurgical approaches above are not working.
Preventing stress fractures
The following principles can help you lead a healthy lifestyle and avoid problems with stress fractures:
- Eat calcium-rich foods and ensure you get enough daily Vitamin D to help maintain bone density.
- Wear good shoes. Do not wear old or stiff shoes, but instead try comfortable, well-padded, and supportive shoes. It is usually a good idea to wear shoes made specifically for the sport you would like to do. Avoid high heels whenever possible.
- Do not smoke. This can lead to problems with healing. It is actually the nicotine that creates the problem, so other gum and products containing nicotine will still prevent the bone from healing.
- Cross-train. This means that you should alternate between activities. For example, you can switch up jogging with swimming or cycling during the week.
- Slowly ease into previous or new sports activities. Gradually increase the time, speed, and distance. Many experts suggest a 10% increase of exercise time per week.









