Meniscus Surgery: Meniscectomy, Transplant, and Repair
Surgery is not necessary for all meniscus injuries, but it may be considered when conservative measures have failed. Arthroscopic procedures make meniscus surgery less intrusive than in the past, with shorter recovery times. The decision to have surgery depends on many factors, including the type and severity of the injury, and it should be made in close consultation with an orthopedic specialist who can evaluate the risks and benefits.

How do you know if you need meniscus tear surgery?
Meniscus injuries occur on a broad spectrum, and not all meniscus tears require surgery. The need for meniscus surgery depends on a lot of factors, including the location, size, and mechanism of injury (for example, traumatic versus degenerative) for each tear. Certain patient factors may also influence the need for surgery, including the age of the patient, the type of sports or physical activity performed by the patient, the amount of knee pain created by the tear, and the presence of mechanical symptoms (such as clicking, catching, buckling, or locking of the knee). Large, traumatic tears that create clicking, catching, or locking are the most likely to benefit from surgery.
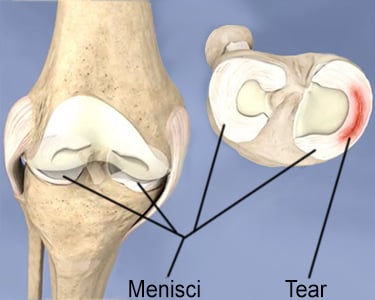
What is the surgery for a torn meniscus?
There are two main types of meniscus surgery, and the appropriate option mostly depends on the specific location, size of the meniscal injury, and morphology of the meniscus tear. The first type of surgery is a partial meniscectomy, which is a “trimming” or “removal” of the torn meniscus. In this surgery, the torn areas of the meniscus are cut and removed using arthroscopic surgical tools and the viable areas of the meniscus are preserved. The second type of surgery is a meniscus repair, in which sutures are placed in the meniscus to fix the tear.
The decision between these two meniscus surgeries is based on the factors listed above, especially the location of the tear on the meniscus and the age of the patient. Not all areas of the meniscus receive the blood flow required for healing after a repair. The periphery of the meniscus is called the “red zone” because it receives blood flow, but this only comprises about 25% of the meniscus. Tears in the red zone have a chance to heal following a repair, so a repair surgery is more likely performed for tears in the red zone. The other 75% of the meniscus is called the “white zone” because it does not receive blood flow. A repair surgery to a tear in this area is more likely to fail, so a partial meniscectomy is often performed for “white zone” meniscal tears.
Video: Meniscal trimming (partial meniscectomy)
How is a meniscus repair done?
There are many ways to perform a meniscus tear repair. The particular surgical technique used largely depends on the size and location of the tear. The surgery begins with knee arthroscopy to examine the meniscus and assess the meniscus tear. There are special suture implants that can be placed through the meniscus tear to allow repair of the meniscus. These implants do not require the surgeon to make additional incisions. For large meniscus tears, the surgeon often must make an additional incision to allow for passing the sutures and tying knots for a more secure repair. These partial open techniques often allow for a more robust repair for larger meniscus tears than would arthroscopic techniques alone.
Video: Meniscal repair animation
What is a meniscectomy?
A meniscectomy, also known as a meniscal debridement, is the removal of the torn meniscus. Often this is only a partial meniscectomy where only the torn pieces are removed. This surgery is often performed through minimally invasive incisions using an arthroscope and arthroscopic instruments. If the damage is too extensive to preserve or repair the meniscus, a total meniscectomy – removal of the entire meniscus – may need to be performed.
What is meniscus transplant surgery?
Because the meniscus acts as a shock absorber for the knee, it protects the cartilage of the knee and prevents the progression of arthritis. Unfortunately, sometimes a patient sustains an injury to the meniscus that leaves little to no viable meniscus left in the knee. When this occurs, the patient is at a high risk of developing knee arthritis. In young patients who have not developed arthritis, the patient is a candidate for meniscus transplant surgery. In this surgery, the surgeon first performs a total meniscectomy and then obtains an appropriately sized meniscus from a cadaver tissue bank, which is placed in the knee. The donor tissue is repaired and sutured into place with the goal of achieving healing of the meniscus within the knee. The recovery process requires an initial period of non-weightbearing and then progression through physical therapy.
What is the meniscus transplant surgery recovery time?
It often takes six to nine months to return to full activity, and most surgeons recommend not playing sports following a meniscus transplant surgery.
How long will I need to stay in the hospital after meniscus surgery?
Most meniscus surgeries can be performed on an outpatient basis, meaning the patient goes home the same day as surgery. Occasionally the patient may stay one night in the hospital if they have additional surgeries that require closer observation.
How long does it take to recover from meniscus repair surgery?
