Ankylosing Spondylitis
Medically reviewed by Theodore R. Fields, MD, FACP
Ankylosing spondylitis is a form of spondyloarthritis that causes inflammation primarily in the spine, sternum, and large joints in the body.
What is ankylosing spondylitis?
Ankylosing spondylitis (AS) is a chronic, inflammatory disorder that particularly affects the spine. But it can also affect several other joints, such as the hips, knees and chest wall. It can also cause inflammation at the entheses – areas where tendons attach to bone, such as where the Achilles’ tendon attaches to the heel or where the tendons at the elbow. The severity and pattern of joint involvement varies from person to person.
"Ankylosing" refers to the tendency of the spine to fuse (or “ankylose”). One component of this fusion process is that ligaments that connect one vertebra to another become injured by the inflammatory process. This causes them to form scar tissue, and then new bone tissue can form within the ligaments. In addition, inflammatory injury to bone tissue itself also causes scarring followed by bony overgrowth. This leads to the fusion of one spinal vertebra to the one above or below it.
"Spondylitis" refers specifically to the inflammatory process ("itis") of the spine. As a result of this inflammation, a person feels stiffness and pain in the back, a gradual loss of mobility, and in the most severe cases, a complete loss of motion of the lower back. The neck (cervical spine) often has a similar inflammatory process and can likewise progressively lose motion.
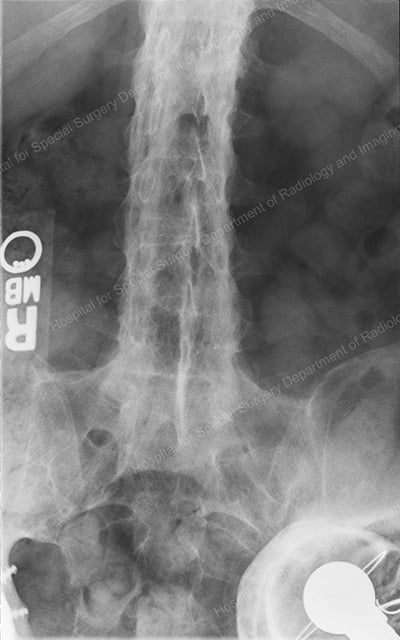
Frontal-view X-ray of an ankylosed spine
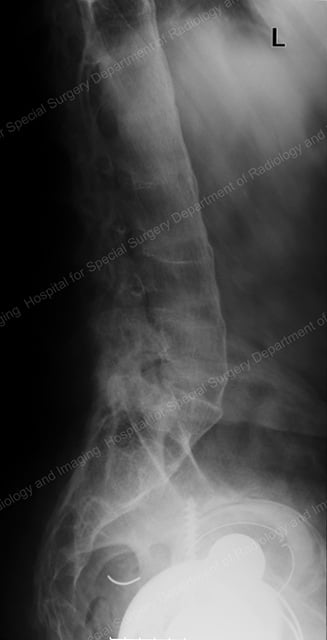
Side-view X-ray of an ankylosed spine
Who gets ankylosing spondylitis?
Ankylosing spondylitis often begins at a young age (from the teens to the third decade of life) and is more common in men – about two to three times more common than in women. AS can also affect children, called juvenile ankylosing spondylitis, and more commonly so in boys than girls.
What causes ankylosing spondylitis?
Genetics play a large role in this condition. More than 90% of people with ankylosing spondylitis have a particular genetic marker called HLA-B27, which can be found on their white blood cells. This marker does not appear to be the only cause, however, as 80% of people with this genetic marker never develop an inflammatory disease. It is clear that some unidentified environmental trigger (and likely there is more than one type) plays a role in determining which people with this genetic marker end up developing ankylosing spondylitis.
A number of people with AS will have a family history of the condition, although it may be much more painful and involve more areas of the body in one family member than another. Many people with AS will not be able to identify anyone else in their family with the condition, however, since only about 20% of those with the HLA-B27 genetic marker will get an inflammatory condition such as AS.
People with the HLA-B27 genetic marker can develop other types of inflammatory conditions without developing AS, such as having eye inflammation with no accompanying arthritis. As noted above, having this genetic marker does not by itself mean a person has ankylosing spondylitis or any other inflammatory condition.
