What Does Life Look Like After a Knee Replacement?

A modern knee replacement involves replacing the surfaces of the knee joint, not the joint itself. The tendons, ligaments and all the other structures around the knee are left in place.
I sometimes compare it to a dentist capping a tooth: We are adding new "caps" to the bones.
Knee replacement surgery usually takes an hour or two. It’s almost always done under regional anesthesia, such as an epidural block. This means that only the surgical area is numb. Many patients also like to have some sedation to help them relax and put them into a light sleep.
Most patients are able to go home within 24 hours, but after that you may have questions about what life will be like with your new knee. Here’s what I tell my patients to expect.
The sooner you start walking, the better
The team at HSS encourages patients to get up and start walking right after surgery. That’s because there will be a lot of swelling and inflammation, and moving the joint is important to prevent it from getting stiff. (Find a knee replacement surgeon at HSS to suit your specific condition, location and insurance.)
Physical therapy is key
Physical therapy after knee replacement surgery is vital. At HSS, we have a program that allows patients to do PT virtually at home. A therapist gives you exercises to do and is able to watch you do them and give you feedback via video call. HSS offered this option even before the COVID-19 pandemic, but now we’ve ramped it up and it’s great. If you prefer to meet with a physical therapist in person, you can do that.
Recovery is different for everyone
Generally, people are pretty far along by six weeks and mostly recovered by three months after surgery. Minor aches and pains may last for a while longer.
Your recovery time will vary depending on whether you have a partial or full knee replacement. You will need to walk with a cane for at least a couple of weeks. Return to work can vary, but generally expect at least a couple of weeks.
For the first four to six weeks after surgery, therapy will focus on improving your range of motion. Many people start with muscles that are atrophied, or weakened, especially if they were limiting their activities for a long time before surgery. For them, it may take longer to recover, making it important to continue an exercise program focused on building strength.
There are very few long-term limitations after knee replacement surgery
The main thing I tell my patients to avoid is long-distance running. It’s high impact and repetitive, and it puts a lot of force on your knee. Most other physical activities and sports are fine. What’s more important is that you do not do anything that makes you feel uncomfortable. Some people are bothered by kneeling because it compresses the joint and puts direct pressure on it. There’s no harm in kneeling, but if it bothers you, you should put a cushion underneath your knee, especially if you’re kneeling on a hard surface.
The main reason we put limitations on your activities is that we want your implants to last a lifetime. If you are younger – in your 40s or 50s, for example – it’s more important for you to follow these restrictions. We don’t have a set lifespan for these implants, but past experience has shown that the vast majority of knee implants last at least 20 to 30 years. Our goal, however, is for them to last a lifetime.
Preparation before surgery is just as vital to healing as what you do afterward
A little preparation can go a long way. At HSS, we take many steps before and after surgery to help our patients heal faster. For example, we offer specialized programs to help people lose weight and quit smoking before surgery, since research has shown those measures can help speed recovery. Our "prehabilitation" prehab program gives patients a chance to build strength in certain muscles around the knee prior to surgery. We also provide very personalized support for patients with sleep apnea, rheumatoid arthritis and other conditions that could have an effect on recovery.
Why you should choose HSS for knee replacement
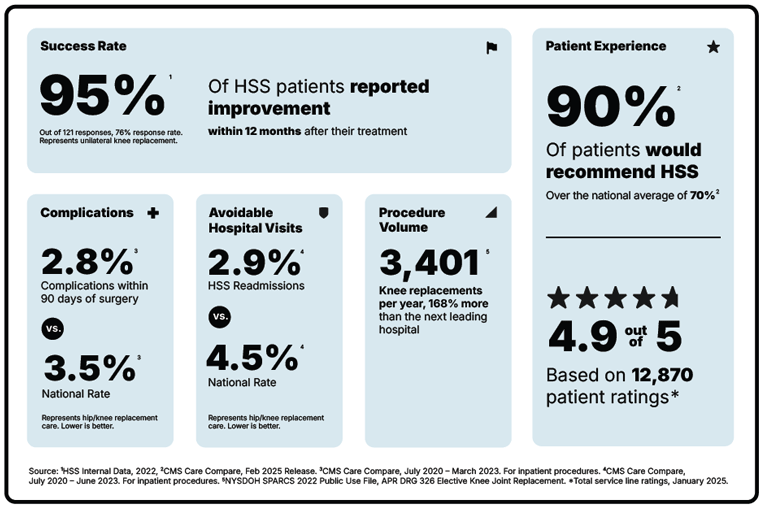
Knee replacement is a surgery focused on reducing pain and getting you back to the activities you love. But not all hospitals achieve the same results. Some are more reliable than others. With the help of the HSS Hospital Reliability Scorecard, you can make sure you're asking the critical questions to find the hospital that's right for you. Understanding the data points will help you make the best decision for your care. See hospital reliability data