Oral Concerns in People With Lupus
Dr. Freedman, whose expertise is related to diseases involving the mouth, including autoimmune processes, presented a lecture on the effects of lupus and oral health.
He began by informing the audience that there are three major categories of lesions that occur in the oral cavity of people with lupus:
- direct involvement of the oral cavity by lupus lesions
- Sjogren’s syndrome
- oral effects of lupus medications
What kinds of oral lesions (mouth lesions) can lupus cause?
There are two types of these lesions:
- those that do not correlate with active disease (more frequent)
- those associated with active disease
Therefore, the direct involvement of the oral cavity by lesions of lupus in the mouth may indicate active disease. The only way to reliably distinguish whether or not an oral lesion is associated with active disease is by means of a biopsy.
Oral lesions not associated with active disease occur in up to 40% of people with lupus and are usually a result of a reaction to a drug being used to treat lupus or another condition. They have a non-characteristic coloring of red or white – or both red and white – and are painless.
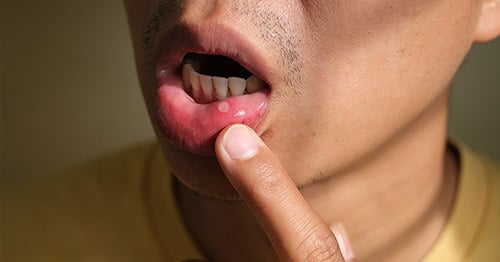
Oral lesions associated with active disease are usually red ulcers surrounded by a white halo and white radiating lines. These are the more typical “discoid” lesions and are only seen in people with active disease, and you should tell your physician as soon as you notice them. These types of lesions, which may or may not be painful, most often occur inside the cheeks, on the hard palate (roof of the mouth), and on the lower lip.
It is essential that you see your dentist and have an oral soft tissue exam regularly. This type of exam takes no longer than three minutes, and you should insist on receiving it during your routine cleaning. This way, your dentist can check for any lesions you may not even be aware you have (particularly if they are painless). Because the only way to reliably determine the true nature of oral lesions is to examine them under a microscope, you should – as mentioned earlier – get biopsies done for any lesions that your dentist may find.
Oral lesions may respond to treatment with topical or intralesional steroids, but antimalarial drugs may be necessary to treat resistant lesions. The control of active systemic disease will usually aid in the control of oral lesions, as well.
Lupus and Sjogren’s syndrome
Sjogren’s syndrome (or Sjogren's disease) is a chronic, systemic autoimmune disease that targets the salivary glands (in the mouth) and lacrimal glands (in the eye). The involvement of these two glands results in dry mouth and dry eyes (sicca complex). There are two forms of Sjogren's:
- the primary disease, which occurs when you experience dry eyes and a dry mouth
- the secondary disease, which occurs when you experience dry eyes, a dry mouth, and another associated autoimmune disease.
People who have both lupus and Sjogren's tend to exhibit fewer systemic manifestations, particularly kidney involvement. Sjogren's occurs in approximately 1% to 3% of the general population, but 20% to 30% of people with lupus. Sjogren's may precede lupus by many years; however, it most often occurs late in the course of lupus.
About one-third to one-half of people with Sjogren's will experience a painless enlargement of a major salivary gland, and this manifestation of the disease is usually bilateral (will occur on both sides). The destruction of the salivary glands by antibodies causes profound oral dryness (xerostomia), which is the most debilitating oral symptom. Loss of saliva results in the loss of the antibacterial and antifungal capacities of saliva. Saliva keeps the oral soft tissue moist and healthy, and buffers the oral environment, helping to neutralize acids that cause dental caries (cavities). Destruction of the salivary glands inhibits that buffering effect. This causes multiple consequences for oral health, such as susceptibility to caries (decay) and oral fungal infections.
Routine and preventative dental care and the use of fluoride treatments to prevent caries is crucial in people with Sjogren's. Otherwise, they may develop rampant decay requiring root canal therapy and crown placement on teeth. Patients who wear dentures may have difficulty keeping their dentures in place due to the poor suction caused by inadequate saliva. Dentures should be cleaned with 2% chlorhexidine (Peridex) and should not be worn overnight in order to prevent fungal infection. People with Sjogren's should try to avoid drugs that dry your mouth – such as anti-histamines, anti-depressants, and decongestants – when possible.
