Lupus and Contraception: Essentials for Patients
- Key points
- The effectiveness of different contraception methods varies
- Lupus patients are less likely to use effective contraception
- Contraception: The basics
- Types of contraception
- General risks of contraceptives
- Specific contraception risks for women with lupus
- Final word
Key points
- Safe and effective contraception is important for all women with lupus, especially those with organ damage, active lupus or medications that may negatively affect a pregnancy. Having ongoing discussions between the patient, her rheumatologist, and her gynecologist is the best way to ensure that the most appropriate, safe, effective and acceptable contraceptive methods are used.
- Long-acting reversible contraceptives (LARC) are recommended for all women with lupus (unless gynecology contraindications are present). Intrauterine devices (IUDs) are safe and effective and may be used in women on immunosuppressive medications. The relatively new progestin implant has not been studied in women with lupus.
- Combined hormonal contraceptives such as the birth control pill may be used in some patients with lupus, but should not be used in those with very active disease or increased risk for blood clots including those with positive antiphospholipid antibodies, a history of blood clots, or other risk factors.
- The progestin-only IUD and pill are good alternatives for most patients who cannot take estrogen and may help to decrease heavy menstrual blood loss in patients on warfarin.
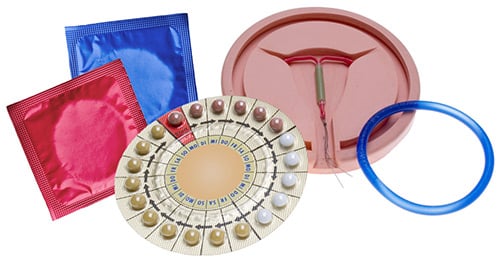
The effectiveness of different contraception methods varies
Safe and effective contraception is important for all women, including women with systemic lupus erythematosus (lupus, sometimes also abbreviated as SLE). The effectiveness of available contraceptives varies, however, and specific details of a woman’s underlying lupus may influence the safety of certain methods.
The most effective contraceptives are the long-acting reversible contraceptives (LARC), which include intrauterine devices (IUDs) and the progestin-containing subdermal implant (a thin progestin-containing rod that is implanted under the skin of the inner upper arm). Unintended pregnancy rates with use of LARC methods are less than 1% per year. Slightly less effective methods (with unintended pregnancy rates of 4% to 8% per year) include combined hormonal contraceptives, such as the birth control pill, and the progesterone-only pill.
Barrier methods such as condoms are the least effective contraceptives, with unintended pregnancy rates of 15% to 20% per year. However, they are the only method to offer some protection against sexually transmitted diseases. "Natural" or "fertility awareness" methods (such as the "rhythm method," in which a woman monitors her menstrual cycle to gauge when she is most likely to get pregnant) are even less effective and are not generally recommended as acceptable forms of contraception for lupus patients.
The best contraceptive for a woman with lupus will depend on whether she tests positive for antiphospholipid antibodies (which may increase risk for blood clotting complications), her level of disease activity, her medical history, current medications, and her personal preference.
Lupus patients are less likely to use effective contraception
Use of effective contraception is less common in women with lupus compared to the general population. This is true even among women who are taking potentially teratogenic medications (medications that may cause birth defects in the newborn when taken during pregnancy). This may be due at least in part to the fact that until recently all lupus patients were advised to avoid estrogen-containing contraceptives such as the traditional birth control pill due to concerns over increased risks of lupus symptom flares or blood clots.
Despite advances in knowledge about safety, however, many lupus patients still do not utilize effective birth control. For example, one survey of 86 women with lupus who were at risk for unplanned pregnancy found that 22% used any contraception inconsistently, and 55% depended solely on the least effective barrier methods (usually condoms). Most importantly, women taking teratogenic medications were no more likely to use effective contraception than women not on these medications.
