Knee Revision (Revision Total Knee Replacement)
Medically reviewed by Amar S. Ranawat, MD

Total knee replacement is one of the most successful procedures in orthopedic medicine. This is due to the substantial pain relief and restoration of function patients experience after a knee replacement. With newer implant designs and improved surgical techniques, total knee replacements can be expected to function well for at least 15 to 20 years in more than 85% to 90% of patients.
This means that people who have a knee replacement at a younger age may eventually need a second operation to clean the bone surfaces and refixate the implants. In patients where the original implant fails, a revision knee replacement surgery may be necessary.
What causes a knee replacement implant to fail?
The primary causes of knee implant failure are wear and loosening, infection, instability, leg fractures, or stiffness.
Wear and loosening
Properly functioning implants depend on their appropriate fixation to the bone. Fixation is usually achieved by cementing the implant onto the bone. Some surgeons prefer instead to use biologic fixation, meaning no cement placed between the implant and the bone.
Although implants are firmly fixed at the initial knee replacement surgery, they may become loose over time. The cause of loosening may not always be clear but high impact activities, excessive body weight and wear of the polyethylene component may all act as contributing factors. Friction caused by the joint surfaces rubbing against each other wears away the surfaces of the implant, creating tiny particles that accumulate around the joint. In a process called aseptic (non-infected) loosening, the bond of the implant to the bone is destroyed by the body's attempt to digest these wear particles. During this process, normal, healthy bone is also digested (a condition called osteolysis), which can weaken or even fracture the bone.
When the prosthesis becomes loose, the patient may experience pain, change in alignment, or instability.
Infection
With current surgical techniques and antibiotic regimens, the risk of infection from total knee replacement is less than 1%. When it does occur, however, infection is a devastating complication of any surgical procedure. In a total knee replacement, the large metal and plastic implants can serve as a surface for the bacteria to latch onto – a process known as biofilm formation. The location of these bacteria make them inaccessible to antibiotics. Even if the implants remain well-fixed, revision surgery is necessary to stop the pain, swelling and drainage from the infection.
Revision surgery of the infected knee can take several forms. Depending on the degree of infection and damage, the surgeon will determine one of two basic courses of action:
- perform a simple washout of the knee while keeping the original prosthetic components in place
- completely exchange the implants with new ones in a full knee revision operation
A complete revision for infection will involve either a single-stage or two-stage operation, depending on the severity of the infection and the virulence of the bacteria. In the single-stage operation, the prior infected components are removed as part of a thorough debridement, the knee is thoroughly cleaned, and new revision components are placed in one operative setting (that is, on the same day). In the two-stage operation, two separate operations are performed weeks apart: The first operation is to remove the old prosthesis and insert a block of cement with antibiotics (known as an antibiotic-impregnated cement spacer). The second surgery is to remove the spacer and insert a new prosthesis. Intravenous antibiotics are frequently given during both options to eradicate the infection.
Instability
Instability occurs when the soft-tissue structures around the knee are unable to provide the stability necessary for adequate function during standing or walking. Instability may be the result of increased soft-tissue laxity (looseness), or improper positioning or alignment of the prosthesis. The soft tissues, including the ligaments around the knee, may stretch out after surgery and no longer provide the support that the knee needs. Pain and/or a sense of the knee "giving away" may affect knee function. If these symptoms cannot be successfully treated through nonsurgical means such as using bracing or physical therapy, revision surgery may be required.
Leg fractures
The type and extent of the fracture will determine whether revision surgery is needed. Periprosthetic fractures (fractures around the knee implants) that disrupt the fixation or the stability of the implant may require revision surgery.
Stiffness
In some instances, a total knee replacement may not allow for you to achieve the range of motion needed to fulfill your daily activities. This can happen if excessive scar tissue builds up around the knee that prevents the joint from moving fully. When this occurs, some patients may benefit from knee manipulation under anesthesia. For this procedure, the patient returns to the operating room and the surgeon uses their hands to physically flex and straighten the knee to help it regain flexibility.
