Prevention and strengthening are key components to staying healthy and active. From our athletic trainers and specialists to online education resources, we have what you need to stay in the game.
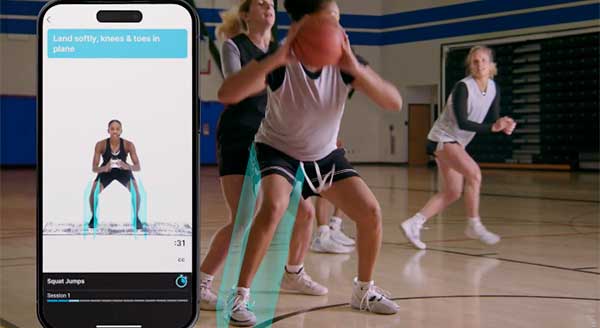
- RIIP (Reduce Injuries Improve Performance) Reps is a free app with neuromuscular training intended to build strength when accelerating, stopping on a dime, cutting, jumping and landing for athletes ages 13 and over. Coaches can easily incorporate this 7-minute program into their regular training regimen.
- Performance and Wellness Services include running assessments, sports-specific movement analysis, metabolic testing, nutrition, one-on-one training and more.
- Athlete Health Program offers training and resources to local groups and schools to improve their fitness and physical education programming.
See all of our Injury Prevention Programs.
Why Choose HSS for Sports Medicine
HSS has been ranked No. 1 in orthopedics for 16 consecutive years according to U.S. News & World Report with one of the top sports medicine programs in the world. Our specialization is second to none - meaning that every step of the process is proven for success.
At HSS, you can expect:
-
- state of the art imaging and radiology from trained musculoskeletal specialists
- a culture that believes in the idea of returning to the game and enhancing quality of life
- a staff that understands an athletes mindset and goals
- surgeons that perform specific sports injury procedures more often than anywhere else