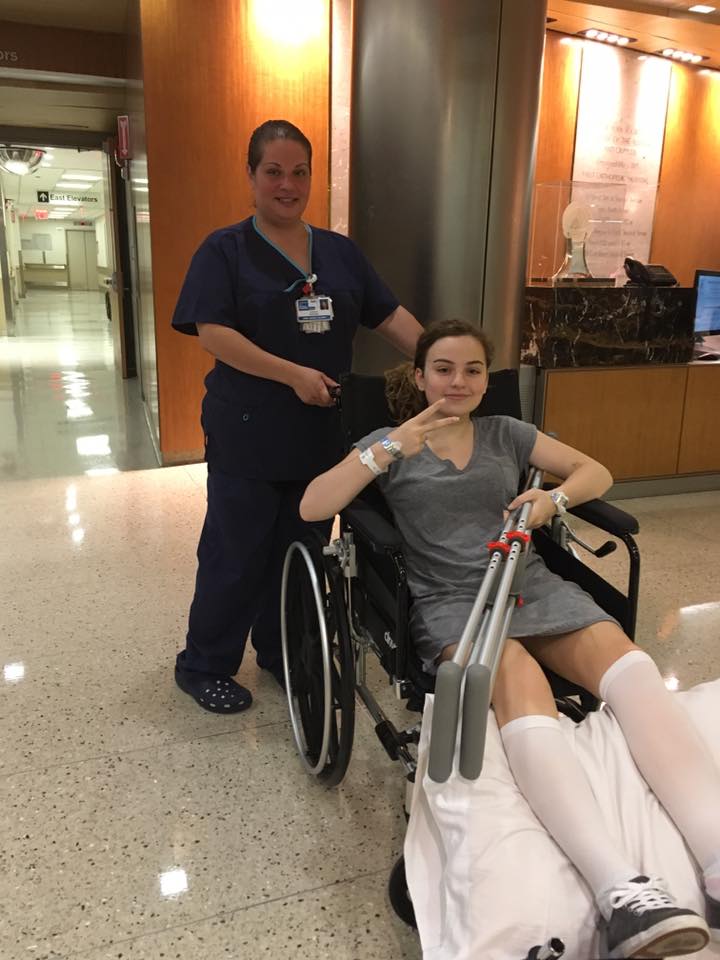- Loading news articles, please wait.

Ernest L. Sink, MD
Physician Profile Page for Ernest L. Sink, MD
 Pediatric Orthopedic and Hip Preservation Surgeon
Pediatric Orthopedic and Hip Preservation Surgeon
About Dr. Sink
Dr. Sink is Chief of the Hip Preservation Service at HSS. He specializes in the treatment of hip disorders, such as hip dysplasia, in patients ranging from newborns to adults. Hip disorders he evaluates are hip dysplasia (DDH) which can affect newborns and adults but also hip pain, labral tears, Perthes disease, and Slipped Capital Femoral Epiphysis (SCFE).
Dr. Sink performs hip preservation procedures in infants, adolescents and adults, including between 80-100 periacetabular osteotomies (PAO) yearly, open hip reductions, osteotomies of the hip, and surgical dislocations. Dr. Sink has authored over 60 peer reviewed articles, and has particular academic and research interest in the outcomes of hip preservation procedures.
Dr. Sink graduated from Texas Southwestern Medical School, where he went on to complete his orthopedic residency training. He completed his fellowship training at Rady Children’s Hospital in San Diego and pursued post-fellowship study of innovative hip procedures in both the United States and Europe. Dr. Sink is involved in teaching other surgeons on a national and international level and collaborates with several other specialized hip surgeons in the country.
Profile Video
Special Expertise
Hip preservation surgery
Hip pain in adolescents and young adults
Hip dysplasia in infants to young adults
Hip osteotomies
Periacetabular osteotomy (PAO)
Surgical hip dislocation
Procedures
Ganz periacetabular osteotomy
Explore Related Patient Stories
View All Patient StoriesVideos



Patient ratings for Dr. Sink
Insurance
If your insurance is not listed, please call our office if you have questions regarding your insurance coverage. If you have out-of-network benefits, then your insurance may reimburse you for a portion of your office visit.
