
Peter Connolly, MD
Vascular Surgeon, Weill Cornell Medicine
This specialty center of excellence at HSS provides integrated care for those faced with a possible amputation or after having already undergone amputation surgery. Our mission is to provide optimal care and achieve the highest level of function and mobility for our patients — whether that is to help prevent a limb from being amputated or to offer the best options for a prosthetic. HSS offers one of the most advanced limb replacement methods at the Osseointegration Limb Replacement Center.
Patient-centered clinical research helps us further advance the care of the individual with a severely compromised limb. We strive to continuously improve and innovate with every patient that we help.
Dr. Rozbruch gives an overview of LSARC and treatment options for patients
Our orthopedic surgeons who specialize in limb salvage surgery and amputation reconstruction surgery will evaluate and work with you to determine the best treatment approach. Focusing on your specific needs, you and your expert surgeon will also interact with other key professionals:
Our team offers integrated care for the patient with a limb at risk or already having undergone an amputation. Our orthopedic surgeons work intimately with other key professionals including certified prosthetists, physical therapists, patient counselors, and psychologists to offer state of the art treatment to our patients. This integrated care begins before surgery and continues until the patient has achieved maximum mobility.

Vascular Surgeon, Weill Cornell Medicine

Plastic Surgeon, Weill Cornell Medicine
Glenn is a graduate of New York University’s Prosthetic and Orthotic Program and is a Certified Prosthetist and Orthotist. He has over 35 years of P&O experience and has been Director of Prosthetics and Orthotics at Hospital for Special Surgery for 27 years. Glenn has advanced training in various types of Scoliosis orthoses, myoelectric prostheses, externally powered orthoses, cranial molding orthoses and microprocessor controlled knee and ankle units. Glenn has been co-investigator on numerous research studies regarding orthotic treatment of osteoarthritis. He has been a guest lecturer at New York University, Hunter College, New York School of Podiatry and numerous New York hospitals. Additionally, he has volunteered extensively at FOCOS Hospital in Pantang, Accra, Ghana and Orthopedic Training Centre in Nsawam, Ghana.
Glenn attended New York University’s Prosthetic and Orthotic program and is a Certified Prosthetist and Orthotist. He is a fellow of the American Academy of Orthotists and Prosthetists, the highest honor bestowed on a practitioner for their education and service to the profession. Glenn has over 35 years of experience as an educator at New York University, Columbia University, and in private practice. Glenn has lectured extensively during his years of practice and has been involved in