Osteochondroma: Types, Causes, Symptoms and Treatments
Benign bone tumors are not life-threatening, and some do not need to be treated at all. Tumors that cause pain, mobility or other problems, however, require intervention to resolve. HSS physicians treat a range of noncancerous bone tumors with and without surgery, including osteochondromas.
What is osteochondroma?
An osteochondroma, also known as an osteocartilaginous exostosis, is one of the most common benign bone tumors. This type of tumor is continuous with the underlying bone − meaning that both the tumor and healthy bone share the same hollow cavity that contains the bone marrow. It grows away from the growth plate during development to form stalks of bone that are covered with a cartilage cap and a bursa (fluid sac).
A growth plate, also called a physis or physeal plate, is a section of cartilage located at the ends of the long bones. This cartilage continually grows and calcifies to add bone length and breadth in growing children and adolescents. Once a person has reached skeletal maturity, these plates close or fuse to form solid bone.
What are the types of osteochondroma?
Osteochondromas can be solitary, meaning there is only one in the body, or multiple. Cases of multiple tumors are usually associated with a genetic syndrome that runs in families called multiple hereditary exostosis (MHE, and also called hereditary multiple osteochondromas). Like a singular (solitary) osteochondroma, MHEs are all continuous with the underlying bone and end with a cartilage cap and bursa.
Osteochondromas, whether single or multiple, can be described as pedunculated (a narrow stalk of bone), or sessile (broad base of bone).
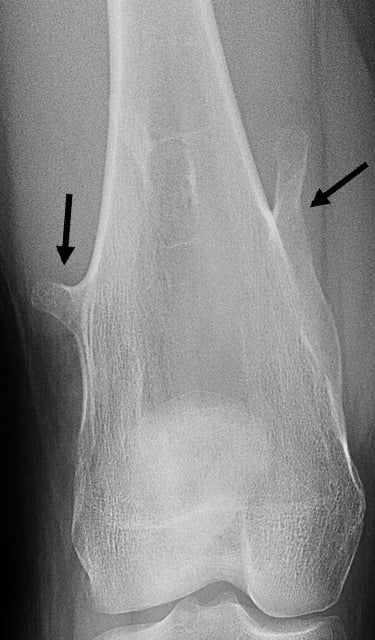
Anteroposterior (Front-to-back) X-ray image showing multiple, pedunculated osteochondromas on a femur.
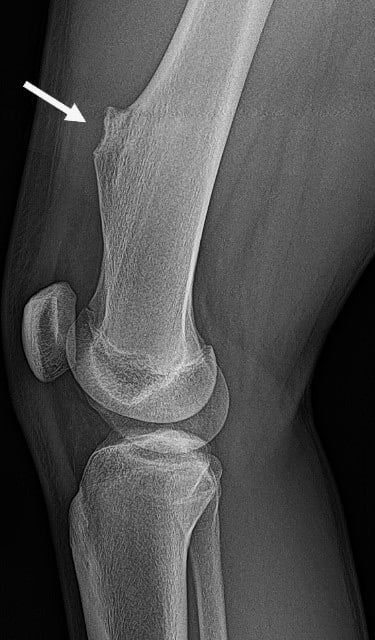
Medial (side-view) X-ray image of a solitary, sessile osteochondroma on the lower portion of the femur, not far above the kneecap.
What causes osteochondroma?
An osteochondroma most commonly forms when the normal function of the EXT-1 of EXT-2 gene (which encodes a specific protein) is disturbed. The normal signaling pathways within the cartilage cells around the growth plate are disrupted. This leads to the growth of a portion of cartilage in an atypical direction. This growth can stop before or at the end of a young person’s normal skeletal development, when the typical growth signals within the body cease.
Is solitary osteochondroma genetic?
Solitary osteochondromas most commonly contain changes in a single gene called EXT-1, which leads to growth of the cartilage cap and formation of bone. This change can occur during growth by way of a random mutation, so the change does not affect the rest of the body or the person’s family.
Conversely, the changes in the EXT-1 and EXT-2 genes associated with multiple hereditary exostosis are passed down in parents’ DNA during conception and thus affect all the cells of an individual, so it is common to develop multiple osteochondromas in the body as a child or adolescent grows.
Is an osteochondroma serious?
Solitary osteochondromas can be monitored without surgery if there is no pain or limitation in function. If pain is persistent or joint motion is affected, surgery to remove the osteochondroma is usually safe, with little risk of complications. Multiple osteochondromas are more likely to lead to inhibition of the growth plate, which can lead to limb deformity or shortening (such as a leg length discrepancy) during childhood and adolescence. Surgery is usually undertaken to prevent severe deformity and assist the limb in growing normally. (Find a doctor at HSS who treats osteochondroma.)
Can an osteochondroma become cancerous?