What are the oral effects of medications used in the treatment of lupus?
There are five common categories of drugs used to treat lupus:
- NSAIDs, indlucing COX-2 inhibitors
- antimalarial drugs – hydroxychloroquine or quinacrine
- corticosteroids – prednisone
- immunosuppressive drugs – azathioprine (Imuran), methotrexate, cyclophosphamide (Cytoxan), cyclosporine, mycophenolate mofetal (Cellcept)
- rituximab (Rituxan)
Each of these treatments has the potential to cause oral complications; therefore, such problems should not automatically be assumed to be a direct result of lupus. There are three main categories of reactions to drugs:
- changes in pigment of the lining of the mouth
- drug reaction to medication
- opportunistic oral infection (affecting persons with a compromised immune system) secondary to effect of immunosuppressive medications
Alteration in pigmentation of the lining of the mouth is a common side effect of antimalarial drugs. It manifests itself as an increase in pigmentation, and its most commonly occurs on the palate.
The following drugs most commonly cause oral reaction: NSAIDs and COX-2 inhibitors, antimalarial drugs, calcium channel blockers, ACE inhibitors, cholesterol lowering agents, rituximab, and cyclosporine. These reactions to medication can be classified in four categories:
Erythema multiforme (also known as “Stevens-Johnson Syndrome”) can occur as a reaction to any of the drugs listed above. This is a serious drug reaction, and experienced in a full-blown state can even be life-threatening. Stevens-Johnson Syndrome is an explosive disease, which can develop overnight. It reveals itself as crusting of the lips (usually symmetrical) and as painful ulcerations of the gums, lips, cheeks, tongue. Swollen glands, fever, and genital lesions may also occur. You should contact a doctor as soon as you realize you are having this reaction, or go straight to the emergency room.
Lichenoid drug reactions can be caused by NSAIDS, COX2-inhibitors, antimalarial drugs, calcium channel blockers, ACE inhibitors, or cholesterol lowering agents.
Drug induced gingival hyperplasia can be caused by cyclosporine and calcium channel blockers. Angioedema of the lip can be a secondary reaction to ACE-inhibitors. ACE-inhibitors are used to treat hypertension. This reaction can also be a result of anti-seizure medications and immune-suppressants. It is important to note that you are more susceptible to gingival hyperplasia when your mouth is not clean; therefore, it is very important to have good oral hygiene.
Tongue swelling and lip swelling (angioedema) can be caused by rituximab and ACE inhibitors. Swelling of the tongue is dangerous because it can compromise the airway, whereas swelling of the lip is rather common and not dangerous. Steroids can help moderate both of these reactions.
An opportunistic oral infection can express itself as a secondary effect of immunosuppressive medications (such as azathioprine, Cytoxan, methotrexate, and cyclosporine) and corticosteroids (such as prednisone). This secondary effect only occurs when the body’s immune system is suppressed in such a way that usually harmless organisms cause problems. Anyone taking steroids is susceptible, and there are two ways in which this kind of infection can be expressed. Herpes simplex virus infection occurs in 80-90% of the general public. Most people are unaware that they are infected with Herpes, which is a lifetime infection. Secondary herpetic eruptions occur in 20% of those who have been infected and are most commonly seen as fever blisters, sun sores, etc. Candidiasis – a fungal infection – can develop secondary to dry mouth, diabetes, and dentures. You should see an oral pathologist (a specialist in dental and cavity diseases, not a regular dentist), internist, or dermatologist – as appropriate – to evaluate and treat these oral complications.
Concluding remarks
In Dr. Freedman’s opinion, the literature appears split on preventive antibiotic medication before dental treatment to prevent bacterial endocarditis. Although, approximately half the people with lupus have heart valve abnormalities. In this light, patients should consult their physician about whether antibiotics should be taken before any dental treatment that can cause bleeding. This includes regular cleanings, scaling, periodontal procedures, dental implant placement, root canal treatment, and extractions.
Learn more about the SLE Workshop, a free support and education group held monthly as HSS.
