Microdiscectomy: Minimally Invasive Surgery for a Herniated Disc
Microdiscectomy is a type of minimally invasive discectomy commonly used to treat a herniated disc.
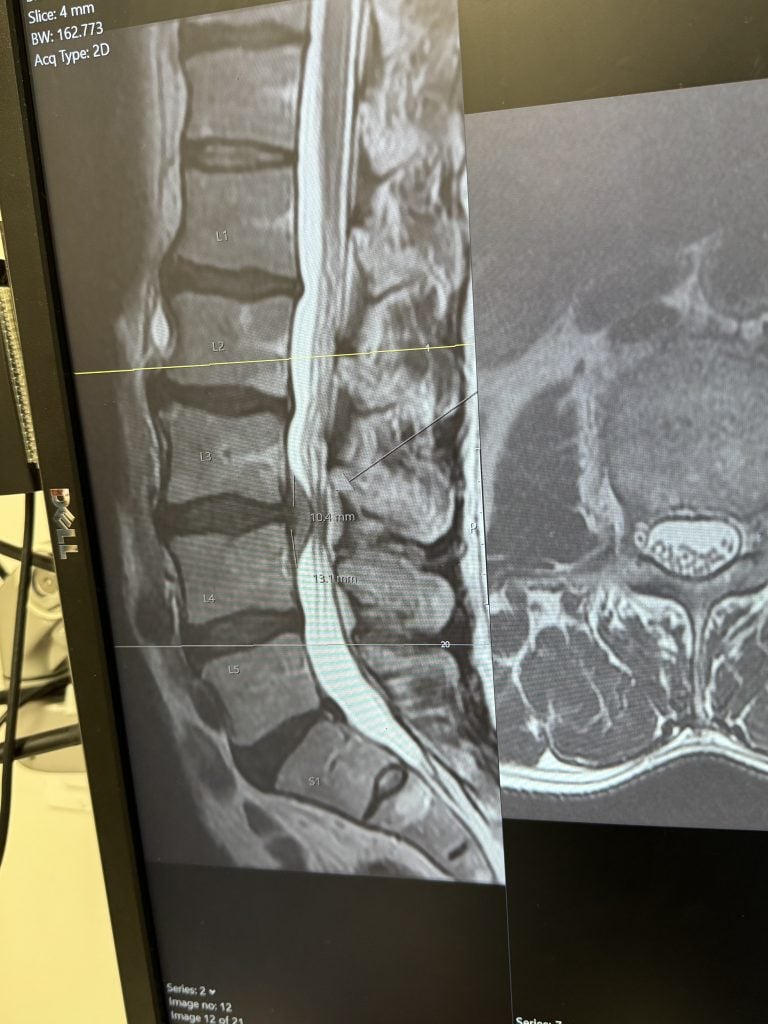
When a herniated disc compresses a spinal nerve, symptoms can include pain (which may extend down one or both arms and legs, as is the case in sciatica), muscle weakness and difficulty with repetitive motions.
Summary: This article explains microdiscectomy surgery, including who may benefit from it, how it is performed using modern surgical techniques, and possible complications. Readers will learn what to expect after surgery, including expected recovery timelines, and long-term outcomes regarding pain relief.
What is microdiscectomy?
Microdiscectomy is a surgical procedure for the relief of pain and other symptoms that occur when a herniated disc in the spine presses on an adjacent nerve root. During the operation, the surgeon frees the nerve by removing small fragments of disc, bone and ligament.
Microdiscectomy is sometimes described as a minimally invasive spine surgery, because it requires only a small incision and the use of a microscope or surgical glasses, called loupes, to magnify the site where the injury has occurred. The surgeon also uses smaller tools and instruments to work in the restricted space of the spine. Microdiscectomy is a type of spinal decompression surgery, and the term microdecompression – which describes the surgical removal of any bone or ligament that is compressing a nerve – may also be used to describe the procedure. However, the term "microdiscectomy" is more specific to the removal of the fragment of herniated disc tissue that is causing the patient’s symptoms.