Women with lupus are at greater-than-average risk for pregnancy loss and complicated pregnancies. Rates of preterm birth, preeclampsia (high blood pressure during pregnancy), and small for gestational age infants are higher for lupus mothers. Research has shown risk factors for pregnancy complications to include active lupus, kidney disease, antiphospholipid antibodies, teratogenic medications and others. Doctors will recommend against a pregnancy in a woman with lupus when the disease is very active, or when teratogenic medications are being used. Some of these risk factors may be addressed while pregnancy is deferred using effective contraception, allowing for a safer and more successful pregnancy in the future. Therefore, whenever women with lupus and their doctors discuss reproductive health and future pregnancy, the discussion should include the importance of a planned pregnancy.
Why, then, do women with lupus use effective contraception less (and not more) often than the general population? Women with other chronic health problems also have lower rates of effective contraceptive use. This suggests that, in such cases, the doctor’s and patient’s focus on the challenging, chronic illness may take precedence over more basic health discussions, especially among patients with an illness that may flare unexpectedly. Another possible explanation is that rheumatologists may feel they do not have the time or the knowledge to discuss these issues with their patients, deferring instead to the patient’s Ob/Gyn. Most Ob/Gyns, however, do not have the specialized knowledge of lupus that rheumatologists have, and they may also be hesitant to advise patients when they have an incomplete understanding of the underlying disease.
Efforts are underway to remedy these gaps in counseling and use of effective contraception. The recently published guideline from the American College of Rheumatology on reproductive health in patients with rheumatic and musculoskeletal diseases strongly encourages discussion and planning regarding reproductive issues as well as ongoing discussion between the patient, her rheumatologist and her Ob/Gyn. In addition, the Food and Drug Administration (FDA) has mandated patient education regarding the importance of effective contraception for certain medications, most notably mycophenolate mofetil, since this medication not only may cause birth defects but may interfere with the effectiveness of certain contraceptives. This education program is called the Mycophenolate Risk Evaluation and Mitigation Strategy (Mycophenolate REMS).
Contraception: The basics
Not all contraceptives are created equal. Effectiveness varies widely, so every discussion of contraception will include guidance on the most effective and the safest methods for a given individual. The effectiveness of contraceptive methods is characterized in two ways: There is the "perfect use" (or theoretical) effectiveness, which is the method’s effectiveness when used exactly as prescribed, and there is the "typical use" (or actual) effectiveness that reflects "real world" use, including forgotten pills or misplaced diaphragms.
Perfect-use and typical-use effectiveness are more closely aligned in methods that are not directly related to the act of intercourse (such as oral contraceptives), and they are nearly identical for LARC, which includes methods that require no ongoing effort on the part of the patient (such as an IUD). LARC is widely considered the most effective form of contraception, but despite this, the oral contraceptive pill is still the most common reversible contraceptive method used by women of childbearing age in the United States. The rate of IUD use in the United States has steadily increased from 1995 (when it was less than 1%) to the present rate of about 10%.
Types of contraception
Barrier methods
Barrier methods include the condom, diaphragm and others. Despite their lower effectiveness, condoms offer certain advantages. The male condom is easily available (no prescription or procedure needed) and it provides some protection against sexually transmitted diseases including human immunodeficiency virus (HIV). Effectiveness of barrier contraception is increased if two methods are used, for example, a condom and spermicide. As a result, this is a common recommendation for women who wish to use barrier protection.
Intrauterine devices
The intrauterine device (IUD) is an effective form of birth control and is approved for women, including adolescents, who have not had children, with few contraindications to use. It is the most used form of reversible contraception worldwide. IUDs contain either copper or levonorgestrel, a type of progestin. The less expensive copper-containing IUDs may remain in place for 10 years but are associated with heavier menstrual bleeding and cramps, especially in the first several months. The levonorgestrel-containing IUDs remain in place for 3 to 5 years. An advantage is that these IUDs generally reduce menstrual bleeding and cramps, with loss of menses in up to 50% of women after two years of use. Systemic side effects are minimal, and fertility quickly returns to normal with removal of the device.
