Compound Fracture
Medically reviewed by William M. Ricci, MD
On this page
What is a compound fracture?
An open fracture, also called a compound fracture, is a bone fracture that is accompanied by breaks in the skin, causing the broken ends of bone to come into contact with the outside environment. The more common, less severe fracture without bone sticking out and breaking the skin is known as a closed fracture.
Why is an open fracture also called a compound fracture?
Open fracture is the term most physicians use today. The older naming convention of “compound fracture” was so named because the protrusion of broken bone through the skin in an open bone fracture complicated or “compounded” the simple fracture injury with a secondary injury that made the patient vulnerable to infection and sepsis. “Compound fracture” is still the popular term most people recognize. Other terms sometimes used for this injury include “open wound fracture,” “exposed fracture,” or “bleeding fracture.”
What causes a compound fracture?
This is usually caused by a broken bone piercing the skin during a high-impact trauma, and it most commonly affects the lower leg, but it can occur in any part of the extremities.
The severity of a compound fracture depends on multiple factors, such as the degree of damage to the bone and the surrounding soft tissues (muscle, tendon, ligament, etc.), the degree of wound contamination with soil, grease, sand, etc., and whether there or not there is any disruption of the major blood vessels to that part of the body.
Which bones most frequently experience an open fracture?
Although any bone can experience an open fracture, the tibia, or shin bone, is the most susceptible. This is because a substantial portion of the tibia is immediately beneath the skin rather than having surrounding muscles like the femur (thighbone). When the tibia breaks, it can easily protrude through the thin layer of skin. When other bones that are better surrounded by soft tissues experience open fractures, it is usually because of a high energy injury mechanism such as a high-speed car crash or a fall from a substantial height.
Why is a compound fracture dangerous?
Compound fractures are urgent situations because they are at a high risk of infection, tissue damage, and healing complications. The exposure of the bone to the outside elements where bacteria exist is one reason for the elevated risk of infection. Another factor is the soft tissue damage associated with all high-energy fractures. Injured tissues are more susceptible to infection than healthy tissues. All high-energy fractures, including compound fractures, are at risk for another serious associated condition called compartment syndrome and are at risk for healing complications, such as nonunion.
Infection
High-energy open fractures become infected much more commonly than similar fractures that are not open. Infection, when it occurs, most commonly becomes evident weeks or even months after injury. In addition to concerns about infection, compound fractures are at high risk for nonunion – not healing in a timely fashion or requiring additional surgery to promote healing.
Compartment syndrome
Compartment syndrome is a medical emergency where injured muscle tissue swells to such a degree that the swelling damages the muscle itself as well as other adjacent tissues − most often nerves. The swollen muscle is constrained inside a compartment by tissue called fascia, which cannot stretch to alleviate the pressure. As the pressure rises, all tissues within the compartment are damaged. When compartment syndrome is not treated, the tissues can undergo necrosis (death) and cause permanent loss of function of the involved muscles and nerves. The treatment for compartment syndrome is an urgent surgery called a fasciotomy, which relieves the built-up pressure in the involved muscle compartment.
Nonunion
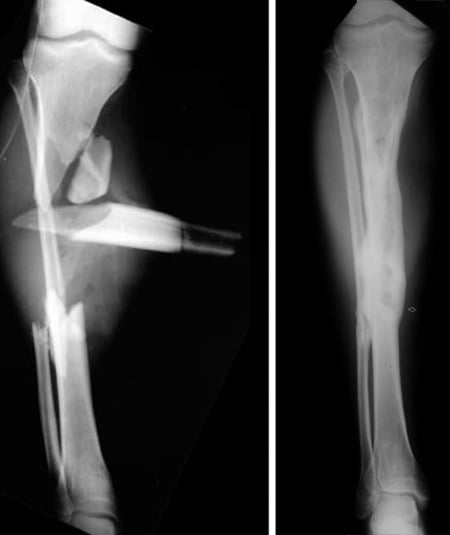
Nonunion occurs when a fractured bone fails to heal or fails to “unite.” Most often, fractured bones heal within 6 to 12 weeks after injury. Sometimes the healing process takes longer, and this is called a “delayed union.” If a bone does not fully heal after several months and it appears on X-rays that the healing process is no longer progressing, then a nonunion has likely occurred. This means that without further intervention such as nonunion surgery, the fractured bones are unlikely to heal. HSS surgeons have extensive experience treating nonunions.
