Ankle Fractures In Children
Ankle fractures are painful and cause short-term disability for people of all ages. But in children, long-term recovery can be complicated if there is associated damage to special tissues.

A child's bone grows at open growth plates. Located at each end of a bone wherever it meets other bones to form a joint (such as the ankle, wrist or knee), these plates eventually close once a person has reached adulthood (that is, when they stop growing).
Whenever a fractured bone includes a portion of a growth plate (also called the "physis"), special care must be taken to ensure that the bone keeps growing properly. Growth arrest – when a bone partially or completely stops growing – is a risk factor in any child who breaks an ankle.
How do I know if my child’s ankle is broken?
If old enough to report the injury, your child may say they twisted and then heard a pop or a crack. They may or may not have fallen down. Depending on the severity of the fracture, your child may or may not be able to walk on the affected leg. However, some children are able walk on a fractured ankle that requires surgical intervention. If the child is too young to communicate how they were hurt (many orthopedic injuries happen too quickly to be witnessed by the care provider), they may refuse to walk on the affected extremity.
Usually, the ankle will swell shortly after the injury. Sometimes there will be numbness in the foot or toes. This may be due to swelling or nerve injuries that may occur with higher energy ankle fractures. If your child is unable to walk or reports pain with ambulation, you should go to the emergency room or an urgent care center.
The following are examples of broken ankle injuries that require extra attention and possible treatment.
Types of fractures
The two chief types of fractures in the ankle are distal tibial fractures and distal fibula fractures, each of which can be nondisplaced or displaced.
Distal tibial fracture
This type occurs in two varieties:
- nondisplaced – in which the fractured bone fragments are aligned
- displaced – in which the fractured bone fragments are misaligned or separated
A nondisplaced distal tibial fracture at the ankle can look like an ankle sprain, with mild swelling accompanied by pain when the child stands or tries to walk. X-rays will show very subtle signs that a fracture is present. A physical exam by a specialist is critical in order to make the diagnosis. Treatment usually requires that the child wear a cast and/or a brace or "walking boot" for three to four weeks. Growth arrest in this type of fracture is uncommon.
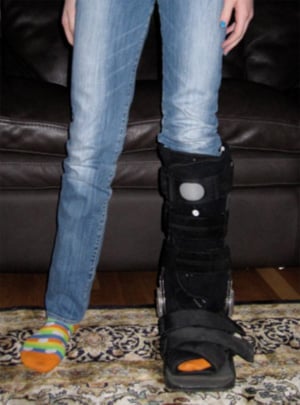
A typical brace or "walking boot" worn to allow a nondisplaced distal tibial fracture to heal.
An accurate assessment of any ankle fracture is essential, because most displaced ankle fractures in children require surgery to correct the anatomic alignment of the bone. In displaced fractures, it is common for the bones to stop growing properly (partial growth arrest). In order to monitor for and detect any permanent damage to the growth plate and optimize healing, any child or teenager who has a displaced ankle fracture must have follow-up clinical exams and radiographic imaging (X-rays) for one to two years.
Displaced distal tibial fractures at the ankle joint range from mild fractures that can be treated with casting to more serious fractures (Tillaux fractures, triplane fractures) that require more detailed radiological imaging – including CT or MRI – and may require eventual surgery.