If excessive scar tissue has built up around the knee joint and has significantly impaired motion and you have not had much success with manipulation, revision surgery may be considered to enable you to regain the motion to perform your everyday activities.
What are the risk factors for a failed knee replacement?
Age, activity level, surgical history and a person’s weight can contribute to implant failure. Younger, active patients, people who are obese, and those who have had prior knee surgeries all have a higher increased risk of a failed implant.
Younger, more active patients have a higher rate of revision than older, less active patients because they place more stress on their prosthesis over more time. Obese patients have a higher incidence of wear and loosening because of the increased force of their weight, and they are more prone to infections because of their increased risk of wound healing. Patients with previous knee surgeries are at higher risk for infection and implant failure.
What are the signs of knee replacement failure?
The most common symptoms of a failed knee implant are pain, decrease in joint function, knee instability, and swelling or stiffness in the knee joint.
Persistent pain and swelling can indicate loosening, wear or infection, and the location of the pain can be all over the knee (generalized) or in one particular area (localized). A decline in knee function may result in a limp, stiffness or instability. Patients who demonstrate these symptoms and signs may require revision joint surgery.
How is a failed knee replacement treated?
When a total knee replacement prosthesis fails, a second knee surgery is required. The most common and effective treatment is called revision total knee replacement (also known as knee revision surgery).
What is revision knee replacement?
Revision total knee replacement is the replacement of a failed total knee prosthesis with a new prosthesis. In simple terms, it is the replacement of a total knee replacement (or a "second knee replacement").
Knee revision surgery is a complex procedure that requires extensive preoperative planning, specialized implants and tools, prolonged operating times, and mastery of difficult surgical techniques to achieve a good result.
What does the doctor do prior to revision surgery?
When the decision for revision knee replacement is made, the surgeon will do a thorough clinical exam and order X-rays and laboratory tests. If infection is suspected, aspiration of the knee (joint fluid removed with a needle) may be required. The aspirated fluid will then be sent to a laboratory for analysis to identify the specific type of infection.
In addition to X-rays, other imaging modalities may be helpful, such as bone scans, CT scans or Magnetic Resonance Imaging (MRI). These advanced imaging technologies can demonstrate changes in the position or condition of the prosthetic components as well help to pinpoint the cause, location and the amount of bone loss to help plan for the surgery.
What happens during knee revision surgery?
First, the old implant is removed and, if needed, bone grafts are used to fill any voids where bone has deteriorated. Then the new prosthesis is placed.
Most revision total knee replacements take longer to perform than primary procedures (about two to three hours).
Overview of knee revision surgery
The first step is removal of the existing implant. If there has been significant bone loss, bone grafts may be required to fill these voids. Bone grafts can be either autografts (your own bone tissue, taken from another part of your body) or an allograft (bone tissue from another person obtained from a bone bank). In some cases, metal wedges, wires or screws may be used to strengthen the bone.
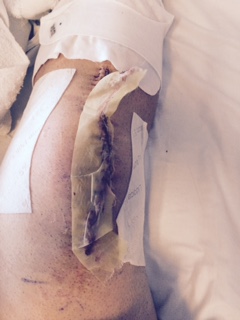
Finally, specialized revision knee implants are inserted. Temporary drains may be placed to help prevent excessive swelling of the knee and are usually removed a few days after surgery. Additionally, specialized negative pressure incisional dressings are also frequently employed to improve wound healing as they have been shown to decrease post-operative wound complications in high-risk patients. These dressings are usually connected to a small portable pump that stays on for about a week and keep the wound protected and dry.
Knee revision surgery video
This video demonstrates a step-by-step animation of a revision total knee replacement operation.
What happens after knee revision surgery?
Postoperative care is very similar to that after a primary knee replacement. This includes physical therapy, blood management, pain medication as necessary, antibiotics and some method of blood clot prevention. A brace or splint may be used to protect the joint after the surgery.
What is the recovery time after knee revision surgery?
It varies, but in most cases, physical therapy will be initiated within 24 hours of the procedure and will continue for up to three months.