Can a compound fracture be life-threatening?
An open fracture, in isolation, can be life-threatening only in extremely rare circumstances. For example, when a broken bone injures a major blood vessel and timely medical treatment is not available. Mortality associated with fractures is usually related to associated injuries to other critical organs, such as the brain, lung, and liver. If not properly treated, open fractures can lead to non-lethal, long-term complications such as bone infection and problems with proper bone healing.
Emergency care
Patients with open fractures should be transported by ambulance, if possible, to the nearest trauma center emergency room to initiate appropriate treatments. The wound should be evaluated and bandaged, and the patient should receive antibiotic medication as soon as possible to minimize risk of infection. The fracture should similarly be evaluated with X-rays and immobilized.
The Orthopedic Trauma Service at HSS treats patients with open fractures regularly. Our patients are evaluated head-to-toe, as there are often associated injuries in other body parts. Orthopedic trauma surgeons work closely alongside general trauma surgeons, neurosurgeons, plastic surgeons, and anesthesiologists as appropriate to provide injured patients with the best care possible to decrease their risks of complications.
How are compound fractures treated?
Treatment for open fractures begins after all emergency care described above is performed. Patients with compound fractures are brought to the operating room for more thorough wound cleaning and irrigation, and for the removal of damaged tissue that can contaminate the wound.
Unless there are other emergency procedures that must be performed, such as fasciotomy for compartment syndrome, this acute wound care will be followed by surgical realignment of bones. The fracture is either temporarily or definitively stabilized at this initial operating room setting. This typically involves open reduction (making an incision to access and realign the bone or bones manually), followed by internal or external fixation.
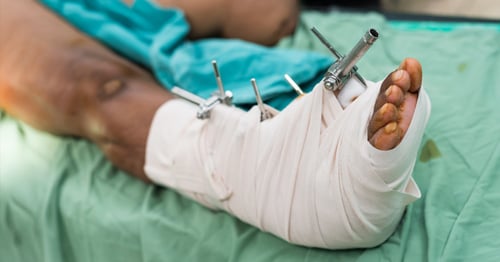
Fixation refers to the use of rods, wires, pins, screws and/or plates placed to hold the bone in proper position during healing. Depending on the severity of the wound, additional procedures for wound management (additional cleaning and/or skin or muscle grafts to cover the wound) may be required.
What should you do when a person has a compound fracture?
First, call an ambulance to transport the patient safely to the nearest hospital. Keep the patient as immobilized as possible while waiting for care to arrive. Unnecessary movement increases pain and damage to the tissues.
Do not try to realign the affected extremity (arm, leg, finger, etc.) where the bone is broken without the presence of trained medical personnel who have the proper splinting supplies. Improper handling can contaminate the wound and cause further damage.
Try to keep the affected extremity as clean as possible. If available, place moist sterile gauze over the wound. At the very least, the wound should be protected from contact with the ground or unclean surfaces.
How do you prevent a compound fracture?
Although not every accident or sports injury can be avoided, it is always important to take precautions and wear safety equipment during high-energy sports activity (such biking, skateboarding, skiing or snowboarding). In addition to the quintessential helmet to avoid head injuries, skaters and skateboarders should wear protection like elbow, knee and wrist pads and motor sport (motorcycle, snowmobile) participants should wear leather or other appropriate protective padding.
Key takeaways
- A compound fracture, also called an open fracture, occurs when a broken bone pierces the skin, exposing bone at the fracture site to the outside environment.
- An open fracture is more serious than a closed fracture because it carries a high risk of infection, tissue damage, and healing complications such as nonunion.
- These injuries usually result from high-impact trauma, such as a fall from a height, vehicle accident, or sports injury, and most often affect the lower leg.
- While open fractures are rarely life-threatening on their own, they can become serious if a major blood vessel is injured or if infection develops.
- Emergency care includes stabilizing the patient, covering and cleaning the wound, administering antibiotics, and immobilizing the fracture before surgery.
- Definitive treatment involves surgical cleaning of the wound and realignment of the bone, followed by internal or external fixation with rods, screws, plates, or pins.
- Patients are often treated in a multidisciplinary trauma setting where orthopedic surgeons collaborate with other specialists to manage associated injuries.
- To help prevent compound fractures, wear appropriate protective gear during high-risk sports or activities such as cycling, skateboarding, skiing, or motorsports.