Because most patients will recover from a herniated disc without surgery, microdiscectomy is recommended only after conservative treatment, including physical therapy, cortisone shots, and other medication have been tried for a period of at least 6 to 12 weeks, without bringing relief. In some cases, motor weakness may be a reason to have this surgery sooner. Patients with cauda equina syndrome require immediate surgical intervention. This is a condition in which pressure on the nerves in the lower portion of the spine affects bladder and bowel function, but it affects less than 1% of people.
How does a surgeon perform a microdiscectomy?
Microdiscectomy surgery may be approached using one of three minimally invasive techniques to gain access to the herniated disc and nerve: a midline, tubular or endoscopic microdiscectomy.
Historically, a traditional discectomy required a large incision and involved removal of the entire disc. Today, with the availability of advanced techniques and equipment, almost all spine surgeons perform microdiscectomies. The procedure usually results in rapid, and sometimes immediate, pain relief.
Microdiscectomy techniques
- A midline microdiscectomy, in which the surgeon makes a one to two-inch vertical incision in the back, lifts the surrounding muscles off the vertebrae, and uses instruments to hold apart the layers of tissue during the procedure.
- A tubular microdiscectomy, in which the surgeon inserts a series of small tubes or dilators through a small incision to create a corridor through the muscle in which to operate, thereby causing less disruption to this tissue.
- Endoscopic microdiscectomy (sometimes also known as microendoscopic discectomy), in which an even smaller incision is made and the surgeon employs a miniaturized camera and instruments; this approach also involves less disruption to surrounding tissues.
Video: Animation of a lumbar microdiscectomy spine surgery
This animation illustrates a minimally invasive lumbar microdiscectomy, which may may involve either a lumbar laminectomy or laminotomy procedure in order to access the portion of spinal disc to be removed. A laminectomy removes one or both both lamina (a bony protective covering on the rear of each spinal vertebra), while a laminotomy makes only a small opening in a lamina.
What are the benefits of a microdiscectomy?
Regardless of which particular microdiscectomy technique selected, the surgical goal is the same: to remove the disc fragment and any bone or ligament that may be compressing the nerve root. To do so, the surgeon creates a small window in the vertebra (a procedure also called a laminotomy) and pulls away the ligamentum flavum, the underlying tissue, to reveal the dura (the covering of the spine) and the nerve root. The herniated part of the disc is then removed to complete the nerve decompression.
Imaging techniques, including X-rays, are used before, and sometimes during, the surgery to ensure localization of the correct operative site.
While herniated discs may occur in almost any level of the spine, lumbar microdiscectomy – surgery in the lower portion of the back – is the most common site for this procedure.
What complications can occur with microdiscectomy?
During surgery, multiple safety measures are followed to control bleeding, prevent infection and avoid injury to any surrounding tissues. Rarely, a tear in the dura (the tissue surrounding the spinal nerves) may occur. The surgeon repairs this with a suture or a patch made of collagen.
How long does a microdiscectomy take?
On average, microdiscectomy surgery takes between 30 to 60 minutes to complete. However, because patients are given general anesthesia and must spend time afterward in the recovery room for a period of monitoring, the total time usually extends to about two hours.
In almost all cases, people undergoing microdiscectomy may return home the same day. Upon discharge from the hospital, patients are typically given a small amount of pain medication – including acetaminophen or small dose of opioid medication – and a muscle relaxant with instructions regarding postsurgical care and how to taper these medications appropriately. Special emphasis is given to symptoms that signal the need for immediate medical attention, including muscle weakness, change in bladder or bowel function, and extreme and unexpected back or leg pain.
What is the expected microdiscectomy recovery time?
Following a two-week period of rest to allow the soft tissues to heal, many patients feel well enough to return to work. However, microdiscectomy recovery typically requires a six-week period of modified activity and includes a course of physical therapy starting between four and six weeks after surgery.
Physical therapists focus on helping patients strengthen core muscles and loosen stiff joints, as well as creating a home exercise program to help protect the spine. All patients are cautioned to ease back into their previous routines gradually, especially those whose work requires physical labor. Because sitting in a chair and leaning forward places pressure on the spine, people with more sedentary jobs also need to be attentive to their posture and take a short walk or do some gentle exercise every hour or so.
