Anterior Approach Hip Replacement: An Overview
Total hip replacement surgery is regarded as among the most valued developments in the history of orthopedics. The procedure relieves pain and restores mobility to people whose joints have been damaged by trauma or degenerative diseases such as hip arthritis. This article discusses a particular method for total hip replacement called the anterior approach.
Types of surgical approaches
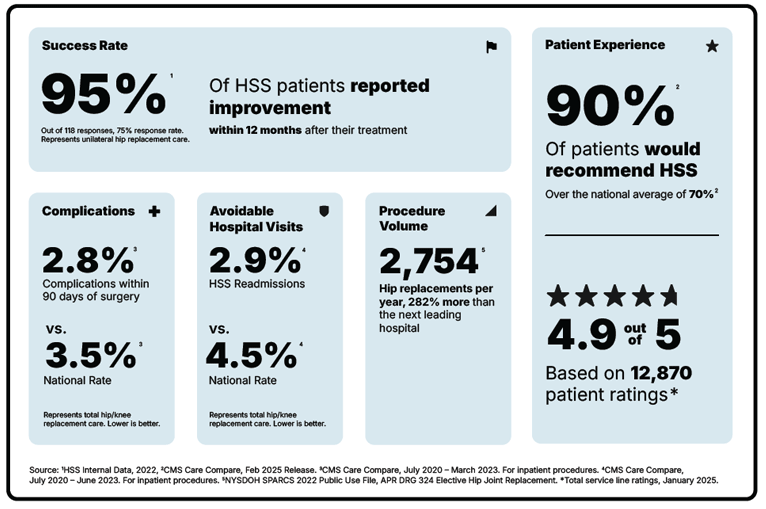
Surgeons and researchers at Hospital for Special Surgery in New York City, where more knee replacements and hip surgeries are performed than at any other hospital in the United States, continually work to improve upon the success of joint replacement surgery by developing, evaluating and refining existing and new surgical procedures and processes. As a result, today orthopedic surgeons have a range of surgical approach options. During the surgery, the hip joint can be accessed through:
- the back of the hip – the posterior approach
- the side of the hip – lateral or anterolateral approach
- the front of the leg – anterior approach
- a combination of the above approaches
The fact that there is more than one approach to perform a hip replacement means that there is no “perfect surgical approach." Each approach has advantages and disadvantages. The surgical approach is chosen carefully by your surgeon based on a number of factors, including but not limited to your anatomy, body type, medical history, the complexity of the procedure, and surgeon’s preference.
The posterior approach is the most commonly used at HSS, followed by the anterior approach.
Posterior approach
The posterior approach, the dominant surgical method for many years, is used in the majority of surgeries performed in the United States. It involves accessing the hip joint through an incision made on the side of your hip. This approach provides doctors with an excellent view of the hip structures, allowing for optimum placement of all kinds of hip implants. Over the years, doctors have refined this procedure so that it is less invasive to body tissues by reducing the size of the incisions while still maintaining safety and effectiveness. These minimally invasive hip replacement techniques – pioneered at HSS – have helped to diminish muscle trauma and reduce length of hospital stay.
Anterior approach
The direct anterior approach has been used to some degree since the 1980s and it has gained popularity in recent years. The incision is made in the front of the groin, rather than on the side (as in the posterior approach).
Who can have an anterior hip replacement?
The decision is made by the surgeon on a case-by-case basis, but certain patients are not well-suited for this procedure, and if they do undergo it, it may require longer incisions. This includes people who have:
- implants or metal hardware in the hip from prior surgery
- a very muscular or obese (BMI greater than 40) body type
- a wide pelvis
Animation: Anterior hip replacement approach
What are the advantages of anterior hip replacement?
Frontal entry makes it possible to reach the hip joint by separating muscles, rather than splitting them. In the appropriately selected patient, the anterior hip replacement is likely associated with less postoperative pain, especially in the first two to four weeks. Afterwards, there are no recovery differences between the anterior and posterior approaches.
Leg length and implant position are also able to be measured with the anterior approach.
- Due to the different nature of the approach, there are different precautions to follow postoperatively to prevent a hip dislocation.
- The reoperation rates (the possibility of requiring a revision surgery) for both approaches are similar. The incidences of a hip dislocation in some patients may be higher in the posterior approach.
- Deep infection rates are similar for both approaches.
What are the disadvantages and risks of anterior hip replacement?
Disadvantages to the anterior approach are both practical and medical.
- For medical experts, a special operating table or specialized retractors and specific tools may be required, but this is also true of other approaches.
- It has a longer surgical time.
- There is a potential for radiation exposure.
- Patients also run a slightly higher risk of experiencing femoral and ankle fractures especially when using the HANA table.
- There is a risk of a numb, tingling or burning sensation along the thigh, referred to as lateral femoral-cutaneous nerve damage which may be temporary or permanent.
- Superficial wound issues are slightly more common in the anterior approach especially in obese patient
Is anterior hip replacement painful?
All surgery has some pain associated with it but, fortunately, the anterior approach tends to be less painful than some of the other hip approaches.
What is the recovery time for anterior hip replacement?
Most patients are walking with a cane the day of surgery or by the next day. This allows rapid progress and more independence for the patient − often allowing the patient to go home the day of surgery or the next morning. Cane use is generally two to three weeks and activities progress accordingly with return to active sport by three months.
Physical therapy is done in person or remotely, but in some cases is not needed at all. By about the three-month mark anterior and posterior approach patients are functioning equally well and the long term results and longevity are similar.
How successful are anterior hip replacements?
It is important to note that the results of total hip arthroplasty are outstanding in terms of relief of pain and improvement in function. There has been, to date, no clinical study demonstrating the superiority of one surgical approach over another. The possible short-term benefits of one surgical approach over another must always be balanced with the possible untoward side effects unique to that approach.
Anterior hip precautions
Recently, improvements in surgical technique, instrumentation, and patient selection have made the anterior hip replacement a viable option for patients considering total hip replacement. Currently, if performed by an experienced surgeon on the properly selected patient, an anterior hip replacement can result in a rapid recovery during the weeks after surgery. The selection of the appropriate patient for anterior arthroplasty is crucial to the overall success of the surgery and your surgeon will discuss which surgical approach is best for your individual condition.
Why you should choose HSS for hip replacement
Hip replacement is a surgery focused on reducing pain and getting you back to the activities you love. But not all hospitals achieve the same results. Some are more reliable than others. With the help of the HSS Hospital Reliability Scorecard, you can make sure you're asking the critical questions to find the hospital that's right for you. Understanding these data points will help you make the best decision for your care: See hospital reliability data