numerous research programs. He joined the staff at Eschen Prosthetic and Orthotic Laboratories as Director of Prosthetics for their practice. Glenn has advanced training in many aspects of prosthetic care including myoelectrics upper limb, microprocessor knees, and advanced foot designs. He is known for his skills in advanced socket designs and vacuum systems. Glenn has been involved in research and development of improving socket systems over the last 25 years.
Haris was a member of the inaugural class to receive a Master’s degree in Prosthetics and Orthotics from Northwestern University’s Feinberg School of Medicine. While attending Northwestern University, he was part of a small group of students selected to travel to Guatemala and provide orthotic and prosthetic care to underprivileged patients. Haris’s personal story has greatly influenced him to focus on prosthetic care. He started working for Eschen as a dual-discipline resident. He completed his residency, passed his board exams, and is an American Board Certified Prosthetist and Orthotist. He is Eschen’s lead Manhattan Prosthetist and Residency Director. Haris has advanced training in many aspects of prosthetic care including myoelectric upper limb prostheses and microprocessor knee and ankle units. He is committed to helping every patient achieve their maximum functional potential utilizing the latest technology and technique.
Andrew is a graduate of New York University and a Certified Prosthetist and Orthotist with over 35 years of clinical experience. He has been a senior executive for several public and private companies in the orthopedic rehabilitative field. He owned and operated one of the five largest orthotic and prosthetic companies in the United States with 27 locations prior to selling to a national public company. His primary focus has been working with practitioners to deliver clinical excellence and the formation of patient-centric programs which enhance the lives and outcomes of patients. In 2011, Andrew acquired Eschen Prosthetic and Orthotic Laboratories, Inc (“Eschen”), a 94 year old prosthetic and orthotic provider. Eschen has since expanded to 6 locations throughout the New York metropolitan area with additional expansion slated to meet the needs of the marketplace. Eschen is the exclusive provider of orthotic and prosthetic inpatient services at Hospital for Special Surgery.
Dennis became a below-the-knee amputee at age 24 as a result of an automobile accident. Dennis was determined to resume his athletic endeavors and qualified for the 1988 Paralympic Track and Field Team. In Seoul, Korea he set the world record for the 100m event in 11.73 s and won gold medals in the 200- and 400-meter events. Four years later in Barcelona, he set another world record in the long jump and took silver in the 100m. He also brought home medals from the 1996 Atlanta Paralympics.
