- Loading news articles, please wait.
About Dr. Cunningham
Dr. Matthew E. Cunningham is an Associate Professor of Orthopedic Surgery at Weill Cornell Medical College. He has clinical interest in thoracic and lumbar spine care, including spinal deformity (scoliosis, flatback, kyphosis, and spondylolisthesis) for adult and pediatric patients, and degenerative problems (stenosis, herniated discs, arthritis, instability) in adults. In consideration of each and every patient, he focuses on the discovery and refinement of less-invasive, less-painful, and less-disruptive ways to correct spinal pathology. This includes surgical solutions for acute spine problems (herniated discs, pinched nerves, radiculopathy) and chronic/degenerative problems (stenosis, spine arthritis, disc herniations, and spinal deformity).
With young scoliosis patients, Dr. Cunningham is sensitive to the need to maintain a normal child’s life as much as possible and works to minimize treatment and avoid surgery wherever other therapies promise success. With adult patients, he incorporates new, less-invasive techniques for surgery that result in smaller incisions, less pain, less abdominal disturbance, and reduced recovery time. Dr. Cunningham runs a basic science research lab, working on a spinal fusion technique that would eliminate surgery altogether, using an innovative injection instead. He also conducts clinical research and participates in two multi-center study groups to improve outcomes in pediatric (CSSG) and adult (ISSG) spine deformity surgical patients.
Currently, he is a volunteer surgeon for the Foundation for Orthopaedics and Complex Spine (FOCOS), a role which has taken him to countries such as Ghana and Sierra Leone in Africa, and Barbados in the West Indies, to provide surgical and non-surgical care to these underserved peoples.
Dr. Cunningham’s background is studded with academic honors and sports. He studied Biophysics at Johns Hopkins University and was recognized with several academic honors including induction into Phi Beta Kappa and being a Rhodes Scholar regional finalist. Throughout his years at Johns Hopkins, he competed in both varsity wrestling and football and was active on the University’s club rugby team. When not in the classroom or on the athletic field, he worked as a lifeguard captain at Seven Presidents Oceanfront Park in Long Branch, NJ.
After graduating from Johns Hopkins, Dr. Cunningham attended Columbia University for both graduate and medical school. While there, he was a student with the National Institute of Health-funded Medical Scientist Training Program (MSTP) and was recognized with many academic honors including induction into Alpha Omega Alpha and receiving the Alfred E. Steiner Research Award, the Dean’s Award for Excellence in Research, and the Miriam Berkman Spotnitz Award. Dr. Cunningham was also recognized for his clinical excellence, winning the Virginia P. Apgar and New York Orthopaedic Hospital Awards.
Throughout his medical studies, Dr. Cunningham remained active in sports; he competed in lifeguard relays with the Borough of Bradley Beach, remained highly involved with Columbia’s 'P&S' Rugby Club, and completed two New York City marathons.
Profile Video
Special Expertise
Adult and pediatric scoliosis, kyphosis, spondylolisthesis, spondylolysis, and other spinal deformities
Complex multiplanar spinal deformity: anterior and/or posterior approaches, osteotomies, and vertebrectomy
Lumbar spine degenerative disease and arthritis: minimally invasive anterior fusion, posterior instrumental fusion
Spondylolisthesis, lumbar spine stenosis and instability: direct an indirect decompression, alignment reduction, sacral transfixation
Surgical solutions for sciatica-type pain and weakness: microdiscectomy, laminectomy, decompression
Procedures
Adult and pediatric anterior and/or posterior spinal fusions for surgical treatment of scoliosis, kyphosis, and spinal deformity
Thoracoplasty, osteotomy, vertebrectomy, posterior vertebral column resection for complex spinal deformity reconstruction
Anterior and/or posterior surgery for stenosis, herniated discs, degenerative disease, and arthritis, including decompression and/or fusion
Posterior lumbar microdiskectomy for herniated discs; posterior lumbar decompression for stenosis; anterior lumbar interbody fusion (ALIF), lateral access lumbar interbody fusion (LLIF) posterior or transforaminal lumbar interbody fusion (PLIF/TLIF), and posterolateral instrumented lumbar fusions for instability and end-stage arthritis of the spine
Explore Related Patient Stories
View All Patient StoriesPatient ratings for Dr. Cunningham
Insurance
If your insurance is not listed, please call our office if you have questions regarding your insurance coverage. If you have out-of-network benefits, then your insurance may reimburse you for a portion of your office visit.