Patients who plan to resume driving after surgery must wait until they are pain-free, finished with any medication that causes drowsiness, and able to both shift their foot between pedals and turn in their seats easily and without pain. To test individual comfort, a practice drive in a parking lot or other safe space, in the company of another driver is recommended before returning to regular roadways.
Is a microdiscectomy painful?
Following surgery, most patients do well with a small amount of non-opioid pain medication and a drug that relaxes the muscles. While there is some discomfort associated with the surgical incision, many patients experience rapid relief of the pain caused by the herniated disc.
In patients who have experienced nerve compression and associated symptoms over an extended period, pain relief may take longer. When leg pain has been the primary symptom, the pain typically retreats up the leg over time. In addition, patients may experience muscle cramping or mild numbness or tingling after surgery which typically resolves with time.
Who is eligible for microdiscectomy?
Most patients with herniated discs that do not respond to a trial of medication and physical therapy over time, are eligible for a microdiscectomy. While the condition is usually seen in individuals aged 30 to 50, it does occur outside this age range.
Herniated discs are rare in children and young adults, who are more frequently able to recover without surgical intervention. Microdiscectomy may be appropriate for adults in their 80s or 90s, though they should be cautioned that there is an increased chance of medical or surgical complications in this population.
How successful is microdiscectomy?
Overall, microdiscectomy success rates are excellent, with many patients expressing a high degree of satisfaction with the outcome. Careful presurgical screening and evaluation, as well as patient commitment to maintaining good spine health following microdiscectomy, contribute to the success of the surgery.
An HSS study found that even people who feel extreme pain or disability before surgery typically experience meaningful pain relief and functional improvement afterward. However, there’s a lot of inconsistency in how doctors and researchers determine whether a lumbar microdiscectomy has been “successful.” Patients need to interpret success rates carefully based on their own, meaningful symptom relief.1,2
Finally, it should be noted that some people with herniated discs are also found to have other issues in the spine that are causing nerve-related pain and disability. In such cases, additional procedures such as a laminectomy – removal of the lamina (bony roof over the spinal canal) in one or more vertebrae, may be required if it is felt that these issues are contributing to their disability.
Can microdiscectomy be used on a disc that herniates a second time?
In cases of disc reherniation, microdiscectomy can be performed for a second time on the same disc, often with good results. However, if herniation occurs in the same disc a third time, a different type of treatment will be recommended.
Key takeaways
- Microdiscectomy is a minimally invasive procedure that relieves nerve pain by removing the portion of a disc compressing a spinal nerve, rather than the entire disc.
- Unless urgent neurologic symptoms are present, it is typically recommended only after nonsurgical treatment fails, usually including physical therapy, medication, and/or injections.
- Surgery often takes less than an hour, with many patients experiencing rapid or immediate symptom relief.
- Most procedures are performed on an outpatient basis, with recovery time generally measured in weeks, not months.
Explore Related Patient Stories
View All Patient StoriesReferences
- Koehne NH, Song J, Locke AR, Tiao J, Maayan O, Mai E, Issa T, Corvi JJ, Namiri NK, Hecht AC, Iyer S, Qureshi SA. Variability of minimum clinically important difference threshold values in lumbar microdiscectomy literature: a systematic review. Spine J. 2025 Oct 10:S1529-9430(25)00813-7. doi: 10.1016/j.spinee.2025.10.010. Epub ahead of print. PMID: 41075990. https://pubmed.ncbi.nlm.nih.gov/41075990/
- Virk S, Vaishnav AS, Mok JK, McAnany S, Iyer S, Albert TJ, Gang CH, Qureshi SA. How do high preoperative pain scores impact the clinical course and outcomes for patients undergoing lumbar microdiscectomy? J Neurosurg Spine. 2020 Aug 7;33(6):772-778. doi: 10.3171/2020.5.SPINE20373. PMID: 32764173; PMCID: PMC11620279. https://pubmed.ncbi.nlm.nih.gov/32764173/