Some patients take longer to recover. In some cases, protective weightbearing or limiting the knee’s range of motion is needed to promote appropriate healing. Therapy will usually continue for up to three months following the surgery. Assistive devices, such as a walker or crutches, will be used early in the convalescence period, and patients will progress to a cane or walking without any assistance as their condition improves.
What are the risks and complications of revision knee replacement?
Any surgery can have potential complications. The complexity of revision joint surgery increases the chance of surgical complications, which include but are not limited to:
- wound drainage
- infection
- bleeding
- damage to nerves or blood vessels
- intra-operative fractures
- blood clot (deep vein thrombosis, DVT)
- pulmonary embolism
Infection, bleeding, damage to nerves or blood vessels, and intra-operative fractures can be minimized by using antibiotics before and after surgery, employing sterile surgical techniques and utilizing well-planned surgical exposures. Patients who are obese are particularly at increased risk of infection and wound drainage issues postoperatively.
Similar to primary knee replacement, some mild swelling of the knee or ankle may be present after surgery for as long as three to six months. Swelling can be treated by elevating the leg, applying an ice pack, and wearing compression stockings.
Prior medical conditions, such as heart and lung complications or stroke conditions, can be aggravated by a revision procedure. These conditions may also develop in patients after revision surgery. Very rarely, death can occur. The decision to perform revision joint surgery is made when the benefits of pain relief and functional improvement outweigh the risk of potential complications.
What should I expect after knee revision surgery?
Most patients who undergo revision procedures can expect to have good to excellent results. Although expected outcomes include pain relief with increased stability and function, complete pain relief and restoration of function is not always possible.
Up to 20% of patients may still experience some pain following revision knee surgery. This can persist for several years after the procedure. Additionally, recovery after revision total knee surgery is heavily dependent on the state and function of the knee prior to the revision surgery.
What are the alternatives to revision surgery?
Alternatives to revision knee surgery are rarely used as they can sometimes be more complex and lead to worse results than revision surgery, but they include knee fusion or amputation.
The following alternatives are employed depending on the seriousness of the problem affecting the knee:
- Arthrodesis (fusion) of the knee joint may relieve pain but at the expense of keeping the knee in a fixed, non-bending position.
- Amputation may be used in extreme cases in which the knee joint has a severe infection that cannot be eradicated
Conclusion
Although total knee replacement is a highly successful operation in the majority of patients, some procedures will fail. Certain signs and symptoms such as an increase in pain or a decrease in knee function may be indicative of joint failure. There are several reasons for the failure of knee implants such as infection, instability, stiffness, wear and loosening, and leg fractures .
Advanced techniques and materials for revision knee surgery usually allow for substantial pain relief and improved function; however, this may not always be possible. Revision total knee replacement is a complex procedure that requires an experienced surgeon and proper preoperative planning to achieve satisfactory outcomes.
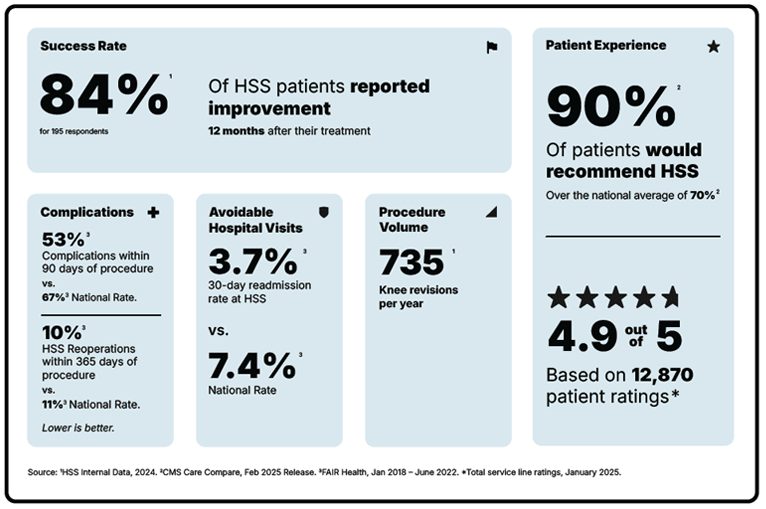
Why you should choose HSS for knee revision
Knee revision is a surgery focused on reducing pain and getting you back to the activities you love. But not all hospitals achieve the same results. Some are more reliable than others. With the help of the HSS Hospital Reliability Scorecard, you can make sure you're asking the critical questions to find the hospital that's right for you. Understanding the data points will help you make the best decision for your care.