In 1989, Dennis co-developed the Fitness for Everyone clinic designed to take amputees beyond traditional rehabilitation. This life-changing program has reached more than 15,500 amputee and 65,000 therapists worldwide.
Dennis has served on the board of directors for the American Board for Certification and the O&P Assistance Fund. In 2002, he was named an honorary member of the American Academy of Orthotists and Prosthetists.
Todd became an above-the-knee amputee at the age of 15 as a result of cancer. Determined to regain an active lifestyle, he pursued competitive athletics for the first time in his life. In 1988, Todd qualified for the Paralympic Track and Field Team and won a gold medal by completing the 100m event in a time of 15.77 s. In the 1995 World Games in Germany, he broke his own world record by running the 100m in 14.55 seconds. Todd has competed and medaled at three Paralympic Games.
Along with his athletic endeavors, Todd has worked in the prosthetic community for more than 14 years. He co-created and conducted the Fitness for Everyone clinic series that has changed the lives of thousands of amputees, their families, and rehabilitation professionals worldwide.
Todd has served on the board of directors of the O&P Assistance Fund since 1997. In 2002, he became an Honorary Lifetime member of the American Academy of Orthotists and Prosthetists.
If you have a limb at risk from infection, bone loss, soft-tissue compromise related to trauma, tumor reconstruction, or peripheral vascular disease, we will determine if you are a candidate for limb salvage surgery or amputation reconstruction surgery. Our surgeons are experts in both limb salvage surgery and amputation reconstruction: they will guide you toward the best approach for your needs. After surgery, you will get support and services at HSS.
If you have already had an amputation, we will provide the support you need. This includes prosthetic fitting, physical therapy, psychological support, and the expertise of patient counselors. These counselors are themselves amputees who run walking schools, support groups, and offer individual counseling. If you had an amputation surgery at a different hospital and are having difficulties, we will evaluate you to determine the root of the problem and offer to you the best solution. Osseointegration is an excellent option for select patients who are having difficulty with socket wear.
Surgeon: S. Robert Rozbruch, MD
Prosthetist: Glenn Garrison, CPO
Patient: Chris
Summary
This patient underwent 8 cm lengthening of a dysfunctional very short below knee amputation (BKA) residual limb that was initially 7 cm in length. The lengthening was greater than 100% and resulted in a BKA residual limb of 15 cm. A prosthesis was attached to the circular external fixator allowing the patient to bear weight and walk during the treatment.
Pre-Op
The patient is a 27-year-old male who developed compartment syndrome after trauma 2 years earlier. This led to a BKA done at an outside medical center. The length of the tibial remnant was 7 cm. Although he was able to wear a prosthesis, he had difficulties related to the short residual limb.