Credentials
Appointments
Chief, Hip Preservation Service, Hospital for Special Surgery
Attending Orthopedic Surgeon, Hospital for Special Surgery
Professor of Clinical Orthopedic Surgery, Weill Cornell Medical College
Associate Attending Orthopedic Surgeon, NewYork-Presbyterian Hospital
Affiliations
American Academy of Orthopaedic SurgeonsPediatric Orthopaedic Surgery of North America
Western Orthopaedic Association
Colorado Orthopaedic Association
Certifications
American Board of Orthopaedic Surgery, 2002Awards
Castle Connolly Top Doctors in New York Metro Area, 2012-2019, 2021, 2022
New York Magazine Top Doctors, 2021, 2022
National expert on hip surgery and hip pain in children and young adults
Teaches hip surgery on a national level
Collaborates with surgeons and centers on outcomes research to study and develop the latest treatments for complex hip disorders
Education
University of Texas Southwestern Medical School, Dallas, TX, 1994
Internship:University of Texas, Dallas, TX, 1994-1995
Residency:University of Texas Southwestern, Dallas, TX, 1995-1999
Fellowship:Pediatric Orthopaedic Surgery, Rady Children's Hospital, San Diego, CA, 1999-2000
AO Fellowship/Apprenticeship Hip Surgery, Bern, Switzerland, Professor R. Ganz, 2004
State Licensure
New York, New Jersey
Languages
EnglishFor My Patients
Patient Forms
Patient Education
- Surgical Dislocation of the Hip Guide
- The Effects of Anesthesia on Children
- Periacetabular Osteotomy (PAO) Information
- PAO Surgery - Frequently Asked Questions

Panel of experts on hip labral tears: What they are and how to treat them
Fracture Care Instructions
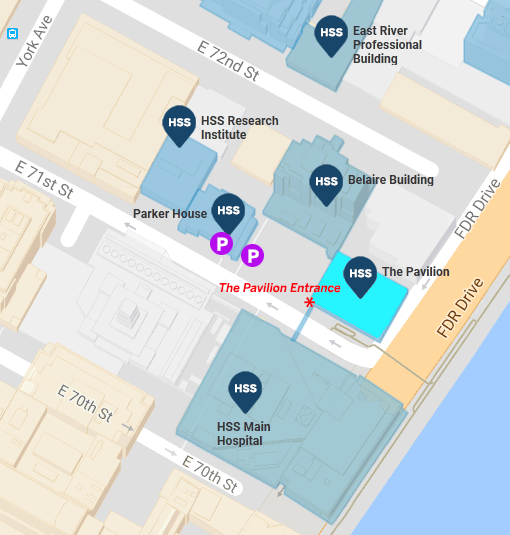
Directions to The Pavilion
My office is located at The Pavilion, 541 East 71st Street. The main entrance to The Pavilion is on the north side of 71st Street underneath the sky bridge that connects the main hospital to the Belaire Building.
Publications by Dr. Sink
Patient Education
Editorial Appointments
Orthopaedics, Editorial Board, 2005-presentPOSNA, Abstract Reviewer for Hip Papers, 2006-2007
Pediatric Orthopaedic Knowledge Update, Lower Extremity Section Editor, 2009-2010
South American Orthopaedic Knowledge Update, Hip Editor, 2009-2010
Selected Journal Articles
Selected Books/Chapters
Sink EL. (Chapter 90) Submuscular Plating of Femoral Shaft Fractures. Edton S, Flynn J (Eds). Operative Techniques in Orthopaedic Surgery. Lippincott Williams & Wilkins, 2007.
Sink EL. (Chapter 91) Open Reduction Internal Fixation of Tibial Tubeosity Fractures. Flynn J (Ed). Operative Techniques in Orthopaedic Surgery. Lippincott Williams & Wilkins, 2007.
Sink EL. (Chapter 7) Submuscular Plating for Pediatric Femur Fractures. Tolo V, Skaggs D (Eds). Master Techniques in Orthopaedic Surgery Pediatrics: Lippincott Williams & Wilkins, 2008.
Sink EL. (Chapter 20) Fractures of the Pelvis. Beaty JH, Kasser JR (Eds). Rockwood & Wilkins’ Fractures in Children. Lippincott Williams & Wilkins, 2008.
Sink EL. (Chapter 30) Submuscular Plating for Pediatric Femur Fractures. Operative Techniques: Pediatric Orthopaedic Surgery. In press 2010.
Sink EL. (Chapter 33) Pediatric Spine and Lower Extremity Fractures. Price C, Flynn J (Eds). Lovell and Winter’s Pediatric Orthopaedics, 7th Edition. Lippincott Williams & Wilkins, In press 2010.