What are the symptoms of ankylosing spondylitis?
The most common symptom of ankylosing spondylitis is low back pain and/or neck pain, morning stiffness and limited motion that is improved by exercise and unrelieved by periods of rest. The second most common symptom is joint pain in the hips, shoulders, knees, chest wall, or other areas.
Uveitis (eye inflammation) can occur in this condition, and regular ophthalmology checkups are important, since eye damage can occur even before a person notices any symptoms. Heart and lung problems can also be associated with ankylosing spondylitis but are fortunately less common.
Symptoms of ankylosing spondylitis vary from patient to patient, but they most commonly begin with the onset of low back pain and stiffness that is especially noticeable in the morning hours and after long periods of rest. This pain is usually relieved by physical activity and improves by the end of the day. Some patients experience similar pain in the buttocks, hips, chest wall, upper back, and neck. If left untreated, the ankylosing process can result in a "hunchback" appearance.
Patients are also prone to an onset of arthritis in the large joints and elsewhere, and can – in some cases – experience heel pain related to Achilles tendonitis, lung problems (as a result of lung scarring and spinal inflammation, limiting chest expansion), aortitis (inflammation of the aortic valve and the aorta – the large artery exiting from the left side of the heart), and uveitis, which can lead to visual loss.
How is ankylosing spondylitis diagnosed?
Early diagnosis is very important with ankylosing spondylitis. Unfortunately, it can be difficult to diagnose since its symptoms (especially its most common one, low back pain) are also caused by many other conditions. In order to make this distinction, a combination of diagnostic measures is required, including a physical exam, imaging studies, and laboratory tests. Diagnosing AS is really a matter of medical history, physical exam, and X-ray or other imaging studies, more than any specific blood test. Many people experience symptoms for years before getting a correct diagnosis.
Imaging studies include X-rays and, if necessary for more detailed evaluation, CT scans or MRIs.
There is no single definitive laboratory test to confirm an ankylosing spondylitis diagnosis, but various lab tests are employed to detect signs of an inflammatory process (for example, the sedimentation rate may be elevated as a sign of inflammation in AS). A blood test for the presence of an HLA-B27 gene marker can be helpful, but the diagnosis is made by a combination of history, exam, lab and imaging studies.
How is ankylosing spondylitis treated?
It is very important to get an early diagnosis for ankylosing spondylitis, since treatment is needed even for mild and early cases. All patients with AS need to begin a physical therapy regimen as soon as possible, and a significant number need strong medications to quiet the inflammation and keep them functional. (Find a doctor at HSS who treats ankylosing spondylitis.)
Physical therapy and exercise
It’s essential for all ankylosing spondylitis patients to engage in physical therapy and home exercise programs, and to strive for proper maintenance of posture and to help maintain maximum possible flexibility. AS stiffens the spine and tends to position the head to be held forward and the lower back to remain in a flexed position. Stretching and exercise regimens aim to reduce all of these tendencies and increase flexibility.
Since the lungs can be affected by anylosing spondylitis (both by scarring that results from inflammation and by a decrease in chest expansion while breathing as a result of chest wall inflammation), breathing exercises are important. This can help patients with ankylosing spondylitis maintain their exercise tolerance. It is also important for this reason that people with ankylosing spondylitis not smoke or vape.
Medications
Medications can be tremendously helpful in relieving pain, restoring mobility, and stopping or slowing disease progression.
While nonsteroidal anti-inflammatory drugs (NSAIDs) such as indomethacin, naproxen, and celecoxib (Celebrex, a COX-2 inhibitor) haven’t consistently demontrated an ability to mitigate the spinal fusion process, they do work to reduce inflammation, stiffness, and the resulting pain for many ankylosing spondylitis patients. For some people with milder spondylitis, NSAIDs, along with physical therapy, may be all the treatment they need.
There has been excellent evidence that anti-TNF agents (a group of medications within the category of biologic medications) can provide significant functional improvement, and these are used in many patients with more serious cases of AS. These anti-TNF agents – including infliximab, etanercept, adalimumab, golimumab and certolizumab – improve mobility while alleviating pain. The anti-TNF medications are given either by self-injection or intravenously in a medical office.
