Lupus, Vasculitis and Blocked Blood Vessels
The word “vasculitis” means inflammation of the blood vessels. (“Vasc” refers to blood vessels and “itis” means inflammation.) Vasculitis can be a diagnosis in itself but more often it coexists with lupus or another autoimmune disease and is then considered to be a component of that illness.
Blood vessel inflammation is common to all the rheumatic autoimmune illnesses. When it occurs in a patient who has lupus, vasculitis may simply confirm a diagnosis for lupus but cause no specific additional health problems itself.
Sometimes its occurrence represents a change in the course of the lupus, with vasculitis becoming a serious complication. Thus, the word vasculitis can mean many things. If a doctor says you have vasculitis, ask what that really means in your case – what disease process is going on and what it means for you.
Warning about misuse of the term "vasculitis"
Vasculitis should not be confused with "vasculopathy," which simply means something is wrong with the blood vessels. Although vasculitis is one type of vasculopathy, if there is no inflammation, it is not vasculitis. Some people – even physicians, but especially writers on the internet – incorrectly use these words interchangeably. Unfortunately, even some doctors use the term vasculitis to mean "an autoimmune disease and blood vessel abnormality that I don't completely understand." That is, they use "vasculitis" very loosely as a general term for autoimmune disease.
As a result, you may see statistics about vasculitis that are very frightening. But those statistics, when the word is used loosely, do not provide correct information about your specific situation, and most conclusions that follows those statistics are likely to be wrong.
If your doctor says you have vasculitis, ask specifically what he/she means before you research it on the internet! (Find a doctor at HSS who treats vasculitis.)
What is vasculitis?
Vasculitis is blood vessel inflammation that causes fever, pain, local tenderness and other evidence of blocked blood vessels.
When a blood vessel becomes inflamed and narrowed, blood supply to that area can become partially or completely blocked, cutting off blood supply to the tissues beyond. Inflammation causes the vessel wall to swell. This makes blood stick to the inner wall to form a clot. When vasculitis interferes with circulation in any part of the body it causes local tenderness and pain. If the blood vessels are close to the skin, characteristic rashes occur. Depending on where the blockage occurs, almost any organ in the body can be affected. (Note: Vasculopathy can also block blood vessels but it does not cause the fever, pain and local tenderness associated with vasculitis. It may, however, cause pain if the parts that are no longer receiving a blood supply die – a circumstance called "infarction.")
While vasculitis may involve both the arteries (the thick muscular vessels that carry blood away from the heart) and the veins (the thinner vessels without muscles that carry blood toward the heart), it is rare for both arteries and veins to be involved at the same time.
What vasculitis is not
Many problems that block blood vessels look like vasculitis, leading doctors to sometimes assume they are dealing with vasculitis. However, greater care should be taken to find out what's really going on. Some diseases that are not vasculitis but in which blood vessels become blocked include:
- atherosclerosis (hardening of the arteries)
- growths on the heart valves that break off, especially those due to infection
- excessive blood clotting (antiphospholipid syndrome)
- vessel spasm, especially when caused by drugs (both legal, such as those sometimes used in intensive care units to raise the blood pressure of someone in shock, and illegal, like cocaine)
- abnormal proteins in the blood that form gels in blood vessels in cold weather (cryoglobulins)
When does vasculitis occur in rheumatic disease?
All of the autoimmune rheumatic diseases – lupus, rheumatoid arthritis (RA), scleroderma and dermatomyositis – involve some level of underlying vasculitis. If you biopsy a swollen joint in a person who has RA, you routinely find vasculitis. That finding is consistent with the diagnosis but it doesn’t imply any worse prognosis. It just confirms that an autoimmune disease is present. Vasculitis is a common finding in people with these diseases and important to help make a diagnosis but it doesn't necessarily mean anything more than that.
When is vasculitis an important complication of an autoimmune disease?
There are times in cases of lupus and RA when the disease takes a different course because a different type of vasculitis has developed or because the blood vessel inflammation increases to become a larger part of the problem. If that happens, you start getting sicker and develop a fever. These are clues to the physician that there has been a change in the course of illness. In those cases, we say "This is lupus complicated by vasculitis" or "this is rheumatoid arthritis complicated by vasculitis." The disease has changed its character and usually needs more vigorous treatment.
