Lupus Brain Fog: Changes in Memory and Thinking
The evolving understanding of brain fog in lupus
In the 1960s, all of the brain symptoms associated with lupus (also known as systemic lupus erythematosus or SLE), including dysfunctions in thinking and memory, seizures, strokes, and psychoses, were considered to be different presentations of a single condition called central nervous system lupus, or CNS SLE. At that time, lupus was thought to affect everyone in the same way with regard to brain health and function.
Then, in the late 1970s, the various ways that lupus can affect brain function were characterized more precisely. Excluded were the separate effects that high blood pressure and drug treatments can have on the brain. In the late 1980s a group of physicians defined criteria for the specific neurological effects of lupus, of which cognitive dysfunction (or lupus fog as it then became known), was one of several. These formal criteria were published in 1999. They allowed for more specific studies of lupus patients to identify how lupus fog affects daily life, and how it can be better managed.
What is “lupus fog?”
Cognitive dysfunction, or what many refer to as "brain fog" or "lupus fog," is often experienced by those who have lupus. The symptoms of lupus fog take many forms, and it affects everyone differently. It can be confusing and frustrating, but you are not alone in the experience. Symptoms range in quantity and severity, and they can include:
- sleeplessness
- rushed speech
- difficulty with word finding
- difficulty navigating
- trouble remembering small details
- impairment of other brain functions that make daily tasks more difficult
Lupus fog is often episodic, meaning that there will be periods of worsening and then a return to normal function. This cognitive dysfunction is usually not severe, and it usually does not progress to the level of severe forms of dementia or Alzheimer’s disease.
Psychosis – a serious mental health disorder – can also occur in lupus patients, but this is different from lupus fog. Psychosis tends to manifest early in the illness, not later on. The good news is that it is fairly rare, short-lived, and unlikely to recur.
Very often corticosteroids, especially in high doses or early after treatment has begun, can cause major mood changes – mostly excitement and sleeplessness – that can be as severe as psychosis. In fact, most of what might be attributed to lupus fog is more likely the effects of medication. Steroid-induced mental changes are different from lupus fog, short-lived (that is, they improve when the dose is reduced), and do not cause permanent damage.
Pictures of the human brain can be created using magnetic resonance imaging (MRI) and a newer type of imaging, called functional MRI (fMRI). While standard MRI can show brain anatomy, fMRI is capable of measuring the working of the brain by determining how much oxygen different parts of the brain are using when a person is engaged in such tasks as planning, speaking or moving. Functional MRI conducted on patients experiencing lupus fog, shows that abnormalities are found in the "efficiency" level of the brain. This means that the person with cognitive dysfunction does not really experience reduced brain power but rather reduced brain processing efficiency. In other words, lupus fog is more like losing speed of thinking rather than losing the ability to think.
How is lupus fog diagnosed?
Several neuropsychological tests are available to assess someone for symptoms of lupus fog. Many use questionnaires that focus on such functions as:
- remembering important experiences in your past
- remembering to take medications
- remembering details at home or work
- concentrating on a task you need to do
A person who is tired or distracted may have trouble scoring well with these assessments. We also have to take into account the education level and skill of the person being tested when interpreting results. The tests usually take a long time to conduct, two days or more. So it is difficult to say which symptoms provide a definite diagnosis because it can vary quite a bit from person to person. Not performing well on these exams should not necessarily be alarming, as scores on these tests are not precise indicators of pathology requiring immediate treatment. With most lupus patients, a key issue is to identify whether their "fog" occurs any more often or more severely than in people who do not have lupus but who do have fatigue.
There are also other kinds of neuropsychological tests. One test lists the names of several colors, but with each word displayed in a color that does not match the color named by the written word (for example, the word "blue" written in red letters, as shown in the graphic below). The goal for the person taking this test is to say out loud the color of the text, rather than the name of the color it spells. This exercise tests the brain’s flexibility in switching tasks.
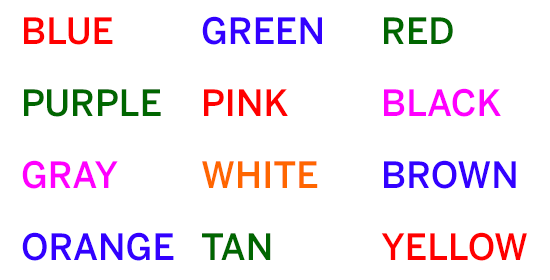
Although certain antibody profiles and other blood tests can identify lupus kidney disease, for example, at this time no single blood test predicts lupus brain disease. With regard to imaging of the brain, standard brain MRI scans commonly show some abnormalities in lupus patients, but these abnormalities do not seem to be associated with brain fog or poor cognition. Functional MRIs, as discussed earlier, may show indications of slower cognitive processing speed.
What are the risks for developing lupus fog?
To date, researchers have not studied the risk of developing lupus fog. However, several studies have looked at the risk for developing dementia in people with lupus. Dementia is a much more serious phenomenon than lupus fog. These studies agree that the risk for dementia in SLE patients is 1.5 to 2 times that of the risk in normal people. However, the absolute risk is only about 3% overall – quite a small risk.1 2
The differences in cognitive dysfunction among those with lupus versus those without it are often due to several factors. The stage of the disease, differences in the diagnoses made by physicians, and the differences among populations in a particular study can all influence the research study results (namely, the recorded changes in learning and memory).
What are current treatments for lupus fog?
Current treatments involve the use of corticosteroids. Another approach is using the medications that largely come from modern psychiatry, such as those used for sleep disorders, and other drugs such as stimulants to improve cognitive processing efficiency.
What research is being conducted for lupus fog?
Research in this area is quite active. Using very advanced technologies, researchers have found some possible mechanisms for lupus fog. Based on these mechanisms, they have proposed using a type of blood pressure medication called an angiotensin converting enzyme inhibitor, or ACE inhibitor, to reduce the symptoms of lupus fog. Clinical trials to test whether this will be effective are underway, including a trial at HSS.
What is the outlook for people with lupus fog?
Cognitive dysfunction occurs in many people with lupus, but it is usually not severe. Likewise, lupus fog usually does not progress to the level of dementia or Alzheimer’s disease. There is more hope than ever before that we will both better understand lupus fog and have more effective, safe treatments to offer patients in the near future.
If you experience episodes of lupus fog, do not panic, and do not think that you are crazy. Do bring this issue to your doctor’s attention. Talk to your doctor to learn about treatments and strategies to manage your life with lupus fog.
References
Footnotes
- Wotton CJ, Goldacre MJ. Associations between specific autoimmune diseases and subsequent dementia: retrospective record-linkage cohort study, UK. J Epidemiol Community Health. 2017 Jun;71(6):576-583. doi: 10.1136/jech-2016-207809. Epub 2017 Mar 1. PMID: 28249989.
- Hanly JG, Kozora E, Beyea SD, Birnbaum J. Review: Nervous System Disease in Systemic Lupus Erythematosus: Current Status and Future Directions. Arthritis Rheumatol. 2019 Jan;71(1):33-42. doi: 10.1002/art.40591. Epub 2018 Nov 24. PMID: 29927108.