Credentials
Appointments
Attending Orthopedic Surgeon, Hospital for Special Surgery
Associate Scientist on the Clinical Scientist Track, Research Division, Hospital for Special Surgery
Associate Attending Orthopedic Surgeon, New York-Presbyterian Hospital
Associate Professor of Orthopedic Surgery, Weill Cornell Medical College
Affiliations
Volunteer Surgeon, Foundation for Orthopaedics and Complex Spine
Member, North American Spine Society
Member, American Academy of Orthopaedic Surgeons
Candidate Fellow, Scoliosis Research Society
Active Member, Orthopaedic Research Society
Complex Spine Study Group, Adolescent Subgroup
International Spine Study Group
Certifications
Board Certified, American Board of Orthopaedic Surgery
Awards
North American Spine Society Young Investigator Research Grant Award
Philip D. Wilson Award for Excellence in Orthopaedic Surgery Research, Hospital for Special Surgery
Orthopaedic Fellowship Award, New York Chapter of the Arthritis Foundation
Emerging Leader Program, American Orthopaedic Association
Clinician Scientist Development Program, AAOS/OREF/ORS
New York Orthopedic Hospital Award for Outstanding Research & Clinical Performance, College of Physicians and Surgeons, Columbia University
Education
Medical: Columbia University College of Physicians and Surgeons, New York, 2000
Internship: New York Hospital, Weill Cornell Medical College, New York, 2000-2001
Residency: Hospital for Special Surgery, New York, 2001-2005
Fellowship: Hospital for Special Surgery, New York, 2005-2007
State Licensure
New York
Languages
EnglishFor My Patients
Directions and HSS Visitor Information
Patient Information
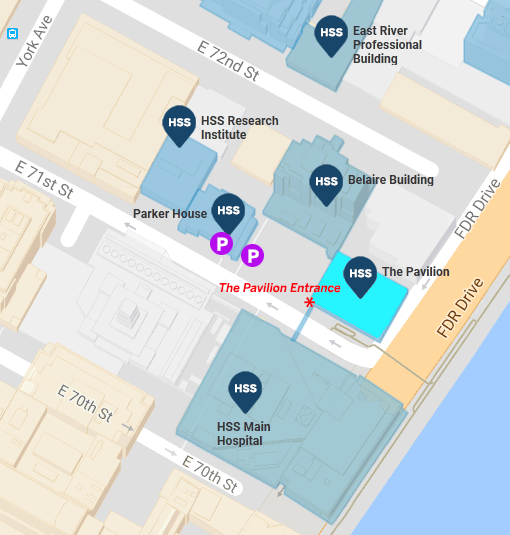
Directions to The Pavilion
My office is located at The Pavilion, 541 East 71st Street. The main entrance to The Pavilion is on the north side of 71st Street underneath the sky bridge that connects the main hospital to the Belaire Building.
Publications by Dr. Cunningham
Patient Education
Editorial Appointments
Clinical Orthopaedics & Related Research, reviewer
Hospital for Special Surgery Journal, reviewer
Journal of Orthopaedic Research, reviewer
Arthritis Research & Therapy Journal, reviewer
Scoliosis, reviewer
Biochemistry, reviewer
Selected Journal Articles
Selected Books/Chapters
Cunningham ME, Kitajewsi J, Greene LA. Efficient Stable Transfection of Pheochromocytoma (PC12) Cells Using a Recombinant Retrovirus (LNC). In: Rush RA & Walker JM (eds): Neurotrophin and Receptor Methods and Protocols: Methods in Molecular Biology. Clifton, NJ, Humana Press; 2001: 135-147.
Cunningham ME, Frelinghuysen PHB, Roh JS, Boachie-Adjei O, Green, DW. Fusionless scoliosis surgery. Curr Opin Pediatr 2005;17(1): 48-53.
Teng KK, Angelastro JM, Cunningham ME, Greene LA. Cultured PC12 Cells: A Model for Neuronal Function, Differentiation and Survival. In: Colin JE (ed): Cell Biology: A Laboratory Handbook, Third Edition. Orlando, FL, Academic Press; 2006: 171-176.
Cunningham ME, Bomback D, Boachie-Adjei O. Revision Deformity Surgery. In Errico, Lonner, and Moulten (eds.): Surgical Management of Spinal Deformities. Philadelphia, PA, Saunders/Elsevier: 2009: 399-417.
