Managing Arthritis in Lupus
- What is arthritis?
- How common is arthritis?
- How common are the different types of rheumatic disease?
- What is inflammatory arthritis?
- How are different types of arthritis diagnosed?
- What is the distribution of arthritis?
- How do doctors distinguish inflammatory from noninflammatory arthritis?
- What types of arthritis might be present in a person with lupus?
- What is osteoarthritis and why should someone with lupus be concerned about it?
- How is arthritis treated?
- What are some specific approaches to patients with arthritis due to lupus?
- Has treatment progressed for arthritis?
Introduction
Dr. Theodore Fields began his presentation by identifying arthritis as one of the most common symptoms of lupus, with about 90% of patients who have lupus developing arthritis at some point. There are over 100 different types of arthritis, which fall into two main divisions: inflammatory arthritis and noninflammatory arthritis. People with lupus may experience inflammatory arthritis as part of their lupus, but some may also have other common types of noninflammatory arthritis, such as osteoarthritis, which are unrelated to their lupus. If you have lupus and arthritis, it’s important to determine which type of arthritis you have before starting treatment.
What is arthritis?
Arthritis is any condition that causes pain and/or swelling in the joint. Before diagnosing arthritis, a rheumatologist must determine whether the pain is actually in the joint or if it is in the surrounding soft tissues. For example, for someone with shoulder pain, the source of pain may be in a tendon that passes over the shoulder, rather than from inside the joint itself. Once it is determined that the source of the pain is actually the joint, the type of arthritis is then clarified.
As noted, there are two main divisions of arthritis: inflammatory and noninflammatory:
- Inflammatory arthritis, such as lupus arthritis or rheumatoid arthritis (RA), involves soft and spongy swelling of the joint, tenderness and stiffness. The painful swelling that occurs in RA may eventually cause joint deformity and bone erosion.
- The most common noninflammatory arthritis is osteoarthritis. In osteoarthritis, the cartilage wears away and spurs of bone may form. In osteoarthritis of the hand, for example, there is often tenderness and bony enlargement at the knuckles but without the spongy feeling to the touch that would be found in RA.
How common is arthritis?
Arthritis is the leading cause of disability in the United States. Twenty-three percent of the adult population is diagnosed with arthritis, according to the Centers for Disease Control (CDC). The CDC reports that 54 million US adults have arthritis, and 8 million working-age adults report decreased ability to work due to arthritis.*
How common are the different types of rheumatic disease?
"Rheumatic disease" is a broad term that covers conditions characterized by pain, swelling or stiffness in a joint or in the tissues surrounding a joint. Fifty percent of rheumatic diseases are nonarticular disorders (for example, tendonitis and bursitis) that affect multiple areas of the body beyond the joints, such as muscles or tendons. Osteoarthritis is the single most common type of arthritis, making up 30% of all people with rheumatic disease. The remaining 20% of people with rheumatic disease have one of the following:
- Rheumatoid arthritis
- Gout
- Connective tissue diseases (such as lupus)
- Miscellaneous conditions that affect only a small subgroup of patients
What is inflammatory arthritis?
The clinical hallmarks of inflammation include redness, swelling, warmth and pain. If the patient has gout, the joint is very hot and red. In contrast, a person with osteoarthritis, which involves much less inflammation, will not tend to have warmth or redness in the joint, even if some swelling, pain and stiffness are present. For someone with lupus and joint pain, the first question the rheumatologist will consider is whether it represents the inflammatory arthritis that is commonly part of lupus.
How are different types of arthritis diagnosed?
An accurate arthritis diagnosis requires multiple actions and tests:
- A complete review of your medical and symptom history: Your rheumatologist will ask you questions about the degree of stiffness and swelling you experience, which of your joints are involved, whether redness or feelings of warmth have been present, etc.
- A complete physical exam, including detailed joint examination: Your doctor can see whether the joint is hot, tender, red or swollen, as well as whether it has soft or hard enlargement. He or she will also look for any other physical findings that could be a clue to the diagnosis (such as a rash that would be consistent with common lupus symptoms).
- Laboratory studies: Blood tests can show signs of inflammation, anemia or the types of antibodies that can appear in patients with rheumatoid arthritis or lupus. People who have osteoarthritis but no rheumatic disease will have normal laboratory results, while those with inflammatory arthritis, such as lupus, will often have some diagnostic “clues” in their lab results.