Rates of complications associated with IUD use are extremely low and include risk of expulsion of the device and risk of infection. Of note, IUD use is discouraged in women at higher risk for sexually transmitted diseases, that is, those with multiple sexual partners. Although there are no specific data on risk of infection with IUD use in lupus patients treated with immunosuppressive medications, some studies have shown there is no increased risk of infection in immunocompromised HIV-infected women or women with organ transplants on immunosuppressive medications.
Hormonal contraception
Hormonal contraception is generally divided into two major categories:
- combined estrogen-progestin
- progestin-only
Hormonal contraceptives may be administered through a variety of methods. Limited to "the pill" in years past, hormonal contraceptives may now be given orally or through a skin patch, vaginal ring, injection, subdermal implant or IUD (as described above).
Combined hormonal contraceptives
The first birth control pill contained 3 to 5 times the estrogen content of most current oral contraceptives. Current combined oral contraceptives contain a synthetic estrogen and one of a number of progestins. Potential side effects of progestins differ, which may influence suitability for use in women with lupus.
Newer formulations of birth control pills tend to be "multiphasic" – that is, they vary the amounts of estrogen and progestin over the course of the menstrual cycle. Extended-cycle preparations can safely limit menses to several times per year. Newer delivery methods for combined hormonal contraceptives include the transdermal (skin) patch and the intravaginal ring. In general, the skin patch (but not the vaginal ring) is associated with a higher blood level of estrogen, which may be relevant for lupus patients in terms of flare and/or clotting issues.
Risk of serious complications with combined hormonal contraceptives is low and may be further limited when physicians carefully assess patients to exclude those at greatest risk. Serious complications are usually vascular in nature, including blood clots in the veins, strokes and heart attacks. Most of the blood clot risk is due to the estrogen component, although certain progestins may also slightly influence the risk of clotting. There is minimal increased risk of cervical cancer and breast cancer in active users of combined hormonal contraceptives, but not in former users.
Importantly, the risk of blood clots is further increased if a woman has pre-existing risk factors for clotting, including antiphospholipid antibodies (aPL), which are present in about one-third of lupus patients. This risk is also increased in people who smoke tobacco, are greater than 35 years of age, or who are obese. The risk of stroke is also increased among people who have high blood pressure or migraine headaches, smoke tobacco or are over 35 years of age.
Progestin-only contraceptives
Progestin-only contraceptives are an alternative for women who cannot or prefer not to take estrogen-containing preparations. Medical authorities such as the Centers for Disease Control and Prevention and The World Health Organization agree that most progestin-only contraceptives are safe and effective for patients who are at increased risk for blood clots in the veins or arteries, although there are few studies to support this. For those who take the progestin-only pill (also called the "mini-pill"), it is important to do so at the same time each day in order for it to be effective. Unlike combined hormonal contraceptive pills, the progestin-only pill is safe to use while breastfeeding.
An injection form of progestin-only contraceptive, depo-medroxyprogesterone acetate (DMPA), administered every three months, is very effective. The progestin IUD, described above, is highly effective as is the subdermal implant, which releases a progestin (etonogestrel) over a three-year period.
Minor side effects tend to be more common with progestin-only than with combined contraceptives – primarily irregular, "break-through" bleeding. (This is the most common reason why some patients discontinue use.) Importantly for lupus patients, DMPA (but not the progestin-only pill or progestin IUD) may cause reversible bone loss of up to 7.5% over two years in healthy women. A history of fracture, osteoporosis or having strong risk factors for osteoporosis (such as corticosteroid use) are relative contraindications to the use of DMPA. An additional disadvantage of DMPA is that there may be a delayed return to fertility. It is not recommended for patients who plan pregnancy within the next year. The subdermal progestin implant is relatively new and has not been well studied in the general population. It has not yet been studied at all in women with lupus.
