Congenital Muscular Torticollis
Torticollis is a constant twist of the neck that can affect the development of a baby’s senses (especially vision) as well as motor skills.
What is torticollis?
Torticollis (Latin for "twisted neck") is a constant tilting of the head to one side with a simultaneous rotation to the opposite side. When adults have torticollis, it is sometimes referred to as “wry neck.” Congenital muscular torticollis (present at birth) is the most common type of torticollis in infants. Torticollis is the third most common congenital deformity after hip dislocation and clubfoot.
What are the symptoms of congenital torticollis?
The clearest symptom of torticollis is a constant tilt in an infant's head to one side, with the chin pointing toward the shoulder opposite that of the shoulder the head is tilted toward.
If you notice any of the following, you may wish to speak with a pediatrician, pediatric orthopedist or physical therapist about torticollis:
- Your baby prefers to turn his/her head to one side over the other.
- When looking at your baby's pictures, his/her head always seems tilted to one side.
- There is flattening on the back or side of your baby's head.
- Your baby's posture looks like the photo above.
- Your baby prefers to nurse on one side.
What causes torticollis?
The causes of torticollis are unknown, but it may arise as a result of muscular, skeletal, neurological or visual conditions. The most common form is congenital muscular torticollis. It is characterized by the shortening of the sternocleidomastoid muscle (SCM), a muscle that bends and turns the neck. Theories for the cause of congenital torticollis include a crowded position in the womb and/or decreased blood supply or trauma to the SCM. After birth, acquired torticollis may be caused by the infant spending too much time with his/her head turned in the same direction. This may cause or may be due to head flattening (a form of plagiocephaly, which is described in greater detail below).
How common is torticollis?
Torticollis is reported in about 0.4% to 2.0% of the population (about 1 in 300 live births).
How is torticollis diagnosed?
A pediatrician or pediatric orthopedist can usually diagnose torticollis by examining the child, although an ultrasound or X-ray may also be required.
Congenital muscular torticollis is observed at birth or in infancy. The infant will have a persistent head tilt to the involved side with the chin rotated toward the opposite shoulder. Clinical signs also include an infant's strong preference to look to one side, as well as flattening of the back of the baby's head.
Is torticollis serious?
The early months of a child's life are crucial for his/her development. Torticollis can impact an infant's development of vision, sensory processing, feeding, and fine and gross motor skills.
Examples may include:
- decreased head control
- limited visual tracking
- limited reaching on affected side
- preference for rolling to one side only
- delayed sitting
- asymmetrical crawling
- delayed walking
- poor balance
- difficulty feeding
- decreased tolerance to movement in space, such as swinging or sliding
If you suspect your child has this condition, it is important to seek treatment as early as possible to avoid potential developmental delay and facial asymmetry. The HSS Lerner Children's Pavilion is nationally ranked as a best children's hospital for pediatric orthopedics by U.S. News & World Report. At HSS, then the diagnosis and treatment of congenital torticollis occur at the same visit.
How do you treat torticollis?
Physical therapy and occupational therapy are the most common treatments, although surgery may be required in some resistant cases.
Physical therapy
The traditional physical therapy approach to the treatment of torticollis includes passive and active range of motion exercises, active strengthening, and a positioning program. The success rate of children treated conservatively with physical therapy is excellent, ranging between 90% to 99%. Parents participate with their baby’s treatment with a home exercise program that consists of stretches for the baby’s neck, play activities that promote symmetrical development, as well as special positioning for play, sleeping and sitting in a stroller. "Tummy time is recommended four times a day for at least 15 minutes.
Surgery
In the unlikely case of persistent congenital muscular torticollis that does not respond to a regular regimen of physical therapy, surgery may be necessary to correct the condition. Under general anesthesia, the pediatric orthopedist will lengthen the tight muscle. Physical therapy will resume after surgery.
Secondary issues: Plagiocephaly in torticollis
What is plagiocephaly?
The term "plagiocephaly" refers to an asymmetric appearance of an infant's head. Plagiocephaly is seen commonly with torticollis, because infants tend to keep their heads turned to one side. Other associated facial asymmetries may include uneven eyes and ears and a fuller cheek on one side.
Plagiocephaly may present in several ways. True plagiocephaly is an oblique flattening of one side of the baby's head with a protruding forehead on one side. Other craniofacial asymmetries include brachycephaly, where the entire back of the head is flat, and scaphocephaly, where the head shape is long and narrow with flattening on both sides. A child can also have a combination of more than one craniofacial asymmetry.

Flattening at top of the head shown by white arrow
Although plagiocephaly is common among infants with torticollis, patients with the condition are referred to a neurosurgeon to rule out craniosynostosis, a separate condition that can cause plagiocephaly.
What causes plagiocephaly?
Positional plagiocephaly is caused by prolonged and asymmetric pressure on the head. This may happen because of intrauterine positioning (in the womb), prolonged time in any reclined positioner or carrier, decreased tolerance for tummy time, or torticollis.
How is plagiocephaly diagnosed?
Diagnosis of plagiocephaly or other cranial asymmetries is based on clinical observation by the child's healthcare professional. A visit to a specialist, such as a craniofacial specialist or neurosurgeon, may be recommended to rule out other diagnoses.
What is the treatment for plagiocephaly?
Treatment for plagiocephaly includes positioning and/or use of a helmet. With a positioning approach, pressure is relieved by turning the child’s head away from the flat side, using “tummy time” or other methods.
As mentioned above, encouraging tummy time throughout the day takes pressure from the back of the head. Tummy time is recommended at least 15 minutes four times per day.
Placing your baby in different positions throughout the day (on his/her side or sitting) and using different carriers, such as front carriers or slings, can also alleviate this pressure. It is still important to follow the Back to Sleep guidelines and have your baby sleep on his/her back.
Some children with plagiocephaly may benefit from wearing a special helmet. Research studies show that the helmet works faster and is more effective than positioning alone, although the decision on whether a helmet is appropriate will be made by a neurosurgeon and a physical therapist.
The helmet, which must be prescribed, is made of a lightweight plastic material by an orthotist (a healthcare professional who fabricates and/or fits braces and splints for patients). It is worn 23 hours per day. The helmet contacts the fuller side of the child’s head and does not make contact with the flatter side of the head. Therefore, as the baby grows, the head will grow more symmetrically.
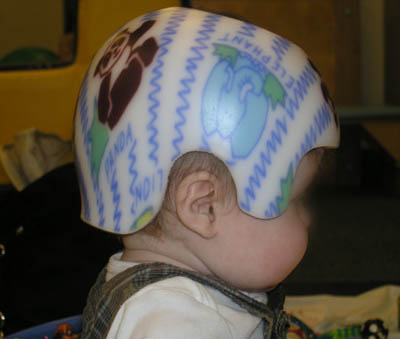
Helmet, made of a lightweight plastic, worn 23 hours per day
Helmets are most effective when started early (four to six months) when there is rapid growth of the cranium. They can be used up until 18 months of age.
If you think your child may have signs of torticollis as described here and would like to have your child seen by a pediatric orthopedist, please visit the HSS Pediatric Orthopedic Service or review a list of physicians who treat this condition. If your child has a diagnosis of torticollis and physical therapy has been recommended, please call the HSS Pediatric Rehabilitation Department at 212.606.1137 to receive an evaluation.
Updated: 9/10/2021