Diseases in which vasculitis is the specific illness, rather than a complication of another disease
- polyarteritis nodosa, which mostly affects middle-aged people
- temporal arteritis or giant cell arteritis, which affects arteries, usually in the head, of older people
- allergic vasculitis, which is an abrupt reaction that sometimes follows infection or drug allergy
- Takayasu's arteritis, which is a relatively rare disease of young women, largely in Asia, involving large blood vessels
- granulomatosis with polyangiitis (formerly known as Wegener's granulomatosis), which affects the kidneys, lungs and blood vessels
- some of the new cancer drugs, called checkpoint inhibitors, sometimes cause vasculitis
These specific kinds of vasculitis are treated differently, depending on the underlying problem.
Vasculitis by the size of the blood vessel
It is often easier to discuss vasculitis in terms of which type blood vessels are involved (the small, medium or large vessels), rather than by the disease it is associated with.
Small-vessel vasculitis
This is the most common form of vasculitis seen in lupus and it is fairly common in dermatomyositis and scleroderma, but less common in rheumatoid arthritis. The small vessels are at your fingertips and inside your organs, such as the kidneys.
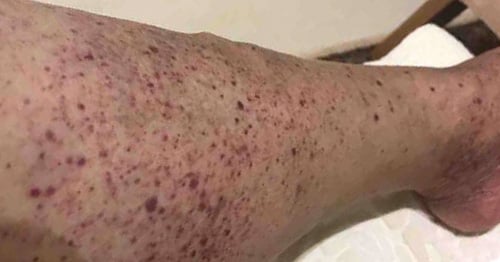
Some signs of it can be seen externally with a small magnifying glass. It shows tiny broken vessels in the cuticle and hemorrhages along the edge or under the nail. Or on other parts of the skin, especially the legs, you see little red dots with black centers that occasionally cause a burning sensation (Figure 1). This small-vessel vasculitis is not particularly threatening.
Sometimes the pattern of blood vessels on the skin is very prominent (Figure 2). (The prominent blood vessel pattern may be normal in cold weather, when it shows how blood vessels constrict to preserve body heat; in vasculitis it is present in both cold and warm.) It is a manageable but annoying category of the disease, with fairly mild symptoms that may not need treatment.
Some people don't even know that they have it. However, when the blood supply to the nerves in the feet is cut off by vasculitis, a patient may develop numbness or weakness in the affected areas.
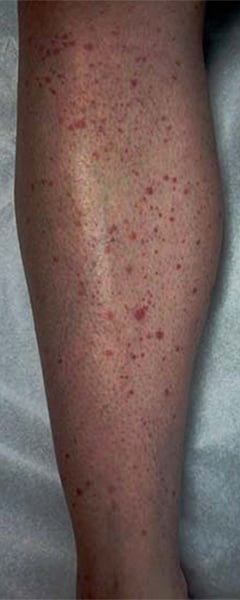
Figure 1. A rash type, often called “palpable purpura,” associated with small-vessel vasculitis.
Another type of small-vessel vasculitis in people with lupus and RA is associated with kidney inflammation called glomerulonephritis, which, if untreated, can cause kidney failure. Small-vessel vasculitis can also be seen, especially in children, as palpable purpura (red dots that feel like tiny bumps), which causes a rash, but also causes abdominal pain and kidney inflammation (called Henoch-Schoenlein purpura, or IgA nephritis). It may come and go and be treated only when it's causing problems, or it may require longer-term treatment.
In addition, small-vessel vasculitis can be seen in severe allergies and in several types of infections. When you treat the underlying cause, such as the infection, the vasculitis goes away.
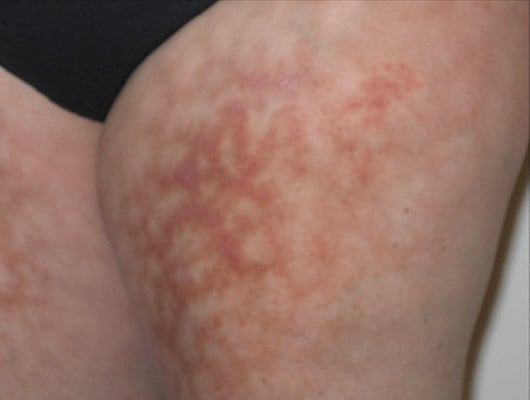
Figure 2. A rash type, often called “livedo,” associated with small-vessel vasculitis.
