Hip Dysplasia in Adolescents and Young Adults
Introduction
Although chronic hip pain is often associated with aging, the appearance of this symptom in adolescents and young adults may be a sign of hip dysplasia, a condition in which one or more areas of the hip joint have not developed normally.
Anatomy of the hip
The hip is a ball-and-socket joint composed of two bones connected by cartilage, ligaments, tendons and muscles:
- the femoral head or tip of the femur (thighbone) is the ball
- the acetabulum, a cup on the side of the pelvis, is the socket
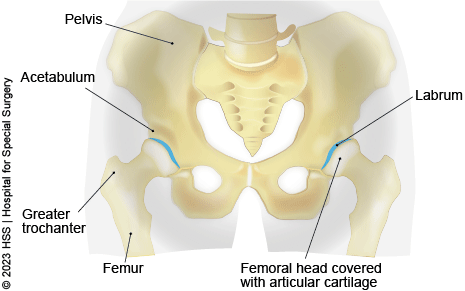
In individuals with hip dysplasia, the acetabulum does not develop fully, making it too shallow to adequately contain and support the femoral head. When this abnormality is present, the ball and socket are misaligned and the labrum can end up bearing the forces that should be distributed throughout the hip. Also, more force is placed on a smaller surface of the hip cartilage and bone, resulting in arthritis over a number of years.
Injury to the labrum and the ligaments that help hold the joint in place can add to the pain and wear and tear on the cartilage. The severity of hip dysplasia can vary considerably from instances in which there is a minor malalignment to a complete dislocation of the femoral head and acetabulum.
Left untreated, hip dysplasia can result in early degenerative changes - the beginnings of osteoarthritis, in which the cartilage wears away and bone rubs against bone. In advanced cases, the patient may require hip replacement.
Causes and Incidence
The cause of abnormal development of the acetabulum is not yet well understood, although there appears to be a relationship between the position of the fetus in the womb, breech births, and a family history of dysplasia. Screening for hip dysplasia (also called pediatric hip dysplasia or developmental hip dysplasia) is routine care for newborns in the United States, but it is impossible to detect all cases of eventual dysplasia in the newborn period. Some of these abnormalities are relatively mild and may not be detected early or cause symptoms until the individual reaches adolescence or later.
A significant number of hip replacements are believed to be the result of untreated hip dysplasia – up to 26%, according to data gathered in the Norwegian Arthroplasty Register over a 10-year period. Some experts believe this figure to be higher.
Although hip dysplasia occurs most frequently on the left side of the body, either one or both hips may be affected. It has recently been shown that the deformity is bilateral (occurring on both sides) in 40% of patients, with varying severity on either side. Hip dysplasia is more common in women than in men, a phenomenon that may be due to anatomical differences in the female pelvis and the tendency for women to have greater laxity (looseness) in their ligaments.
Hip dysplasia can be seen in a wide age range of patients, but adolescents tend to have more severe dysplasia, as the soft tissues surrounding the joint fail earlier.
Diagnosis
In addition to a thorough physical exam and patient history, orthopedists use X-rays, magnetic resonance imaging (MRI), and in some cases, 3-D CT images to confirm a diagnosis of hip dysplasia. The highly sophisticated MRI techniques available at HSS are particularly helpful in providing images that show clear distinction between bone and cartilage and helps to pinpoint the extent of the labral tear if present.
Not infrequently, the damage that is visible on these images does not correspond to the patient’s symptoms; for example, the patient may have considerable damage to the cartilage, but experience very little pain.
Not all labral tears are the result of hip dysplasia. Labral tears of the hip may be secondary to other causes of hip pain, such as femoroacetabular impingement.
Nonsurgical Treatment
Treatment for hip dysplasia focuses on preserving the hip for as long as possible, which is one reason to be evaluated for hip pain promptly. The sooner the orthopedist detects the problem, the more treatment options are available. An initial trial of non-surgical treatment may be appropriate for young adults with either very mild dysplasia or those whose hip dysplasia has resulted in significant damage to the joint and whose only surgical treatment option would be hip replacement.
For those with minimal symptoms and dysplasia, the orthopedist will closely monitor the condition to detect any progression that may warrant treatment.
For both groups of patients, anti-inflammatory medication, steroid injections, specific physical therapy, and use of a cane may help relieve symptoms.
Surgical Treatment
Patients with hip dysplasia who experience pain and have limited damage to their cartilage may be candidates for periacetabular osteotomy (PAO). This procedure involves a series of cuts to the bone to reorient the acetabulum over the femoral head, in order to restore a more normal anatomy. Screws are then placed in the bones to stabilize this position.
View Animation of PAO
In up to 10% of patients the orthopedic surgeon may also perform a femoral osteotomy. Hip arthroscopy may also be performed along with a PAO in selected patients (for example, to repair the labrum).
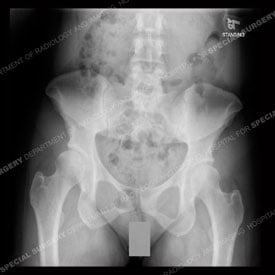
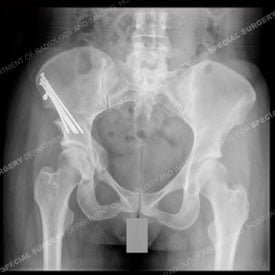
X-ray images of the hip region of a young patient with hip dysplasia (left) corrected with
PAO surgery (right). Note the screws (appearing in white), which are set in place to realign
the acetabulum in a more normal position over the head (top) of the femur (thighbone).
