Knee Arthritis
Medically reviewed by Lisa A. Mandl, MD, MPH ; Tony S. Shen, MD

Knee pain can be caused by multiple conditions and may not necessarily be arthritis. If you have knee pain or mobility issues, see a specialist to determine whether it may be caused by a simple overuse condition such as runner's knee or whether you are experiencing the onset of osteoarthritis.
Anatomy of the knee
The knee joint can be thought of as a hinge joint, with the primary motion of bending and straightening. In reality, it is more complex than a simple hinge, as these surfaces actually glide and roll upon one another. Three bones meet to form the knee joint: the femur (thighbone), the tibia and the patella (kneecap). The bones are covered with smooth cartilage surfaces that act as a cushion during weightbearing activity.
The bones of the knee are covered with a smooth, glistening layer called articular cartilage and connected by strong ligaments and powerful muscles that are attached to the thigh and calf by tendons, and which provide side-to-side stability. In a healthy knee, all of these structures work together to allow the knee to flex (bend) and extend (straighten) the lower leg smoothly.
The knee can be thought of as having three compartments: the medial (inner), the lateral (outer) and the patellofemoral (where the patella or kneecap meets the femur). In addition, there are two specialized types of cartilage within the knee joint called the lateral and medial meniscus. These act as shock absorbers between the thigh bone and the lower leg bones. Two ligaments – the anterior cruciate ligament (ACL) and the posterior cruciate ligament (PCL) – contribute to the knee's stability.
What is knee arthritis?
Knee arthritis literally means "inflammation of the knee joint," although inflammation is not always present when there is arthritis. On an X-ray of a knee with arthritis, the space between the upper and lower bones is often reduced or, in some places, even absent due to loss of cartilage, the shiny material which covers the ends of the bones.
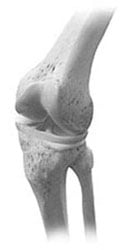
The knee joint
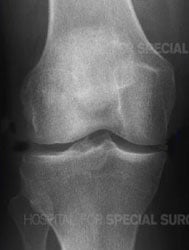
X-ray of a healthy knee joint
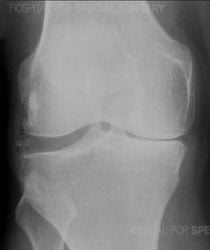
X-ray of an arthritic knee
What causes knee arthritis?
There are two basic types of knee arthritis, and they have separate causes. Osteoarthritis is the most common, and this occurs when the entire knee joint starts to malfunction, due to deterioration of the soft tissues – cartilage, ligaments, tendons, muscle – and the bones themselves. The incidence of osteoarthritis increases with age and is most common among those age 50 and older. Conditions such as rheumatoid arthritis or lupus are autoimmune disorders which can cause inflammatory arthritis. These conditions not only affect the joints but can involve other organs such as the lungs or kidneys, and these can affect people young or old alike.
Osteoarthritis of the knee
People with knee osteoarthritis complain of pain, stiffness, and limited motion in their knee. Although it is most common in older people, younger patients may get post-traumatic arthritis. This is a form of early onset osteoarthritis that results from an injury to the ligaments, cartilage and/or bone in or around a joint. People who are born with abnormalities in the shape of their bones or joints can also have osteoarthritis at earlier ages.
Inflammatory knee arthritis
Various inflammatory disorders can affect the knee joint, including gout, psoriatic arthritis, rheumatoid arthritis, and lupus .
What are the symptoms of knee arthritis?
Symptoms include knee joint aching, stiffness, pain, and mild swelling. These symptoms often lead to reduced activity and muscle weakness. Weakened muscles can lead to instability and decreased ability to control the knee, further limiting the ability to participate in enjoyable activities. The knee joint may develop cysts, bone spurs, or loss of cartilage, which can be seen on X-rays.
Sometimes, people actually feel a catching or clicking within the knee when they bend or flex their knee. Generally, loading the knee joint with activities such as walking long distances, standing for long periods of time, or climbing stairs makes arthritis pain worse. When the arthritis has gotten to be severe, the pain may occur even when sitting, lying down or sleeping. The pain can be felt anywhere around the knee: As the cartilage is worn away preferentially on one side of the knee joint, people may find their knee will become more knock-kneed or bowlegged.
Symptoms of inflammatory arthritis in the knee
Knee arthritis symptoms in cases of inflammatory arthritis can vary. In rheumatoid arthritis, the stiffness is often much worse in the mornings. and gets better as the day goes on. Pain and stiffness can actually improve with activity, which Joints affected by inflammatory arthritis are often much redder and more swollen than joints with osteoarthritis.
What are the risk factors for knee arthritis?