Diagnosis of small-vessel vasculitis can be made by an experienced clinician simply by observation. Here, the question is not "Is it vasculitis?" but "What's causing this vasculitis?" Less experienced physicians want to do blood tests or skin biopsy. Angiography and other X-rays of blood vessels are not useful for small-vessel vasculitis. A kidney biopsy may be needed in some circumstances.
What does it mean when small-vessel vasculitis occurs in someone with long-term lupus or RA? You may not need to treat the vasculitis itself; you have to look at the whole patient and ask “Why has this complication occurred?” It could be an allergy or an infection, which should be found and treated. Small-vessel vasculitis should not be ignored because it is important, but it is usually not life-threatening. If allergy or infection has been ruled out, treatment with corticosteroids (prednisone) or other immunosuppressants may be negotiable, depending on what the patient wants to tolerate in terms of side effects.
Medium-vessel vasculitis
These vessels include those that lead down your arms and legs, and also to your heart and brain, and even those supplying blood to your intestines or kidneys. Medium-vessel vasculitis is usually what physicians are referring to when they call vasculitis a serious disease. (For example, polyarteritis nodosa, a type of vasculitis that has its own name, tends to be very dramatic. People who have it say they have never felt worse in their lives.) Medium-vessel disease can occur in lupus and RA, but it is rare.
The symptoms of medium-vessel vasculitis include:
- fever
- severe muscle aches
- sudden loss of power in specific muscles (perhaps a foot starts dragging)
- severe abdominal pain
- sudden loss of circulation in a finger or toe that turns totally black (gangrene)
- stroke or heart attack
Again, an experienced physician can make the diagnosis at the bedside based on symptoms alone. Blood tests are useful to confirm the diagnosis. Sometimes a muscle biopsy, nerve conduction study, or angiography is necessary to be sure. The reason for the vasculitis also must be identified: It may be caused by infection, such as hepatitis B or hepatitis C; it may be polyarteritis nodosa alone; or it may be a complication of an autoimmune disease.
Medium-vessel vasculitis can be life-threatening because the blocked vessels going to the heart can cause a heart attack, or those going to the brain may cause a stroke. Survival depends on immediate recognition of the disease and immediate and vigorous treatment. When medium-vessel vasculitis occurs, treatment is not negotiable. High-dose steroids and cyclophosphamide, and some newer drugs like rituximab, are needed to reverse it as soon as possible. A number of even newer drugs are also being considered and/or used in patients with this type of vasculitis.
Large-vessel vasculitis
The large vessels are those that lead from your heart (namely, the aorta and the arteries that go across the shoulders and down to the hips). Large-vessel vasculitis is not part of lupus or rheumatoid arthritis. When the large blood vessels develop vasculitis, it is an independent disease, such as Takayasu's or giant cell (also called cranial or temporal) arteritis. This type of vasculitis has completely different symptoms, usually involving fever and pain in the part of the body affected. Many times it requires a bit of cleverness to figure out what's going on. Large-vessel vasculitis is not immediately threatening, but it can do a lot of damage if not treated for long periods.
Treatment is aimed at preventing disability, such as the blindness that may be caused by giant cell arteritis, usually prednisone, but now including other drug options like conventional immunosuppressive agents (methotrexate and mycophenolate), TNF Alpha inhibitors, anti-B-cell therapies (rituximab and belimumab) and the newly available JAK inhibitors that combat the inflammatory response that occurs with autoimmune disorders.
Summary
Vasculitis is inflammation of the blood vessels; vasculopathy is anything that may go wrong with blood vessels. Vasculitis occurs as a regular part of rheumatic disease, or vasculitis may occur as its own illness. Many other problems may mimic vasculitis.
Vasculitis may be serious, but it is not serious in most cases in people with lupus and other rheumatic diseases. It may not even require any change in treatment. However, when serious vasculitis occurs, very aggressive therapy is necessary, depending on the cause. In serious vasculitis related to autoimmune diseases such as lupus, aggressive therapy with prednisone and other immunosuppressants is essential.