Kim HJ, Cunningham ME, Boachie-Adjei O. Revision Spine Surgery to Manage Pediatric Deformity. J Am Acad Ortho Surgery 2010; 18(12): 739-48.
Boachie-Adjei O, and Cunningham ME. Revision Spine Surgery in the Growing Child. In Akbarnia BA, Tazici M, Thompson GH (eds): The Growing spine: Management of Spinal Disorders in Young Children. Berlin, Germany, Springer-Verlag; 2011: 487-97.
Mo F and Cunningham ME. Pediatric Scoliosis. Curr Rev Musculoskelet Med 2011; 4(4): 175-82.
Cunningham ME and Boachie-Adjei O. Revision Surgeries for Adult Spinal Deformity. In Bridwell, K.H. and Dewald R.L. (eds.): The Textbook of Spinal Surgery, 3rd Edition. Philadelphia, PA, Lippincott Williams & Wilkins: 2011: 970-981.
Cunningham ME. Adult Spinal Deformity Surgery. Curr Orthop Pract 2012; e-Pub ahead of print: April 10, 2012.
Hirsch BP, Unnanuntana A, Cunningham ME, Lane JM. The Effect of Therapies for Osteoporosis on Spine Fusion: A Systematic Review. Spine Journal 2012 (in press).
Selected Presentations
Sheela D, Rosenberg TJ, Rawlins BA, Hidaka C, Ronald C, Boachie-Adjei O, Cunningham ME. Gene-Delivery Induced Intervertebral Disk Neoangiogenesis and Anterior Spine Fusion. (ORS Annual Meeting, Long Beach, CA, January 2011.)
Sheela D, Cunningham ME. Intervertebral Disk Organ Culture System: A Pilot Study Assessing In Situ Cell Viability. (ORS Annual Meeting, Long Beach, CA, January 2011.)
Kim HJ, Cunningham ME, Boatey J, Wright B, Mendelow MJ, Hess WF, Paonessa KJ, King AB, Yagi M, Boachie-Adjei O. (CSSG, FOCOS) Infection Rates for Spine Surgery in Underserved and Underdeveloped Nations: A Review of a Consecutive Series in a SRS Global Outreach Program in Africa. (IMAST Annual Meeting, Copenhagen, Denmark, July 2011.)
Yagi M, King AB, Cunningham ME, Boachie-Adjei O. Clinical and radiographic Outcomes of Pedicle Subtraction Osteotomy (PSO) for Fixed Adult Sagittal Imbalance: Does Level of Proximal Fusion Affect Outcome? (Podium/paper #18, SRS Annual Meeting, Louisville, KY. September 2011.)
Cunningham ME. Percutaneous Gene-Delivery Mediated Intervertebral Body Fusion. (NASS Annual Meeting, Chicago, IL, November 2011.)
Research
Molecular cellular biology aspects of bone formation and spinal fusion success.
Adapting gene-therapy and gene-delivery technology for minimally invasive or percutaneous spinal fusions
Development of comparative models to study and perfect spinal fusions and fracture care
Prospective clinical outcomes assessment in complex spinal surgery, with emphasis on development of evidence based medicine
Long term assessments of post-surgical complex spinal surgery patients, with emphasis on complication risk factors and techniques for avoidance
Clinical Trials / Research Studies
Industry Relationships
HSS has a long history of supporting appropriate relationships with industry because they advance HSS's mission to provide the highest quality patient care, improve patient mobility, and enhance the quality of life for all, and to advance the science of orthopedic surgery, rheumatology, and their related disciplines through research and education.
Below are the healthcare industry relationships reported by Dr. Cunningham as of January 8, 2026.
- Better PT - Inventor; Board of Trustees
- Joint Effort Administrative Services Organization, LLC (“JEASO”) - Ownership Interest- (Through JEASO- de minimis owner of the Recovery Shop)
- Medical Education Resources, LLC - Honoraria
- Sustain Surgical - Ownership Interest
HSS and its physicians make this information available to patients and the public, thus creating a transparent environment for those who are interested in this information. Further, the HSS Conflicts of Interest and Commitment Policy prohibits physicians from collecting royalties on products they develop that are used on patients at HSS. Patients should feel free to ask their HSS physicians questions about these relationships.