Finally, risk for blood clots with progestin-only contraceptives, while clearly much lower than for combination hormonal contraceptives, is somewhat controversial due to a lack of studies in women with lupus and/or aPL. However, in women with other known risk factors for blood clots, the progestin-only pill and IUD do not further increase clot risk. DMPA, however, may confer an increased risk, although data are very limited due to small numbers of patients in studies.
Emergency contraception
Emergency contraception, used to prevent pregnancy after unprotected intercourse, is available and may be used by any woman with lupus. Options include physician placement of a copper IUD, prescription-only oral selective progesterone receptor modulators, and, most commonly, non-prescription oral levonorgestrel (available over the counter) to be taken within 72 hours. Cardiovascular disease and increased risk for blood clots are not contraindications to the use of any form of emergency contraception and even women with antiphospholipid antibodies may use these.
General risks of contraceptives
While combined hormonal contraceptives are an effective and generally safe form of birth control for many women, they are not for everyone, even among women who do not have lupus. Between 10% to 20% of all women, not just those with lupus, may be ineligible for combined hormonal contraceptives based on traditional contraindications such as high blood pressure or migraine headaches, among others. In addition to these traditional contraindications, a proportion of lupus patients will be ineligible based on the presence of aPL and of active or severe disease.
Specific contraception risks for women with lupus
Certain issues are of obvious concern when evaluating risks of contraceptive methods in women with lupus. Fortunately, LARC, preferred due to their greater effectiveness, may be used by any woman with lupus regardless of her level of disease activity or aPL status. Estrogen-containing hormonal contraceptives are options for some lupus patients who cannot or choose not to utilize LARC. However, the presence of aPL (with their associated blood clotting risk) is a strong contraindication to the use of estrogen methods. Estrogen-progestin contraceptives have not been studied in women with active lupus and so are also discouraged in this setting. Hormonal contraceptives may interact with some lupus medications, so potential interactions must be carefully evaluated. Contraception risks for women with lupus may include:
Risk of lupus flare
Early studies – mostly case reports of patients – suggested a risk of disease flare in lupus patients exposed to combined oral contraceptives and were attributed to the possible immunostimulatory effect of the estrogen. However, two controlled studies published in 2005 demonstrated no increased flare risk with use of combined hormonal contraceptives in lupus patients with quiet or stable (low level) disease activity. To minimize risk of increased disease activity, it would seem prudent to avoid combined hormonal contraceptive methods with higher estrogen exposures than were used in the published studies, particularly the transdermal patch with its overall higher estrogen exposure. In contrast to estrogen, progestins have not been suggested to increase risk of flare in lupus patients.
Risk to serum potassium levels
The type of progestin used may be of concern for some lupus patients. The progestin drospirinone may rarely cause elevated serum potassium levels in susceptible individuals. Women taking medications that increase serum potassium or alter kidney function or women with underlying kidney disease may require monitoring of serum potassium if taking drospirinone-containing oral contraceptives.
Risk of infection
The progestin IUD appears to be safe for lupus patients. Although risk of infection (pelvic inflammatory disease, or PID) is not well studied in lupus patients on immunosuppressive medications, extrapolation from safety studies in other immunocompromised patient groups suggests no increased risk of infection.
Risks to bone health
Due to the risk of decreased bone density and the potential increased risk of blood clots, DMPA is not a good long-term option for patients with osteoporosis or long-term corticosteroid use. There are no data yet on the etonorgestrel subdermal implant in lupus patients.
Risk of blood clots
Antiphospholipid antibodies (aPL) are well recognized as risk factors for blood clots and pregnancy loss or complications in patients with antiphospholipid syndrome (APS). There are three common tests for aPL: anticardiolipin antibody, anti-Beta-2-glycoprotein-I (aβ2GPI) antibody and lupus anticoagulant.