- X-rays and/or other diagnostic imaging procedures: Osteoarthritis will often show up on an X-ray, while someone with lupus arthritis will commonly have normal X-rays, since lupus doesn’t tend to cause bone erosion. Rheumatoid arthritis, on the other hand, can show narrowing of the joint and erosion of the underlying bone as the condition progresses. In some cases, ultrasound or MRI imaging can reveal changes in the joint that can’t be seen on X-ray, which can help to define the type of arthritis.
What is the distribution of arthritis?
As mentioned above, the first question a rheumatologist will ask you is whether the pain is actually in the joint or not. If it is in the joint, the distribution of pain offers more information. For example, if a person has either or both of the following, it suggests inflammatory arthritis, such as RA or lupus:
- Swelling in the joints where the bones of the fingers join with the bones of the hand
- Swelling of the entire wrist
Those joints are not usually involved in osteoarthritis. Osteoarthritis tends to occur in some joints where lupus arthritis is not common, such as the finger joints closest to the nails or at the thumb side of the wrist (without involving the whole wrist).
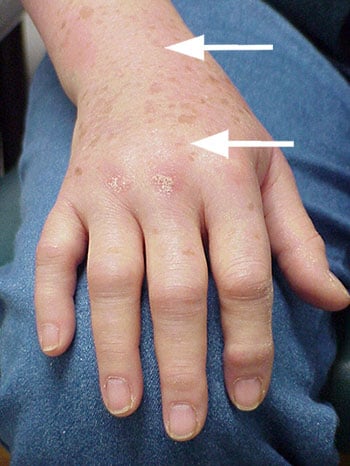
Figure 1: Swelling where the fingers meet the hand, and of the entire wrist (arrows) are clues to an inflammatory type of arthritis, as in lupus or rheumatoid arthritis.
Image courtesy of Theodore Fields, MD.
How do doctors distinguish inflammatory from noninflammatory arthritis?
When we try to make the diagnosis of rheumatoid arthritis or lupus, it is critical that we first identify that there is some form of inflammatory arthritis present. Because osteoarthritis is so much more common than any other type of arthritis, a patient with lupus and joint pain may be found to simply have both lupus and osteoarthritis. There are seven signs that help confirm a diagnosis of inflammatory arthritis:
- When a patient experiences pain and tenderness when we squeeze the hand joints where the fingers meet the hands, as well as the balls of the feet
- Swelling in hand or foot joints, especially at those same joints
- Warmth of joints
- Mild redness over a joint is common in RA or lupus, but not in osteoarthritis (an intensely red joint makes us think of gout or infection)
- Limitation of motion in a joint
- Joint swelling combined with fatigue or low-grade fever
- Morning stiffness that lasts more than half an hour
Laboratory tests, normal in noninflammatory arthritis such as osteoarthritis, can also help confirm a diagnosis in people with inflammatory arthritis.
Rheumatoid factor and anti-Cyclic Citrullinated Peptide (CCP) antibody can be positive in rheumatoid arthritis. ANA (antinuclear antibody) is present in the great majority of lupus patients. Nonspecific tests of inflammation – such as sedimentation rate (also known as erythrocyte sedimentation rate or ESR) and C-reactive protein (CRP) – can be helpful, since they are normal in osteoarthritis but often elevated in rheumatoid arthritis or lupus. People with inflammatory conditions such as RA and lupus can have anemia (low red blood count). A high uric acid level in the blood suggests that a person with an inflammatory arthritis might have gout (if their pattern of arthritis also fits with gout, such as getting intense episodes of pain and swelling and redness at the base of the big toe).
All of these clues help identify people who appear to have inflammatory arthritis. It’s important to determine whether someone with inflammatory arthritis in the hands has lupus or rheumatoid arthritis (some people actually have a crossover of the two).
Both types of arthritis can cause swelling in the hands (see Figure 1), but rheumatoid arthritis tends to cause joint erosion and narrowing, while lupus does not. Both can cause an angulation where the fingers meet the hand, with the fingers angled toward the side of the little finger. In rheumatoid arthritis, that angulation tends to be fixed, but in lupus the fingers generally can be pushed back into place. In lupus, this kind of angulation at the fingers is called Jaccoud’s arthritis; X-rays of this condition tend not to show narrowing or damage in the joint. In rheumatoid arthritis, the X-ray, especially after the condition is present for some time, can show joint damage.