The biggest risk factor for osteoarthritis is getting older. However, it is important to remember that osteoarthritis is not an inevitable part of aging, and the many older people live out their lives without any complaint of knee pain. There is likely a genetic component as well. Other risk factors include weight gain, previous knee injury, as well as poor alignment of the knees, that is, being bowlegged or knock-kneed.
If I have arthritis in one knee, will I get it in the other?
If you have been diagnosed with osteoarthritis, having an affected knee does not mean that you will develop arthritis in the opposite knee. About 40% of patients who have osteoarthritis in one knee will have the same condition in the other knee. In contrast, patients with rheumatoid arthritis often develop problems in both knees.
What type of doctor treats knee arthritis?
Osteoarthritis of the knee may be treated by a sports medicine physician, rheumatologist, or an orthopedic surgeon, depending on your type of arthritis and what kinds of treatment you are looking for. A physical therapist is a crucial team member and should always be consulted to help you reduce pain and increase your mobility. If your knee pain is a result of rheumatoid arthritis, gout or other form of inflammatory arthritis, you should consult a rheumatologist. (Find a doctor who diagnoses and treats knee arthritis.)
How is knee arthritis diagnosed?
An accurate diagnosis for knee arthritis relies on an evaluation and physical exam, laboratory tests, and imaging.
The physical exam
Your doctor will ask about your medical history and symptoms, and then conduct a physical exam to assess:
- your knee pain levels
- range of motion in the knee joint and/or patellofemoral joint
- leg muscle strength
- the presence of any joint swelling or tenderness
- gait (the manner in which you walk)
Radiological examinations
If the physical exam suggests you may have knee osteoarthritis, imaging exams may be used to confirm the diagnosis and rule out other conditions.
Imaging for diagnosing advanced knee osteoarthritis
X-rays are very helpful in diagnosing advanced knee osteoarthritis because the joint will have specific characteristics, including:
- Bones that are closer to each other than they should be: As cartilage wears away, the joint space between them often narrows.
- Cysts: As the body responds to cartilage destruction and attempts to stabilize the joint, cysts or fluid-filled cavities can form in the bone.
- Increased bone density or uneven joints: When bones are no longer cushioned by cartilage, they can rub against one another, creating friction. The body responds by producing more bone tissue, which increases bone density. Increased bone creates uneven joint surfaces and bone spurs at the joint.
Is walking good for knee arthritis?
Yes! Although it may seem counterintuitive, walking can help decrease the pain and stiffness associated with osteoarthritis. In addition, any form of exercise that helps you maintain a healthy weight can reduce the stress on your joints, and this may slow the progression of your arthritis. You should, however, consult a doctor to confirm that your knee pain is caused by osteoarthritis rather than by an injury for which resting would be appropriate. A physical therapist can help determine appropriate levels of exercise for patients with osteoarthritis of the knee.
Are there any exercises that will help my knee arthritis?
Physical therapy should always be a part of the treatment for knee osteoarthritis. In addition, certain exercises such as tai chi, and yoga are low impact and have been found to be particularly helpful in knee arthritis. However, experts agree that the best kind of exercise for knee arthritis is the one that suits your lifestyle and that you can integrate into your daily life! A physical therapist can help you determine the type and amount of exercise which is safe for you.
What is the treatment for knee arthritis?
Nonsurgical approaches to relieving pain and stiffness should always be tried first. These include physical therapy, weight loss, self-management programs and cognitive behavioral therapies. Oral pain medications or periodic injections of corticosteroids into the knee can help decrease pain and improve function. Inflammatory arthritis in the knee is usually managed medically rather than surgically. For patients with severe degeneration of the knee joint due to osteoarthritis, surgical management may be considered. Knee replacement surgery can offer substantial improvement in pain and function to patients who have debilitating pain from severe arthritis.
Nonsurgical treatments for knee arthritis
- Exercise is first line therapy for knee osteoarthritis.
- An assessment by a physical therapist is important to assess what activities can be done safely.
- Low impact exercises such as swimming, water aerobics, walking on a level surface, and using a bicycle are often helpful to improve range of motion and strengthen the muscles.
- Weight loss can also reduce stress on the knee joint.
- The use of supportive devices (cane, brace orthotics) may also be indicated.
- Nonsteroidal anti-inflammatory medication like aspirin, naproxen, or ibuprofen for pain.
- Another class of medications called Cox-2 inhibitors such as celecoxib (Celebrex) can reduce inflammation.
- Injections directly into the knee joint may be recommended. These may provide temporary, symptomatic relief, but are not generally recommended for prolonged use. Your doctor may discuss the effectiveness, risks, and benefits of these different options. Various types of knee injections may be helpful, either alone or in combination, including:
- cortisone injections
- platelet-rich plasma (PRP) injections
- hyaluronic acid injections (also known as viscosupplementation or knee gel shots)
It is difficult to predict the timing and progression of knee arthritis. Sometimes, pain increases and the ability to participate in daily activities decreases despite nonsurgical treatment plans. In those cases, surgery may be recommended.