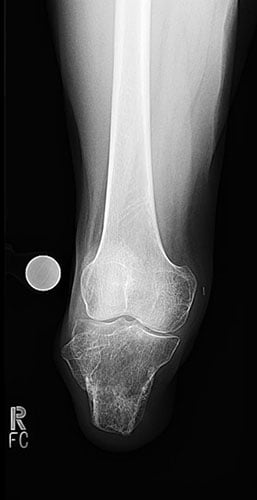
Surgery
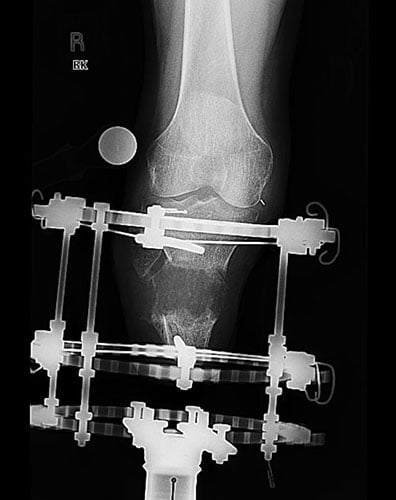
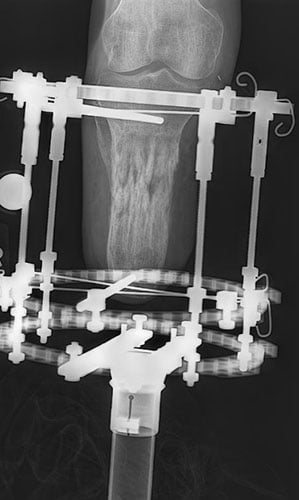
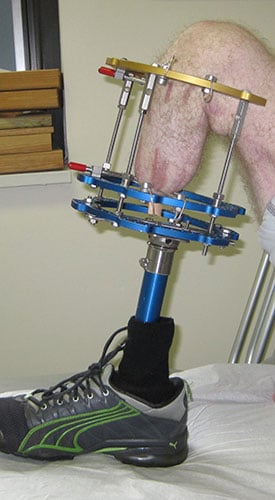
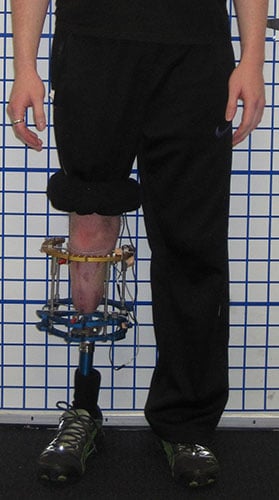
Outcome
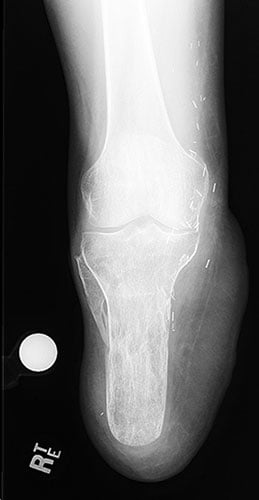
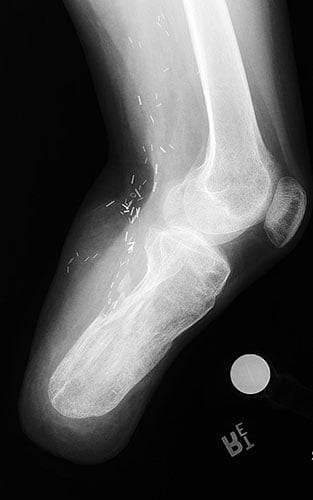
Figures 7A and 7B: AP and lateral x-rays 2 years after surgery. Note the well healed bone 15 cm in length without deformity. Flap coverage was performed by plastic surgeon to improve soft-tissue coverage of the residual limb.
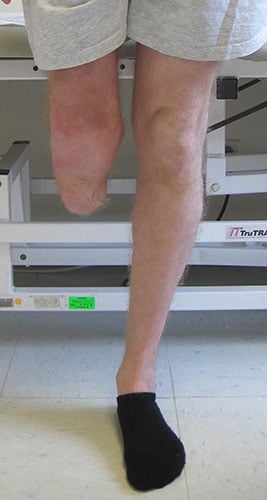
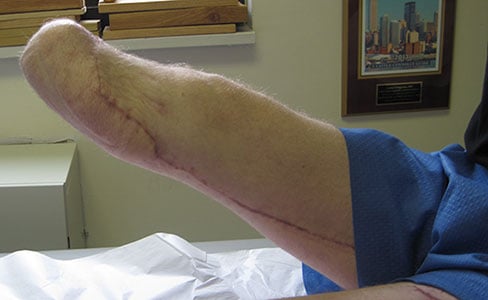
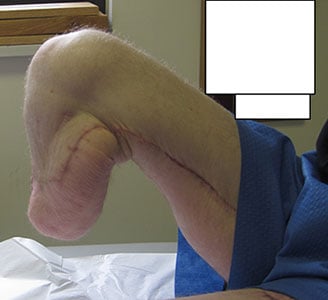
Figures 8A and 8B: Clinical photos showing appearance and length of the residual limb. Prosthetic wear was improved with the lengthened residual leg.
Surgeon: S. Robert Rozbruch, MD
Patient: Angelo
Pre-Op
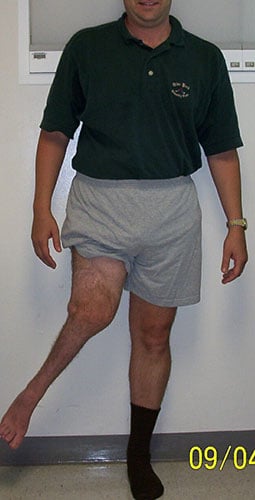
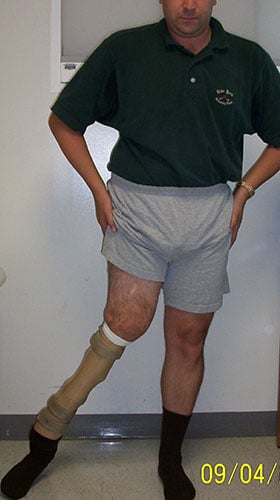
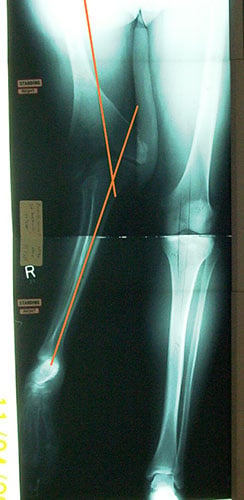
Angelo had massive shortening from a congenital deformity and has worn a prosthesis all his life. However, the valgus deformity of the right limb has made prosthetic wear difficult and has compromised his function. Notice the angular deformity (figure 3) demonstrated by the 2 orange lines.
Surgery
He underwent an osteotomy of the proximal tibia to straighten the leg.
Outcome
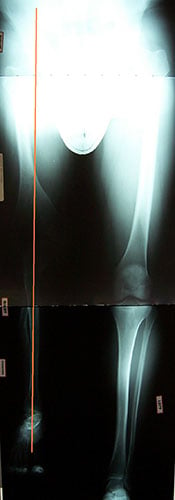
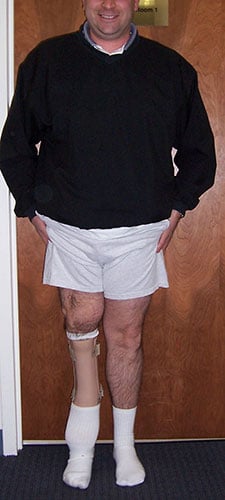
With a straight leg, prosthetic wear, function, and aesthetics have all been improved for Angelo. Notice a straight orange line in Figure 4 representing the mechanical axis of the right lower extremity.
Comparison of Two Patients
Watch the Case Presentation
Patient Surgeon: S. Robert Rozbruch, MD
Watch the Surgical Animation

Case 4
Lengthening and Reconstruction of Short Transfemoral Amputation

Case 5

Case 6
Stoma Care after Osseointegration Amputation Reconstruction Surgery
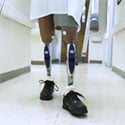
State-of-the-art prosthesis or orthosis to achieve maximum mobility
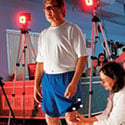
Motion capture technology to drive best results

Regain mobility from people who understand

Limb Lengthening and Complex Reconstruction Service
Specializing in complex procedures to regain mobility

Hand and Upper Extremity Service
Expertise in surgery of the upper extremity
Patient-centered clinical research will help us further advance the care of the individual with a severely compromised limb. Our team is dedicated to finding the best methods and techniques to help our patients through evidence-based research.
This video animation shows an osseointegration amputation reconstruction. For additional videos, click the menu button ![]() in the upper right corner of the video player.
in the upper right corner of the video player.