In order to be eligible for PAO, the patient must have reached or be close to reaching skeletal maturity; the low end of the age range is about eleven years. While younger patients tend to have the lowest rate of complications and fastest recovery time, patients up into their early 40s are eligible for PAO provided they meet other criteria (minimal arthritis, good range of motion, and mild symptoms).
Patients in whom cartilage damage is significant and progressive are not good candidates for PAO; initial non-operative treatment and eventual total hip replacement can be an effective alternative. In selected cases, the surgeon uses arthroscopy as an adjunct to PAO. Hip arthroscopy alone is generally not recommended for hip dysplasia with a labral tear, as it can disrupt the ligaments and muscles that surround the hip, further destabilizing the joint.
At HSS, patients who undergo PAO are hospitalized for five to seven days. Following discharge, the patient uses crutches for four to six weeks. Most return to their regular activities by three to six months. In patients with dysplasia in both hips, the surgeries are performed four to six months apart.
Patients with a PAO performed before significant arthritis have very good results even up to 20-25 years after the procedure.[1] “Performed by an experienced orthopedic surgeon, PAO has a good safety profile and produces predictable results,” says Ernest L. Sink, MD, an associate attending orthopedic surgeon at HSS who frequently performs the procedure. “If you are considering undergoing a PAO, it’s important to go to a center where many of these procedures are done.”
Read a case study on Staged Bilateral Periacetabular Osteotomies for the Surgical Treatment of Hip Dysplasia originally featured in the Winter 2012 issue of Grand Rounds from HSS - Management of Complex Cases.
Looking to the Future
In order to build on the body of knowledge about hip dysplasia in young adults, every patient treated at the HSS Center for Hip Preservation is entered into a registry that carefully tracks their progress and the outcome of treatment. Research initiatives are also ongoing at HSS to look at PAO results in high level athletes and how to get them back to sports, to identify new drugs and techniques that can help patients with hip dysplasia.
The hope is that combining medical therapy, specific physical therapy, and hip arthroscopy with a PAO procedure will make treatment even more effective.
References
Reference
1. Steppacher SD, Tannast M, Ganz R, Siebenrock KA. Mean 20-year followup of Bernese periacetabular osteotomy. Clin Orthop Relat Res. 2008; 466:1633-1644.
Further Reading for Medical Professionals
Norwegian Arthroplasty Register: http://www.ncbi.nlm.nih.gov/pubmed/21434808
Burke NG, Devitt BM, Baker JF, Butler JS, Cousins G, McCormack D, O'Byrne JM. Outcome of periacetabular osteotomy for the management of acetabular dysplasia: experience in an academic centre. Acta Orthop Belg. 2011 Feb;77(1):33-40.
Clohisy JC, Barrett SE, Gordon JE, Delgao ED, Schoenecker PL. Periacetabular Osteotomy for the treatment of severe acetabular dysplasia. J Bone Joint Surg Am. 2005; 87: 254-259.
Clohisy JC, Schutz AL, St John L, Schoenecker PL, Wright RW. Periacetabular Osteotomy: A Systematic Review. Clin Orthop Relat Res. (2009) 437: 2041-2052.
Cunningham T, Jessel R, Zurakowski D, Millis MB, Kim YJ. Delayed gadolinium-enhanced magnetic resonance imaging of cartilage to predict early failure of Bernese periacetabular osteotomy for hip dysplasia. J Bone Joint Surg Am. 2006; 88: 1540 – 1548.
Ganz R, Klaue K, Vinh TS, Mast JW. A new periacetabular osteotomy for the treatment of hip dysplasias: technique and preliminary results. Clin Orthop Relat Res. 1988; 232: 26-36.
Matheney T, Kim YJ, Zurakowski D, Matero C, Millis M.Intermediate to long-term results following the bernese periacetabular osteotomy and predictors of clinical outcome: surgical technique. J Bone Joint Surg Am. 2010 Sep;92 Suppl 1 Pt 2:115-29.
Mayo KA, Trumble SJ, Mast JW. Results of periacetabular osteotomy in patients with previous surgery for hip dysplasia. Clin Orthop Relat Res. 1999; 363:73-80.
Schoenecker PL, Clohisy JC, Millis MB, Wenger DR. Surgical management of the problematic hip in adolescent and young adult patients. J Am Acad Orthop Surg. 2011 May;19(5):275-86.
Sucato DJ, Tulchin K, Shrader MW, DeLaRocha A, Gist T, Sheu G. Gait, hip strength and functional outcomes after a Ganz periacetabular osteotomy for adolescent hip dysplasia. J Pediatr Orthop. 2010 Jun;30(4):344-50.
Teratani T, Naito M, Kiyama T, Maeyama A. Periacetabular osteotomy in patients fifty years of age or older: surgical technique. J Bone Joint Surg Am. 2011 Mar;93 Suppl 1:30-9.
Zaltz I, Beaulé P, Clohisy J, Schoenecker P, Sucato D, Podeszwa D, Sierra R, Trousdale R, Kim YJ, Millis MB. Incidence of deep vein thrombosis and pulmonary embolus following periacetabular osteotomy. J Bone Joint Surg Am. 2011 May;93 Suppl 2:62-5.