See hospital reliability data
Explore Related Patient Stories
View All Patient StoriesReferences
- Barrack RI, Brumfield CS, Rorabeck CH. "Heterotopic Ossification After Revision Total Knee Arthroplasty." Clinical Orthopaedics and Related Research. 2002:208–213.
- Bookman JS, Schwarzkopf R, Rathod P, Iorio R, Deshmukh AJ. Obesity: The Modifiable Risk Factor in Total Joint Arthroplasty. Orthop Clin North Am. 2018;49:291–296.
- Hamilton DF, Howie CR, Burnett R, Simpson AHRW, Patton JT. Dealing with the predicted increase in demand for revision total knee arthroplasty: challenges, risks and opportunities. Bone Joint J. 2015;97-B(6):723–728.
- Hartley RC, Barton-Hanson NG, Finley R, Parkinson W. "Early Patient Outcomes After Primary and Revision Total Knee Arthroplasty. A Prospective Study." Journal of Bone and Joint Surgery, British Volume. 2002; 84: 994–999.
- Jiranek WA, Hanssen AD, Greenwald AS: Antibiotic-Loaded Bone Cement For Infection Prophylaxis in Total Joint Replacement. J Bone Joint Surg Am 2006, 88:2487-2500.
- Katz BP, Freund DA, Heck DA. "Demographic Variation in the Rate of Knee Replacement: A Multi-Year Analysis." Health Services Research. 1996; 31:125–140.
- Kim J, Nelson CH, Lotke PA (2004) Stiffness after total knee arthroplasty: prevalence of complication and outcome of revision. J Bone Joint Surg 86-A:1479–1484.
- Kurtz S, Ong K, Lau E, Mowat F, Halpern M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am. 2007;89(4):780–785.
- Leopold SS, Rosenberg AG, Bhatt RD, Sheinkop MD, Quigley LR, Galante JO: Cementless acetabular revision: Evaluation at an average of 10.5 years. Clin Orthop 1999; 369:179-186
- Lee D-H, Lee S-H, Song E-K, Seon J-K, Lim H-A, Yang H-Y. Causes and clinical outcomes of revision total knee arthroplasty. Knee Surg Relat Res. 2017;29(2):104–109.
- Newman JM, Siqueira MB, Klika AK, Molloy RM, Barsoum Wk, Higuera CA. J Arthroplasty. Use of closed incisional negative pressure wound therapy after revision total hip and knee arthroplasty in patients at high risk for infection: a prospective, randomized clinical trial. 2019;34:554–559.
- Peersman G, Laskin R, Davis J. "Infection in Total Knee Replacement: A Retrospective Review of 6489 Total Knee Replacements." Clinical Orthopaedics and Related Research. 2002; 392:15–23/
- Ranawat AS, Ranawat CS. "Total Knee Arthroplasty for Severe Valgus Deformity". Journal of Bone and Joint Surgery. 2005; 87:271-284.
- Ranawat CS, Flynn WF, Saddler S. "Long-term results of the total condylar knee arthroplasty: a 15-year survivorship study". Clin Orthop. 1993;286:94-102.
- Sheth NP, Bonadio MB, Demange MK. Bone loss in revision total knee arthroplasty: evaluation and management. J Am Acad Orthop Surg. 2017;25(5):348–357. doi: 10.5435/JAAOS-D-15-00660.
- Skinner J, Weinstein JN, Sporer SM, Wennberg JE. Racial, ethnic, and geographic disparities in rates of knee arthroplasty among Medicare patients. New England Journal of Medicine. 2003; 349:1350 -9.
- Taunton, M. What’s new in Adult Reconstructive Knee Surgery. The Journal of Bone and Joint Surgery. 2019; 103-11.