What is the surgery for knee arthritis?
Although knee replacement for arthritis is the most common and well-known surgery, other procedures may be appropriate for some patients. A knee osteotomy, for example, can help some patients who have a rotational or alignment issue that accelerates the development of osteoarthritis. Others may benefit from a synovectomy and/or some type of knee arthroscopy.
Surgeries for knee arthritis
Various surgeries may be appropriate, either on their own or in combination with another.
- Total or partial knee replacement surgery. The artificial joint replaces the damaged and worn-out cartilage surfaces inside of the knee joint with an artificial joint surface that will be fixed to the bones. Patients with isolated patellofemoral knee arthritis may benefit from patellofemoral joint replacement. This is the most common surgical treatment for severe debilitating knee arthritis.
- Synovectomy – the removal of part of the synovium, the inner lining of the joint capsule – can sometimes be recommended for seriously inflamed knees.
- An osteotomy of the femur and/or tibia – in which bone is cut and realigned – can correctly align the knee to reduce excessive, asymmetrical forces that exacerbate osteoarthritis in one part of the knee. This may be appropriate for people with early onset arthritis caused in part by alignment problems (knock knee, bowleg) or rotational deformities (such as femoral anteversion or femoral retroversion). A person who has a bowleg or knock-knee issue, even if mild, may find their condition becomes more pronounced as knee arthritis advances, since there is greater wearing down of cartilage and bone from one side of the knee as compared to the other.
Learn more from the content below.
Explore Related Patient Stories
View All Patient StoriesReferences
- Bannuru RR, Osani MC, Vaysbrot EE, Arden NK, Bennell K, Bierma-Zeinstra SMA, Kraus VB, Lohmander LS, Abbott JH, Bhandari M, Blanco FJ, Espinosa R, Haugen IK, Lin J, Mandl LA, Moilanen E, Nakamura N, Snyder-Mackler L, Trojian T, Underwood M, McAlindon TE. OARSI guidelines for the non-surgical management of knee, hip, and polyarticular osteoarthritis. Osteoarthritis Cartilage. 2019 Nov;27(11):1578-1589. doi: 10.1016/j.joca.2019.06.011. Epub 2019 Jul 3. PMID: 31278997. https://pubmed.ncbi.nlm.nih.gov/31278997/
- Fibel KH, Hillstrom HJ, Halpern BC. State-of-the-Art management of knee osteoarthritis. World J Clin Cases. 2015 Feb 16;3(2):89-101. doi: 10.12998/wjcc.v3.i2.89. PMID: 25685755; PMCID: PMC4317618. https://pubmed.ncbi.nlm.nih.gov/25685755/
- Kon E, Di Matteo B, Delgado D, Cole BJ, Dorotei A, Dragoo JL, Filardo G, Fortier LA, Giuffrida A, Jo CH, Magalon J, Malanga GA, Mishra A, Nakamura N, Rodeo SA, Sampson S, Sánchez M. Platelet-rich plasma for the treatment of knee osteoarthritis: an expert opinion and proposal for a novel classification and coding system. Expert Opin Biol Ther. 2020 Dec;20(12):1447-1460. doi: 10.1080/14712598.2020.1798925. Epub 2020 Sep 3. PMID: 32692595. https://pubmed.ncbi.nlm.nih.gov/32692595/
- Kulm S, Kolin DA, Langhans MT, Kaidi AC, Elemento O, Bostrom MP, Shen TS. Characterization of Genetic Risk of End-Stage Knee Osteoarthritis Treated with Total Knee Arthroplasty: A Genome-Wide Association Study. J Bone Joint Surg Am. 2022 Oct 199;104(20):1814-1820. PMID: 36000784. https://pubmed.ncbi.nlm.nih.gov/36000784/
- Oeding JF, Varady NH, Fearington FW, Pareek A, Strickland SM, Nwachukwu BU, Camp CL, Krych AJ. Platelet-Rich Plasma Versus Alternative Injections for Osteoarthritis of the Knee: A Systematic Review and Statistical Fragility Index-Based Meta-analysis of Randomized Controlled Trials. Am J Sports Med. 2024 Oct;52(12):3147-3160. doi: 10.1177/03635465231224463. Epub 2024 Feb 29. PMID: 38420745. https://pubmed.ncbi.nlm.nih.gov/38420745/
- Ranawat A, Guo K, Phillips M, Guo A, Niazi F, Bhandari M, Waterman B. Health Economic Assessments of Hyaluronic Acid Treatments for Knee Osteoarthritis: A Systematic Review. Adv Ther. 2024 Jan;41(1):65-81. doi: 10.1007/s12325-023-02691-y. Epub 2023 Oct 30. PMID: 37899384. https://pubmed.ncbi.nlm.nih.gov/37899384/