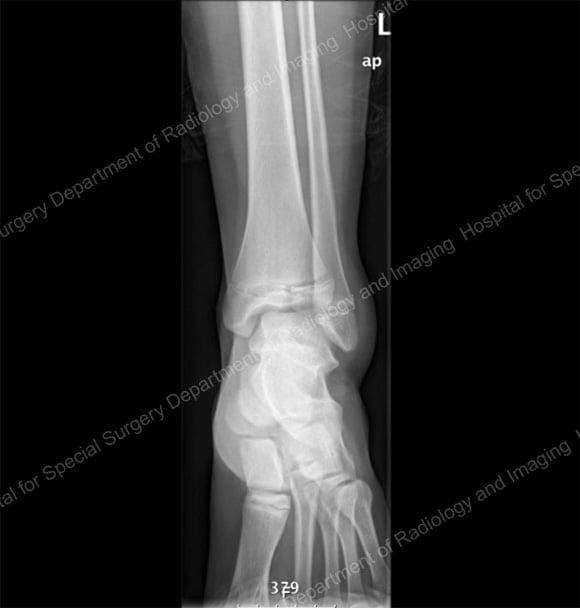
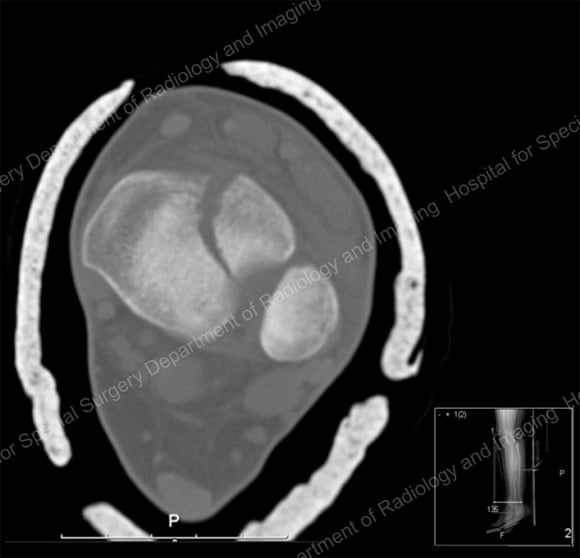
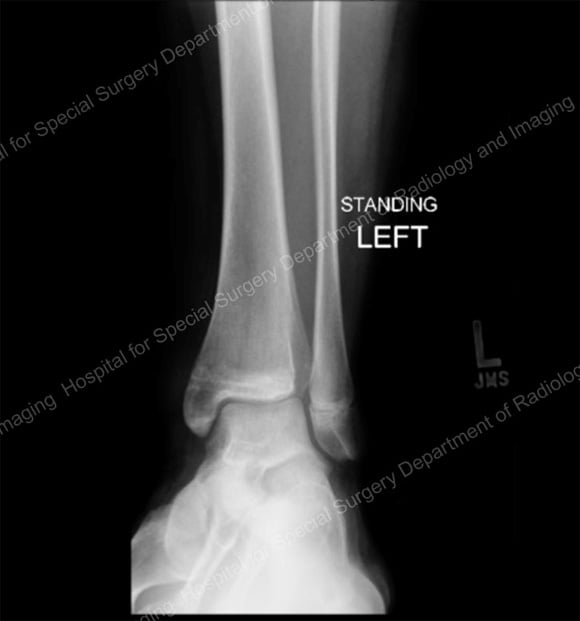
Anterior X-ray (image 1) and cross-sectional CT scan (image 2) of a minimally displaced distal tibial fracture that affected the growth plate and ankle joint.
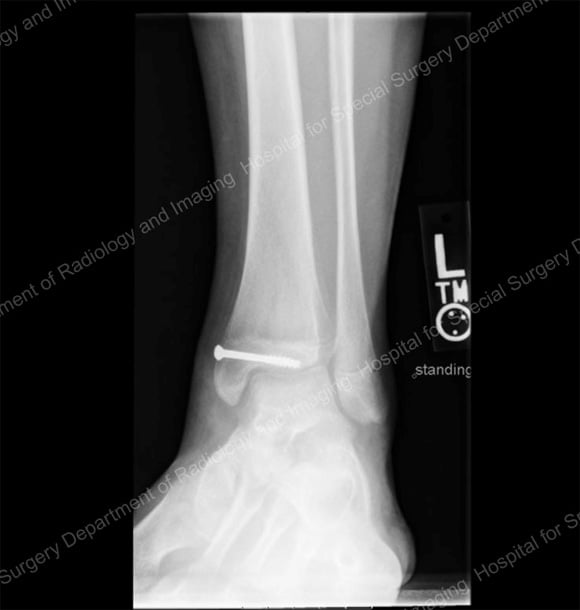
X-rays showing surgical correction of the tibia with screws (image 3) and the tibia after the fracture has healed and the screw has been removed (image 4).
Distal fibula fracture
This type of ankle fracture also occur in nondisplaced and displaced varieties.
Nondisplaced fractures of the distal fibula can look a lot like ankle sprains. Generally they are treated the same way as nondisplaced tibia fractures, with three weeks of a functional brace or cast. Patients with nondisplaced distal fibula fractures should have follow-up for up to two years to watch for any growth disturbances.
Displaced distal fibula fractures are usually treated with surgery if the fracture extends into the ankle joint. In these cases, the most common goal of surgery is to restore a smooth, properly aligned, joint surface. If the displacement does not extend into the joint, a pediatric orthopedic surgeon can often realign the bone fragments and hold them with a cast.
If you wish to find a doctor at HSS who treats broken ankles in a growing child or teenager, be sure to select a pediatric orthopedic surgeon. These are specialists in pediatric skeletal abnormalities and fractures who can diagnose, treat, and provide appropriate follow-up care for your child to minimize future growth problems. If you prefer to call, you may also contact our Physician Referral Service, who can direct you to an appropriate doctor in the Pediatric Orthopedic Surgery Service at Hospital for Special Surgery.

