
Advice to improve your movement, fitness, and overall health from the #1 in orthopedics in the U.S.
6 Things to Know About Recovery After Knee Replacement
Learn more about whether knee replacement might be the right choice for you.
Advice to improve your movement, fitness, and overall health from the #1 in orthopedics in the U.S.
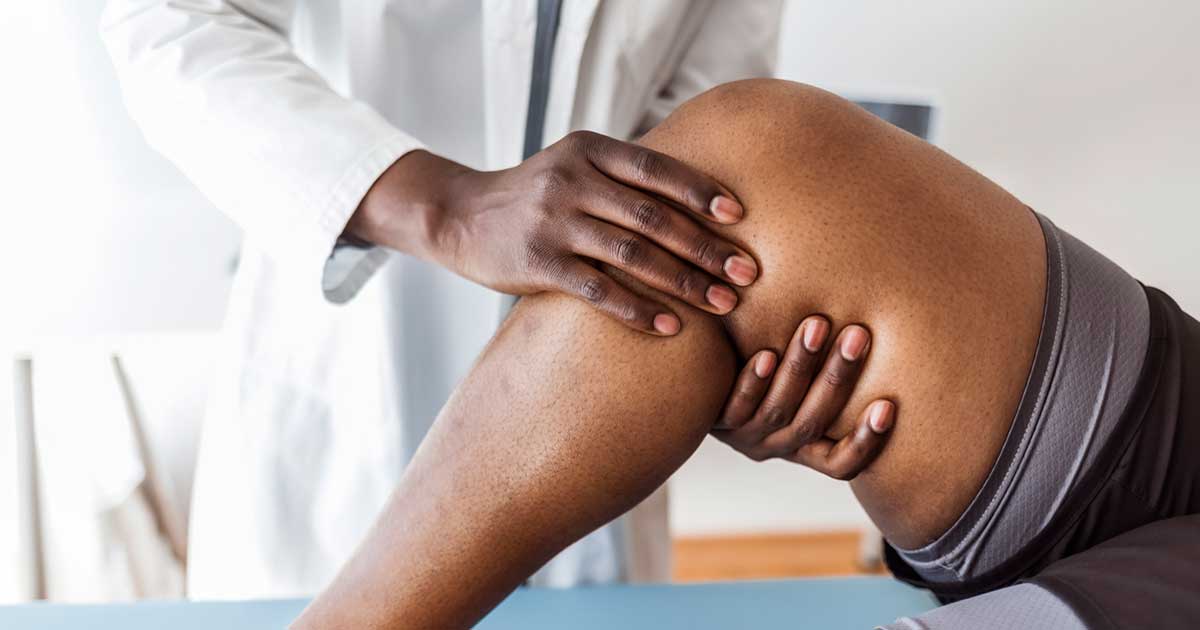
Of course, making the decision to have surgery can be difficult. (No one really enjoys the process.) But if you’re considering a knee replacement, you should know that that newer surgical procedures, including the use of less invasive techniques and surgical robots, have made knee replacement surgery much easier for patients than it used to be, says Fred David Cushner, MD, a knee replacement surgeon at HSS. These techniques result in less blood loss and a faster recovery.
Here are six things to know about recovering from knee replacement surgery.
1. Pain care begins from the moment you enter the operating room.
Knee replacement surgery at HSS is usually done with spinal anesthesia (commonly known as an epidural) rather than general anesthesia. “When you have general anesthesia, there is usually a lot of pain right when you wake up,” Dr. Cushner says. “But with spinal anesthesia, it wears off gradually, which allows us to keep up with the pain.”
When the spinal anesthesia wears off, patients may be offered nerve blocks in the area around the joint replacement. Medicines injected into the nerves above the knee can provide 24 to 36 hours of pain relief.
Many other kinds of medications also help relieve pain, including anti-inflammatories, nerve pain medications like gabapentin, and even some antidepressants. “Narcotics are part of the protocol, too, but we only give them as needed, not around the clock,” Dr. Cushner says.
Importantly, the less invasive procedures used today result in a smaller amount of tissue damage to the surgical area. This means the degree of pain most people experience after the surgery is greatly reduced.
2. After your knee replacement surgery, your care team will get you up and walking within a few hours.
One of the goals at HSS is to get patients out of bed as soon as the spinal anesthesia wears off. Depending on what time of day you have your surgery, this might be the same day or first thing the next morning.
Your physical therapists and nurses will make sure that you can safely get out of bed, transfer from your bed to a chair, and get to the bathroom. They will also ensure that you have enough range of motion in your new knee to begin walking with a walker right away. “This is important because the more you get up and use your new joint, the faster you will recover,” Dr. Cushner says.
Some patients are able to go home the same day, but the majority of patients spend one night in the hospital. “Occasionally someone needs to stay a little longer,” Dr. Cushner says, “especially if they live in a walk-up or don’t have a lot of family support. But we know that patients do very well recovering at home.”
3. Physical therapy is an important part of recovery after knee replacement surgery.
Physical therapy starts from the first time you get out of bed. Each stage of therapy has a different goal. While you are still in the hospital, your physical therapist will check your range of motion, or how much you can bend and straighten your leg. This includes working to keep your leg at full extension, while at the same time making sure that it’s not overextended when propped up.
After you leave the hospital, an HSS physical therapist will come to your home for the first few weeks. They will work on maintaining the range of motion in your knee and helping you to rebuild strength in the surrounding muscles. Eventually, you will transition to getting physical therapy at a clinic or other facility.
During the early months of the COVID-19 pandemic, HSS offered virtual physical therapy to many patients. That type of therapy is still an option for those who prefer it.
How long you continue physical therapy after surgery is based partly on your course of recovery and partly on your preferences. “Some people stop at six to eight weeks,” Dr. Cushner says. “Others may continue for three to four months, especially if they like doing their therapy under the supervision of a specialist.”
4. Most people are able to walk without a walker or cane about six weeks after knee replacement surgery.
Recovery is different for everyone. It’s based on several factors, including whether you have one or both knees replaced, the condition of your other joints, and your overall health and fitness level before the operation.
Generally, though, most patients use a walker for the first three weeks, and then transition to using a cane for another two to three weeks.
5. You can return to a fully active lifestyle after knee replacement surgery.
“It’s a gradual recovery, and everyone is different, but the bottom line is that people do return to big, active lifestyles after knee replacement surgery,” Dr. Cushner notes.
Most people begin to increase their activity levels as soon as they stop using a cane. Regularly taking longer walks is an important part of physical therapy and recovery. Within two to three months, most people can return to activities like riding a bike or playing golf. Eventually, patients are able to go back to more strenuous activities like skiing and playing tennis. “It’s all obtainable,” Dr. Cushner says. “There are no limitations.”
As for wound healing, thanks to less invasive procedures, incisions are usually only four or five inches long. Most HSS surgeons close surgical incisions using plastic surgery techniques. “This helps the wounds heal better and also looks nice aesthetically,” Dr. Cushner says.
6. Where you have your knee replacement matters for your recovery.
“Studies have shown that the number of procedures a hospital does in joint replacement every year matters — and we are the leaders,” Dr. Cushner says. “Patients who come here get the complete package: not only the best surgical treatment but also state-of-the-art anesthesia, nursing care, and physical therapy.”
Infection rates after joint replacement surgery are also extremely low for patients treated at HSS; only 0.5%. Infections are a serious complication that may require additional surgery.
“We’re always evolving, whether in the design of the implants, the surgical techniques, or the use of special instruments and robotics,” Dr. Cushner says.
Published 10/24/2022