Meniscus repair recovery time is typically six to nine months depending on the activities of the patient. Most meniscus repair surgeries require two to four weeks on crutches with a knee brace for the first six weeks. Physical therapy starts right away to help the knee regain range of motion. Most patients are out of the brace by six to eight weeks. Jogging typically begins around three to four months with return to sports around six to nine months depending on the level of play of the athlete and the type of repair.
What is the recovery time after a meniscectomy?
The recovery time from meniscectomy is typically faster than the recovery time from meniscus repair. Depending on the location of the tear, patients can usually put full weight on the leg right away. Occasionally the patient may need to use crutches for the first week. Most patients start resuming their normal sports activities four to eight weeks after surgery depending on their preferred sports and activities.
How long do I have to wait to drive after meniscus surgery?
Driving after meniscus surgery depends on which leg is operated on and which surgery is performed. Following a meniscectomy (“trimming”) surgery, the patient can typically drive as soon as they are off any narcotic pain medications (typically one to three days). Following a meniscus repair surgery, most patients can return to driving two to three weeks after surgery for a right sided surgery and one to two weeks following a left knee surgery.
How successful is meniscus surgery?
Success rates vary depending on both the type, location and severity of the tear, and which surgery is used to treat it. One study published in 2022 reported a greater than 80% success rate for meniscal repair five years after surgery. For example, greater outcomes were seen among repairs of lateral meniscus tears showed than medial tears.4
What are possible risks or complications with meniscus surgery?
Complications with arthroscopic knee surgery are rare but any surgery comes with risks such as postsurgical blood clots, infections or damage to nerves or other tissues. The key benefits of meniscus surgery include postponing or averting knee arthritis later in life and increasing knee stability.
What will happen if I don’t have meniscus surgery?
Many meniscus tears can be treated without surgery. Conservative options include physical therapy and corticosteroid injections. Significant meniscus tears increase the likelihood that a person will develop knee arthritis in the future. Although some tears do not require surgery, forgoing surgical intervention for a tear that could benefit from trimming or repair may lead to other orthopedic issues later. Younger patients, for example, may end up requiring a partial or total knee replacement earlier than among those who never damaged their meniscus.
Why you should choose HSS for meniscus surgery
Rotator cuff repair is a surgery focused on reducing pain and getting you back to the activities you love. But not all hospitals achieve the same results. Some are more reliable than others. With the help of the HSS Hospital Reliability Scorecard, you can make sure you're asking the critical questions to find the hospital that's right for you. Understanding these data points will help you make the best decision for your care: See hospital reliability data
Explore Related Patient Stories
View All Patient StoriesReferences
- Bansal S, Floyd ER, A Kowalski M, Aikman E, Elrod P, Burkey K, Chahla J, LaPrade RF, Maher SA, Robinson JL, Patel JM. Meniscal repair: The current state and recent advances in augmentation. J Orthop Res. 2021 Jul;39(7):1368-1382. doi: 10.1002/jor.25021. Epub 2021 Mar 19. PMID: 33751642; PMCID: PMC8249336. https://pubmed.ncbi.nlm.nih.gov/33751642/
- Hutchinson ID, Rodeo SA. The Current Role of Biologics for Meniscus Injury and Treatment. Curr Rev Musculoskelet Med. 2022 Dec;15(6):456-464. doi: 10.1007/s12178-022-09778-z. Epub 2022 Jul 26. PMID: 35881326; PMCID: PMC9789233. https://pubmed.ncbi.nlm.nih.gov/35881326/
- Katz JN, Collins JE, Jones M, Spindler KP, Marx RG, Mandl LA, Levy BA, Wright R, Jarraya M, Guermazi A, MacFarlane LA, Losina E, Chang Y. Association Between Structural Change Over Eighteen Months and Subsequent Symptom Change in Middle-Aged Patients Treated for Meniscal Tear. Arthritis Care Res (Hoboken). 2023 Feb;75(2):340-347. doi: 10.1002/acr.24796. Epub 2022 Oct 21. PMID: 34606692; PMCID: PMC8977396. https://pubmed.ncbi.nlm.nih.gov/34606692/
- Nepple JJ, Block AM, Eisenberg MT, Palumbo NE, Wright RW. Meniscal Repair Outcomes at Greater Than 5 Years: A Systematic Review and Meta-Analysis. J Bone Joint Surg Am. 2022 Jul 20;104(14):1311-1320. doi: 10.2106/JBJS.21.01303. Epub 2022 Apr 19. PMID: 35856932. https://pubmed.ncbi.nlm.nih.gov/35856932/
- Su L, Garcia-Mansilla I, Kelley B, Arshi A, Fabricant PD, Sherman SL, Jones KJ. Clinical Outcomes of Meniscal Allograft Transplantation With Respect to the Minimal Clinically Important Difference. Am J Sports Med. 2022 Oct;50(12):3440-3446. doi: 10.1177/03635465211036116. Epub 2021 Sep 8. PMID: 34495780. https://pubmed.ncbi.nlm.nih.gov/34495780/