An Overlap of Drug-Induced Subacute Cutaneous Lupus Erythematosus and Dermatomyositis in an 80-Year-Old Woman
From Grand Rounds from HSS: Management of Complex Cases | Volume 10, Issue 2
Case Report
An 80-year-old woman developed a pruritic rash on her scalp, prompting a dermatology evaluation after several weeks. A biopsy found interface dermatitis and prominent tissue eosinophils, perhaps consistent with a drug reaction. Her past medical history included Hashimoto’s thyroiditis, hypertension, knee osteoarthritis, collagenous colitis, mitral regurgitation requiring mitral valve replacement, atrial fibrillation for which she was taking coumadin, and a distant history of breast cancer, with no evidence of active disease. Several medications were discontinued, including diltiazem 2 months after the rash appeared, losartan–hydrochlorothiazide a month after that, followed by atorvastatin, guaifenesin, loperamide, and omeprazole.
Nonetheless, her rash progressed. She developed periorbital edema and erythema, rash of the anterior chest and lateral thighs, periungual erythema, diffuse erythema of the dorsum of her hands, and coarseness and fissuring of the skin of her lateral fingers. Hydroxychloroquine 200 mg twice daily was added 5 months after symptoms appeared, with little benefit. Given the increasingly classic presentation of the rash, she was thought to have dermatomyositis (DM). A skin biopsy taken from the thigh showed interface dermatitis with karyorrhexis, a finding consistent with subacute cutaneous lupus erythematosus (SCLE), although DM or a drug reaction could not be ruled out. Serologic testing was notable for a positive antinuclear antibody titer (1:2560) and antibodies to single-stranded DNA and thyroglobulin, but testing was otherwise negative, including for anti-Ro/SSA and anti-histone antibodies and a limited myositis panel.
A re-introduction of diltiazem several months later to treat hypertension resulted in a dramatic surge in her pruritic rash, with more diffuse erythema covering most of her body. The rash was mostly confluent in the upper body but consisted of coalescing papules and annular plaques of the lower extremities (Fig. 1). She also reported severe fatigue and subtle weakness, most noticeable as modest difficulty in climbing steps and dyspnea on exertion.
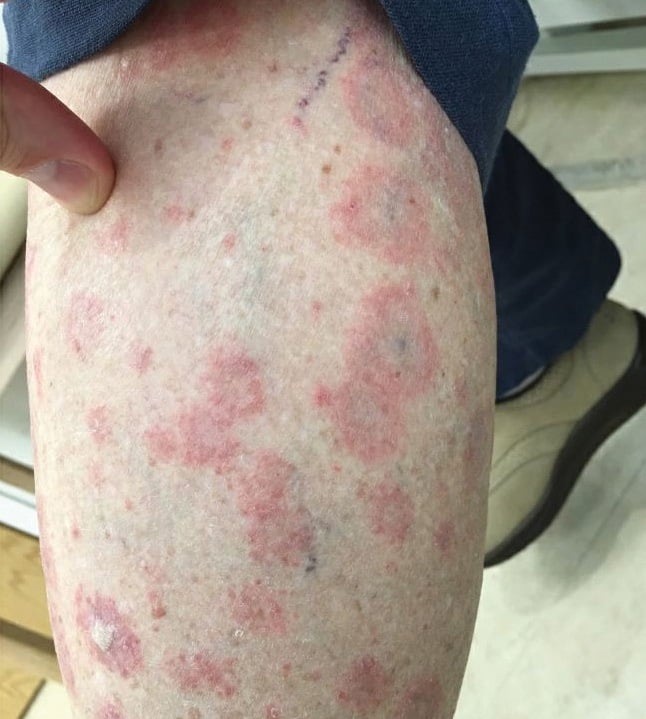
Figure 1: Annular plaques of the lower extremities.
Examination confirmed proximal muscle weakness, rash, and marked nailfold capillary changes (Fig. 2), with hyperkeratotic cuticles, extensive dropout, and enlarged capillaries. Laboratory testing revealed normal creatine kinase but elevated lactate dehydrogenase levels, lymphopenia, and mild eosinophilia.
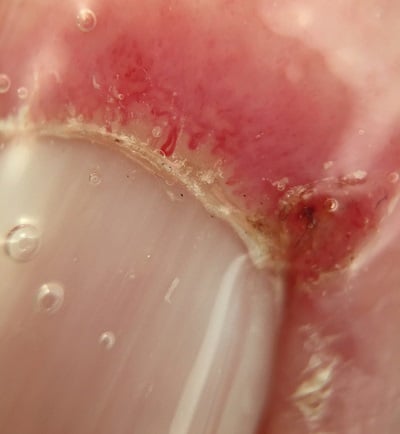
Figure 2: Nailfold changes, including hyperkeratotic cuticles, extensive dropout, and enlarged capillaries.
Based on these findings, she was diagnosed with DM and a second, distinct rash provoked by diltiazem exposure, suggestive of SCLE. She was treated with tapering prednisone, beginning at 40 mg daily, and hydroxychloroquine.
Later, the annular rash and peripheral eosinophilia faded with diltiazem discontinuation, but the DM rashes and weakness persisted. Two months later she was found to be positive for antibodies to transcription intermediary factor 1-γ, which was not part of the initial myositis assessment. This antibody can be associated with malignancy in patients with DM, but no cancer has been identified on subsequent annual screenings. Four years after her initial symptoms, the patient is still experiencing mild skin and muscle symptoms despite prednisone 5 mg daily and hydroxychloroquine. Trials of azathioprine and methotrexate were complicated by repeated infections and so were discontinued. She is also managing her symptoms through structured physical therapy.
Discussion
This case presents an interesting overlap of SCLE and DM. Drug-induced lupus is a well-characterized phenomenon, classically associated with anti-histone antibodies; management involves removing the offending agent. SCLE can be associated with medications, most commonly calcium channel blocker therapy [1].
Drug-induced DM is less well characterized but can occur in the setting of a variety of medications [2], including statins, hydroxyurea, or supplements [3], although diltiazem has not been reported as a potential cause. In this case, diltiazem may have had a role in the onset of DM and SCLE, although removing it did not resolve all clinical findings, even with the addition of hydroxychloroquine and prednisone.
This case highlights the value of nailfold capillary assessment in the diagnosis of DM [4], as some other features of the patient’s presentation were suggestive of systemic lupus erythematosus (SLE), and skin biopsy was insufficient for distinguishing between SLE and DM. Additionally, while the annular rash of the lower extremities appearing as an atypical manifestation of DM cannot be ruled out, its resolution with diltiazem cessation, along with the persistence of other DM manifestations, suggests that these were separate phenomena.
References
- Crowson AN, Magro CM. Subacute cutaneous lupus arising in the setting of calcium channel blocker therapy. Hum Pathol. 1997;28(1):67–73.
- Seidler AM, Gottlieb AB. Dermatomyositis induced by drug therapy: A review of case reports. J Am Acad Dermatol. 2008;59(5):872–880.
- Zeidi M, Chansky PB, Werth VP. Acute onset/flares of dermatomyositis following ingestion of IsaLean herbal supplement: Clinical and immunostimulatory findings. J Am Acad Dermatol. 2019;80(3):801–804.
- Cassius C, Le Buanec H, Bouaziz JD, Amode R. Biomarkers in adult dermatomyositis: tools to help the diagnosis and predict the clinical outcome. J Immunol Res. 2019;2019:9141420.