About a third of patients with lupus have aPL, though fewer have the clinical syndrome, APS. Diagnosis of APS depends on having both aPL antibody and typical complications. It is challenging to predict the risk of blood clots or pregnancy complications for an asymptomatic aPL-positive woman, but risk appears to be highest for those with lupus anticoagulant and/or high titer IgG anticardiolipin antibody. Having other risk factors for blood clots, whether genetic, medical, or external factors, may further increase likelihood of blood clots. Medical factors that may increase risk include underlying cancer, pregnancy, and kidney issues causing significant urinary protein loss. External factors include cigarette smoking, estrogen use, surgery, and prolonged bedrest.
Because of the known potential risks, no controlled studies have been done to measure the direct risk of estrogen-containing contraceptives in patients with aPL. Case reports have described aPL-positive patients who took oral contraceptives developing blood clots, including stroke. Among younger women (less than 50 years old) who have a positive lupus anticoagulant, the odds of their having a stroke is 43 times (43x) greater than other women in the same age group; for women with lupus anticoagulant who also take an oral contraceptive, the risk rises to 201x. (Keep in mind that the risk of stroke among the general population of women in this age group is extremely low, so while these elevated risk rates are significant, the number of women with lupus in this age range who have strokes is still relatively low.)
In contrast to the clear increased clotting risk with estrogen use, the progestin-only pill and IUD are generally accepted as safer methods of birth control for those already at increased risk of blood clots. Progestin methods offer another advantage for patients on blood-thinning medication such as warfarin: they often reduce heavy menstrual blood flow.
Medication interactions
Interactions of hormonal contraceptives with other medications are well recognized and may lead to decreased effectiveness of either the contraceptive itself or the other medication. Since many lupus patients are on multiple medications, it is important to check for interactions.
One medication commonly used in lupus patients with a potential interaction with estrogen-progestin contraceptives is mycophenolate mofetil. Because of possible interaction with both estrogen and progestins, an IUD or use of two methods of birth control, at least one of which should be non-hormonal (such as a condom), is suggested for patients taking mycophenolate.
Other medications with possible interactions include anti-seizure medications and cyclosporine. Most antibiotics, except for rifampin, do not significantly change contraceptive effectiveness. Certain herbal medications may increase the clearance of oral contraceptives and negatively impact effectiveness, for example St. John’s Wort.
Final word
The issues surrounding choice of contraception are complex, especially for women with lupus. Yet it is important to understand the options and their potential risks and benefits in order to make the best choice. Fortunately, a woman does not have to do this alone. She can work as a team with her rheumatologist and Ob/Gyn to determine what is best for her particular combination of medical considerations and preferences, feeling safe and confident in her reproductive health management.
References of interest
Sammaritano LR. Contraception in patients with rheumatic disease. Rheumatic Disease Clinics. 2017 May 1;43(2):173-88.
Yazdany J, Trupin L, Kaiser R, Schmajuk G, Gillis JZ, Chakravarty E, Schwartz, EB. Contraceptive counseling and use among women with systemic lupus: a gap in health care quality? Arthritis Care Res 2011;63(3):358-365.
Sammaritano LR, Bermas BL, Chakravarty EE, Chambers C, Clowse ME, Lockshin MD et al. 2020 American College of Rheumatology Guideline for the Management of Reproductive Health in Rheumatic and Musculoskeletal Diseases. Arthritis and Rheumatology. 2020 Apr;72(4):529-556.
Petri M, Kim MY, Kalunian KC, Grossman J, Hahn B, Sammaritano L, et al. Combined oral contraceptives in women with systemic lupus erythematosus. N Engl J Med 2005;353:2550-2558.
Sanchez-Guerrero J, Uribe AG, Jimenez-Santana L, Mestanza-Peralta M, Lara-Reyes P, Seuc AH, et al. A trial of contraceptive methods in women with systemic lupus erythematosus. N Engl J Med 2005;353:2539-2549.
Urbanus RT, Siegerink B, Roest M, Rosendaal FR, de Groot PG, Algra A. Antiphospholipid antibodies and risk of myocardial infarction and ischaemic stroke in young women in the RATIO study: a case-control study. The Lancet Neurology. 2009 Nov 1;8(11):998-1005.