What types of arthritis might be present in a person with lupus?
A person with lupus and joint pain can have any one of these types of arthritis and related conditions:
- Arthritis related to lupus itself – with joint inflammation but no joint erosion
- Osteoarthritis in hands, knees, hips – unrelated to lupus, but so common in the general population that it also occurs in many lupus patients
- Crossover lupus and rheumatoid arthritis with joint erosion (less common)
- Avascular necrosis – joint damage that is often related to prior treatment with steroids, rather than from lupus itself; this is less common but, when present, usually occurs in the hip
- Other types – such as gout, arthritis following an injury, or infectious arthritis. Of the other types, gout is less likely in lupus patients because gout is more common in men while lupus is more common in women. Infectious arthritis is more common in lupus than in the general population because lupus patients with severe disease are often treated with medications that suppress the immune system and increase infection risk.
What is osteoarthritis and why should someone with lupus be concerned about it?
Since osteoarthritis is the single most common type of arthritis, it is not at all rare for someone with an inflammatory condition such as lupus to also have this noninflammatory type of arthritis. In most people, significant osteoarthritis doesn’t start until about age 50, and almost everyone has it in advanced old age.
Osteoarthritis may occur in the fingers or the thumb side of the wrist, as well as in the neck, low back, hips, knees, midfoot and the balls of the foot. Hip osteoarthritis produces pain in the groin because the actual ball and socket of the hip joint is located in the groin.
We try to separate osteoarthritis from lupus arthritis because the treatment plans for inflammatory and noninflammatory arthritis are different.
How is arthritis treated?
Treatment differs according to the type of arthritis the patient is experiencing. Basic measures include physical therapy and exercise, joint protection and splinting. Physical therapists can be very helpful in directing an appropriate exercise program to improve motion of joints and increase strength and stability. It is important to learn movement techniques that protect your joints in order to avoid overstraining joints that are already inflamed. Splints can help ease pain caused by joint inflammation and previous overstraining.
A local steroid injection is another treatment for arthritis. Because the anti-inflammatory steroid medication is in crystalline form, most of it stays in the joint where it is injected. This enhances safety by reducing the effects of the anti-inflammatory steroid on the whole system. A small amount of anti-inflammatory steroid does go into the system after a steroid joint injection, but much less than if the corresponding amount of steroid were taken by mouth. When a small number of joints is involved, such as one knee or one shoulder, a local injection can be an effective treatment with a small chance of side effects.
If the above treatments are not very effective, medicines may be used to treat the joint discomfort. Rheumatologists use analgesics (painkillers) like acetaminophen (Tylenol®), or stronger painkillers such as opioids (codeine and many others). Compared to other medications, acetaminophen appears to have fewer side effects if used in low dose, but for some people it isn’t enough. Opioids can ease pain, but can have problematic side effects, including constipation, lightheadedness and nausea. In higher doses, they can suppress your breathing and be fatal. Due to side effects like these, and the tendency of opioids to be habit-forming, rheumatologists go to great lengths to find treatments for a person’s joint pain that don’t involve the use of opioids.
Another option for treatment of arthritis is the use of nonsteroidal anti-inflammatory drugs (NSAIDs) such as naproxen (Aleve®), ibuprofen (Advil®) or celecoxib (Celebrex®), which now all include heart health warnings on their labels. At least some of the heart health risks of these medications seem related to their side effect of increasing blood pressure, so they are likely of higher risk in patients who hypertension. NSAIDs can also cause ulcers and fluid retention. We try to prescribe these medications in the lowest dose and for the shortest period possible.
For inflammatory arthritis, prednisone may be given. This is an anti-inflammatory drug that is often extremely effective in stopping inflammation, pain and stiffness. Unfortunately, at higher doses, there are many side effects. We try to keep the doses low from the start and taper them whenever possible. If a single joint is inflamed, a local steroid injection may be safer than taking oral prednisone. In people with lupus arthritis who continually need significant doses of oral prednisone to control their arthritis, we consider adding other medications that can allow steroid dose to be decreased, as discussed below.