Another group of biologic medications, which block a chemical called IL-17, have been approved by the FDA for ankylosing spondylitis. The two approved medications in this group are secukinumab and ixekizumab, and are both self-injected medications.
Other medications that have been FDA-approved for ankylosing spondylitis include the group of oral medications called JAK inhibitors: specifically tofacitinib and upadicitinib. For patients with AS and arthritis of the hip or knee, for example, local steroid injections can help with pain and stiffness.
Patients with ankylosing spondylitis, due to decreased mobility and inflammation, are at increased risk of osteoporosis. They should have their bone density evaluated and treated if it is low.
Is there surgery for ankylosing spondylitis?
The great majority of people with ankylosing spondylitis never need surgery for this condition. Surgery is usually considered only when a person’s AS has progressed to a point to where a patient’s mobility is severely impaired due to chronic, debilitating pain or a painful deformity. For those who do, several procedures are available.
The nature of the surgery will depend on the degree of deformity, whether or not the bony changes are causing any pressure on nerves, and the stability of the spine. The procedures will generally involve an osteotomy, which refers to the removal of some of the bone and realignment of the spine. Instrumentation and spinal fusion are generally used to allow the bone to heal in a stable position. Also, some people with ankylosing spondylitis will have severe enough hip arthritis that they need a hip replacement, but this is uncommon.
The type of surgery will depend upon the specific case and the judgment of the surgeon – and again, surgery is rarely needed for ankylosing spondylitis.
What is the prognosis for someone with ankylosing spondylitis?
As is true for all types of inflammatory arthritis, ankylosing spondylitis progresses differently on a patient-by-patient basis, and symptoms will vary. In some people, the hardening of the spine occurs at a faster rate, while others will experience only slight inflammation and pain, and little loss of function.
Again, in common with many other types of inflammatory arthritis, ankylosing spondylitis is not presently curable, but very effective treatments exist. NSAIDs such as indomethacin or naproxen can be extremely helpful, and pain killers without anti-inflammatory properties (such as acetaminophen) can also help. The anti-TNF medications clearly often provide dramatic improvements in function and may prove effective in halting the disease in the long term. Anti-IL-17 medications are also frequently effective. Surgery is an occasional option for those with advanced, debilitating forms of the disease.
Regardless of the medications used in the individual case, the importance of exercise and physical therapy cannot be overstated.
The outlook for patients with ankylosing spondylitis is much better today than it was even as recently as the first decade of the 21st century. It is very important for ankylosing spondylitis to be diagnosed as early as possible, before the spine has a chance to fuse. If a person with AS is faithful to their exercise and physical therapy program, and works with their rheumatologist to develop a medication regimen that is right for them, their chances of a highly functional, long-term outcome are excellent.
In the news
- What’s the 12-3-30 Workout All About?
- Ways to Sit, Stand, and Sleep Easier With AS
- Finding Relief for AS Pain
- Exercise for Ankylosing Spondylitis: What You Need to Know
- Get Ready to Reach Your Flexibility Goals
- Boost Your Balance and Flexibility by the End of This Month
- Exercise Your Way to Better Mobility with This #ASWarrior
- How Ankylosing Spondylitis Is Different for African Americans
- Dream Big: Namaste Your Way to Better Mobility With Our #ChronicYogi
- HSS Rheumatologists, Social Worker Honored by American College of Rheumatology
- 5 Ways to Practice Good Posture
- Frailty Affects Nearly Half of Older Patients With Ankylosing Spondylitis or Psoriatic Arthritis
- Ankylosing Spondylitis and Vertigo: What Are the Connections?
- 3 Stubborn Myths About Ankylosing Spondylitis
- 12 Myths About Axial Spondyloarthritis That Are Dangerous to Believe
- 7 Surprising Symptoms of Ankylosing Spondylitis
- What to Eat — and Avoid — for Strong Bones if You Have Ankylosing Spondylitis
- 8 Things All Women Who Have Ankylosing Spondylitis Need to Know
- Treatment approaches for improving QOL in ankylosing spondylitis
- Best Yoga Moves for Ankylosing Spondylitis
- 6 Diseases That Could Mimic Ankylosing Spondylitis — and Delay Your Diagnosis