The vast majority of osteochondromas stop growing after adolescence and remain stable. However, there is a small risk (approximately 5% but likely greater in those with multiple osteochondromas), that the cartilage portion develops into a chondrosarcoma, which is a form of cancer. Thus, any growth of an osteochondroma as an adult warrants evaluation, and osteochondromas of the pelvis, spine, or scapula (shoulder blade) that are difficult to monitor should be routinely imaged to confirm that the tumors remain stable and show no change in size or appearance.
HSS treats cancerous bone tumors such as osteosarcoma and metastatic bone disease, as well as benign tumors.
What is the prognosis for an osteochondroma?
Most osteochondromas can simply be monitored over time if they do not lead to symptoms. In a small percentage (less than 5%), the tumor’s cartilage cap may start to grow and form a cancer, which is usually not an aggressive type but warrants removal regardless. In patients with osteochondromas in the pelvis, or other locations hard to monitor with physical exam, radiographic follow-up is recommended to monitor for growth.
What are the symptoms of an osteochondroma?
Osteochondromas are often discovered as a painless firm mass adjacent to a bone, most commonly around the knee, but almost all bones can be affected. They can be painful when the fluid sac that covers the osteochondroma (called a bursa) becomes inflamed or if it irritates a nearby tendon during normal motion of a joint. A sharp change in pain can occur if the stalk of the osteochondroma fractures. They can also be completely asymptomatic and discovered on X-rays obtained for other reasons.
What parts of the body are usually affected by osteochondroma?
Solitary osteochondromas are most commonly discovered around the knee or the shoulder, but they can be found in most bones of the arms, legs, pelvis, spine and ribs. The facial bones are spared. In multiple hereditary exostosis, the forearms are most commonly involved, along with the area around the knee.
Do osteochondromas stop growing?
Yes, once the signals for normal growth end during adolescence, osteochondromas also stop growing. Ongoing growth or growth in adulthood should be evaluated by a physician, as it could represent an osteochondroma that has turned cancerous.
How is an osteochondroma diagnosed?
An osteochondroma is often suspected during a physical exam when a firm mass is discovered near a joint and it cannot be moved when palpated (examined through touch) by the doctor. The diagnosis can be made with an X-ray if the osteochondroma has the classic stalk appearance, but sessile or broad based osteochondromas may also need a CT scan or MRI to confirm the diagnosis. Continuity with the underlying bone (where the tumor and healthy bone share the medullary cavity that houses the marrow) is the hallmark for diagnosis of an osteochondroma.
How is an osteochondroma treated?
Most osteochondromas are monitored without surgery if discovered as a child or early adolescent, because removal can damage the growth plate, or the osteochondroma can recur with further growth. As a teenager or adult, if the osteochondroma leads to pain, restricted joint motion, or is in an inconvenient location for clothing or shoe wear, the osteochondroma can be removed surgically. If multiple osteochondromas are affecting growth and leading to deformity, surgical treatment may be pursued earlier in life. There is no medication for osteochondroma.
Should you remove an osteochondroma?
If an osteochondroma is not causing any symptoms, it is safe to observe in the majority of cases. An osteochondroma that leads to deformity as a child or continues to grow as an adult should be evaluated for removal. If an osteochondroma starts causing pain or fractures, patients may opt for removal.
What is the surgery for osteochondroma?
Surgery for osteochondroma removes the stalk of bone, cartilage cap, and any overlying bursa (fluid sac) associated with the mass. Complete removal of the cartilage cap prevents recurrence of the mass and eliminates the risk of developing a malignancy in the cartilage cap in the future. The incision is made large enough to safely visualize the base of the mass. The outcome of surgery should include relief of pain and better movement of the adjacent joint.
If the osteochondroma is causing deformity of the adjacent joint (such as knock knee condition), leg length discrepancy or other problem, additional procedures to address the deformity may be performed at the time the tumor is removed.*
How long is the recovery from osteochondroma surgery?
The recovery for a small osteochondroma excision (surgical removal) is brief − around two weeks for the swelling to subside and the incision to heal. For larger osteochondromas that require a larger incision and more surgical exposure, the recovery may be longer, four to six weeks, and may include use of crutches. Generally, patients make a full recovery after surgery.
If correction of deformity is included as part of surgery, the recovery may take several months depending on the specifics of the surgery and should be discussed with your physician.
References
- Reif TJ, Matthias J, Fragomen AT, Rozbruch SR. Limb Length Discrepancy and Angular Deformity due to Benign Bone Tumors and Tumor-like Lesions. J Am Acad Orthop Surg Glob Res Rev. 2021 Mar 10;5(3):e00214. doi: 10.5435/JAAOSGlobal-D-20-00214. PMID: 33720060; PMCID: PMC7954373.