What are some specific approaches to patients with arthritis due to lupus?
One approach to controlling lupus arthritis is with slow-acting agents such as hydroxychloroquine (Plaquenil®). This medication can help with joint pain and swelling and may also help with the fatigue of lupus. There is evidence that this drug slightly lowers cholesterol as well. Plaquenil is often added in lupus patients with arthritis, as it can help lower the dosage of, or possibly eliminate the use of, prednisone in some patients. Some side effects of Plaquenil are diarrhea, skin rash, sun-sensitivity and, rarely, eye problems (pigment deposits in the back of the eye). Patients taking Plaquenil are checked by an ophthalmologist before starting therapy, and routinely while on the medication. Fortunately, eye problems don’t occur often if the dose is kept within defined limits. Overall, Plaquenil tends to be very well-tolerated in most people.
For the patient with lupus arthritis who does not do well on Plaquenil, stronger agents, such as methotrexate, may be started at a low dose. When a person takes methotrexate, he or she undergoes a series of liver tests to detect any drug-related problem. Methotrexate can make a person fatigued the day after a dose, and it can cause gastrointestinal upset. In general, methotrexate is very well tolerated; however, one should not get pregnant while taking this drug, due to known toxicity to a developing fetus.
If methotrexate is not helpful or well tolerated, there are other options, such as oral azathioprine (Imuran®), oral mycophenolate mofetil (Cellcept®), and intravenous belimumab (Benlysta®). Cellcept and Imuran® are also used for lupus patients with kidney involvement. Benlysta, which also available in a self-injected subcutaneous form, is a newer medication.
More lupus medications are also under active study. For example, an oral medication called baricitinib (Olumiant®) is currently being studied in lupus patients. Many rheumatologists will try methotrexate for lupus arthritis if Plaquenil is not successful. They may consider the other options if methotrexate doesn’t work out. In patients with the crossover type of inflammatory arthritis (which has characteristics of both rheumatoid arthritis and lupus), methotrexate is the likely first agent to be used, since it has been shown to decrease joint damage (which is a risk here because of the rheumatoid arthritis aspect of the joint problem).
Has treatment progressed for arthritis?
Progress is being made in all major types of arthritis. This research is proceeding more quickly in some areas than others. For example, for osteoarthritis, people’s lifestyles have been improved and their pain reduced through advances in injections, medicines and exercises; however, there are no medicines yet that clearly stop the process of osteoarthritis.
For RA, in the last 15 years there have been major advances in management with the development of the “biologic agents,” such as etanercept (Enbrel®) and adalimumab (Humira®). The role of these biologic medications in lupus remains an area of controversy. However, progress in lupus management has been made, and one biologic agent, the previously mentioned belimumab (Benlysta), is now FDA-approved for lupus treatment. For lupus patients, there is much cause for optimism. Lupus is now the focus of clinical trials with a number of medications.
Conclusion
Dr. Fields closed by reminding the group that people with arthritis should be evaluated early in the course of their symptoms. In rheumatoid arthritis, starting treatment early leads to less joint damage down the road. In people with lupus and joint pain, determining what kind of arthritis they have is critical. If classical inflammatory arthritis associated with lupus is found, medications such as Plaquenil can make a difference, and many other options are available. If a lupus patient has a crossover type of lupus arthritis with RA, then methotrexate may prevent joint damage. If a lupus patient turns out to have osteoarthritis as the cause of his or her joint pain, and not the inflammatory arthritis of lupus, then a different approach can be used. That approach focuses on physical therapy, local steroid injection and analgesic medication. Lupus patients with arthritis can take comfort from the recent approval of belimumab (Benlysta), the first new drug approval for lupus in many years, and in knowing that many clinical trials of medications for lupus are now in progress. In the near future, we hope to have even more options for treating the lupus patient with arthritis.
References
* Centers for Disease Control and Prevention Arthritis Factsheet, https://www.cdc.gov/chronicdisease/resources/publications/factsheets/arthritis.htm, accessed April 22, 2019.
About the HSS SLE Workshop
Learn more about the HSS SLE Workshop, a free support and education group held monthly for people with lupus and their families and friends.