Selected Presentations
'Evaluation of Adolescents for Impingement and Dysplasia.' Nov 28-Dec 2, 2007. IPOS
'Management of 'Late' SCFE Deformities.' Dec 1-5, 2009. IPOS
Sink EL and Dayton M. Femoral-Acetabular Impingement in Adolescents. Podium Presentation, Pediatric Orthopaedic Society of North America, Hollywood, FL, May 2007.
Sink EL and Dayton M. Hip Pathology Recognized During Surgical Dislocation in Chronic SCFE Patients. Podium Presentation, Pediatric Orthopaedic Society of North America, Hollywood, FL, May 2007.
Sink EL. Labral Tears in Adolescent Hips. Instructor, American Academy of Orthopaedic Surgeons, San Francisco, CA, 2008.
Sink EL, Multi-center Evaluation of Early Complications Following Surgical Hip Dislocation. Podium Presentation, American Academy of Orthopaedic Surgeons, Las Vegas, NV, February, 2009.
Clohisy J, Zaltz I, Sucato D, Podszwa D, Trousdale R, Sierra R, Beaule P, Sink, EL, Schoenecker P. Early Complications Associated with the Periacetabular Osteotomy: A Prospective Multicenter Study. Podium Presentation, American Academy of Orthopaedic Surgeons, New Orleans, LA, March, 2010.
Sink, EL, Bravman J. The Predictive Value of Physical Exam, Radiographs, and MRI for Surgical Pathology of Hip Impingement Surgery in the Adolescent Pre-arthritic Hip. Podium Presentation, Pediatric Orthopaedic Society of North America, Waikoloa, HI, May 2010.
Sink, EL, Eliert R. Treatment Outcomes of Femoroacetabular Impingement in Adolescents. Podium Presentation, Western Orthopaedic Association, Monterey, CA, August, 2010.
Sink EL. Children’s Hospital Practice Update: Hip Dysplasia. Podium Presentation, The Children’s Hospital, Denver, CO, 2006.
Agudelo JF, Sink EL, Heare T. Surgical Hip Dislocation for the Treatment of Severe Slipped Capital Femoral Epiphysis: A Preliminary Report. Podium presentation, The Children’s Hospital Annual Orthopedic Day Conference, Aurora, CO, May 2009.
Bravman JT, Sink EL. Predictive Value of Radiographs and MRI for Pathology and Results of Hip Impingement Surgery in Adolescents. Podium Presentation, The Children’s Hospital Annual Orthopedic Day Conference, Aurora, CO, May 2009.
Murray T, Sink EL, Flynn K. Submuscular Plating for Pediatric Femur Fractures Two Year Follow-Up. Podium Presentation, The Children’s Hospital Annual Orthopedic Day Conference, Aurora, CO, May 2009.
Sink EL, Ryba A, Monreal A, Dayton M. Treatment Outcomes of Femoroacetabular Impingement in Adolescent. Podium Presentation, The Children’s Hospital Annual Orthopedic Day Conference, Aurora, CO, April 2010.
Henning AE, Hiza E, Ryba A, Monreal A, Sink EL. The Incidence of Pincer Type Acetabular Morphology on Radiographs in Asymptomatic Adolescent Patients Podium Presentation, The Children’s Hospital Annual Orthopedic Day Conference, Aurora, CO, April 2010.
Research
Treatment outcomes of femoroacetabular impingement in adolescents
Physical exam, radiographs and MRI for predicting surgical pathology of hip
Impingement surgery in the adolescent pre-arthritic hip
Decreased complications of pediatric femur fractures with a change in management.
Evaluating early complications associated with surgical hip dislocation and periacetabular osteotomy
Clinical Trials / Research Studies
Patient Registries
Dr. Sink is a principal investigator for these patient registries .
Industry Relationships
HSS has a long history of supporting appropriate relationships with industry because they advance HSS's mission to provide the highest quality patient care, improve patient mobility, and enhance the quality of life for all, and to advance the science of orthopedic surgery, rheumatology, and their related disciplines through research and education.
Below are the healthcare industry relationships reported by Dr. Sink as of April 22, 2026.
-
Blue Box Docs, LLC - Ownership Interest
- HSS ASC Development Network, LLC - Ownership Interest
- Medacta USA - Consultant
HSS and its physicians make this information available to patients and the public, thus creating a transparent environment for those who are interested in this information. Further, the HSS Conflicts of Interest and Commitment Policy prohibits physicians from collecting royalties on products they develop that are used on patients at HSS. Patients should feel free to ask their HSS physicians questions about these relationships.