The Ponseti Method for Clubfoot Correction: An Overview for Parents
The Ponseti method has become the most widely practiced technique for early treatment of infants born with clubfoot.
If a child's physician meticulously follows the details of this method, applying all its elements without modification, parents of children with clubfoot can expect optimal results in the short and long term.

- What is the Ponseti method?
- Why is it called the Ponseti method?
- When should we start the Ponseti method?
- How long does the Ponseti method take?
- What are the stages of the Ponseti method?
- How does the Ponseti method work?
- How do I take care of my baby in the Ponseti cast?
- How successful is the Ponseti method?
- How often does clubfoot relapse?
What is the Ponseti method?
The Ponseti method is a systematic series of casting and orthotic bracing treatments that permanently and nonsurgically corrects clubfoot in young children.
Why is it called the Ponseti method?
This comprehensive method for treating congenital clubfoot was developed by physician Ignacio Ponseti in the 1940s.
When should we start the Ponseti method?
It is best to begin within the first few weeks of life in order to correct clubfoot without the need for major reconstructive surgery. The pliable tissues of a newborn's foot, including tendons, ligaments, joint capsules, and certain bones, will yield to gentle manipulation and casting of the feet at weekly intervals.
How long does the Ponseti method take?
The initial casting period takes about 6 to 8 weeks, followed by a period of 3 months during which the baby wears a removable orthotic 23 hours a day. After that, the child continues orthotic treatment for sleep (naps and nighttime) until 5 years of age.
What are the stages of the Ponseti method?
The corrective process utilizing the Ponseti method can be divided into 2 phases:
- The treatment phase – during which time the deformity is corrected completely.
- The maintenance phase – during which time a brace is utilized to prevent recurrence.
During each phase, attention to the details of the technique is essential to minimize the possibility of incomplete correction and recurrences.
Treatment phase
The treatment phase should begin as early as possible, optimally within the first week of life. Gentle manipulation and casting are performed on a weekly basis. Each cast holds the foot in the corrected position, allowing it to gradually reshape. Generally, 5 to 6 casts are required to fully correct the alignment of the foot and ankle. At the time of the final cast, the majority of infants (90% or higher) will require an Achilles tendon lengthening procedure.
Maintenance phase
The final cast remains in place for 3 weeks, after which the infant's foot is placed into a removable orthotic device. The orthosis is worn 23 hours per day for 3 months and then during naps and night-time until 5 years of age. Failure to use the orthosis correctly may result in recurrence of the clubfoot deformity. Good results have been demonstrated at multiple centers, and long-term results indicate that foot function is comparable with that of normal feet.
How does the Ponseti method work?
The unique manipulation and casting maneuvers used in the Ponseti method gradually correct multiple deformities associated with clubfoot, in succession. First, the high arch is flattened. Next, the inward position of the forefoot and midfoot is slowly pushed externally with several casts. The process of external placement of the fore and midfoot indirectly corrects the hindfoot and ankle. Lastly, the final stretching casts address the contracted Achilles tendon. If the Achilles tendon remains too contracted, which occurs in approximately 90% of clubfeet, the tendon is cut completely.
First cast
Prior to casting, the position of the forefoot (front of the foot) in relation to the heel creates cavus (abnormally high arch) of the foot. The first cast application addresses this issue and aligns the forefoot (front of the foot) with the hindfoot (back of the foot). In doing so, the cavus is corrected, typically after one cast.
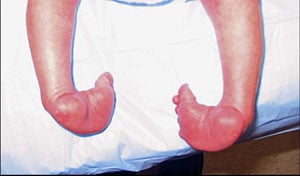
Before treatment: The marked curvature of the foot, called a cavus deformity, is characterized by a visible crease in the midfoot. The foot is tilted down due to tightness of the Achilles tendon.
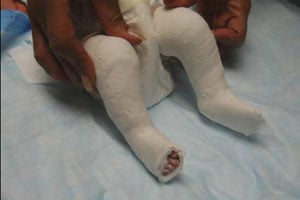
The initial Ponseti cast. Note the positioning of the forefoot to align with the heel, with the outer edge of the foot tilted even farther downward due to Achilles tendon tightness.
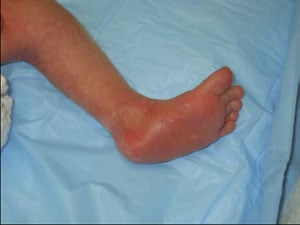
After the first cast, the foot is straight and the cavus and crease are no longer evident.
It is usually easiest to apply the cast in 2 stages: First a short-leg cast to just below the knee is placed. Once the plaster sets, the cast then extended to a long-leg cast above the knee up to the groin. Long-leg casts are essential to maintain adequate stretching of tendons and ligaments and prevent any cast slippage.
Second cast
One week later, the first cast is removed and, after a short period of manipulation, the next toe-to-groin plaster cast is applied.
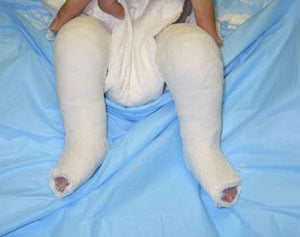
The second cast is applied with the outer edge of the foot still tilted downward and the forefoot moved slightly outward.
This phase in the manipulation and casting process is focused on straightening the foot, aligning the forefoot with the heel. Care is taken to maintain the downward tilt of the foot. Enhanced correction of this downward tilt – due to tightness of the ankle – will occur in subsequent casts. Before casting, the physician manipulates the forefoot to stretch the foot and determine what amount of correction can be maintained when the plaster cast is applied.
Unlike previous techniques, the heel is never directly manipulated in the Ponseti method. Rather, the gradual correction of the hindfoot and midfoot are such that the heel will naturally move into a correct position.
Further casting
Manipulation and casting are continued on a weekly basis for the next 2 to 3 weeks in order to gradually straighten the forefoot, allowing the forefoot to move in line with the heel. After four or five casts have been applied, normal position of the foot will begin to be observed.
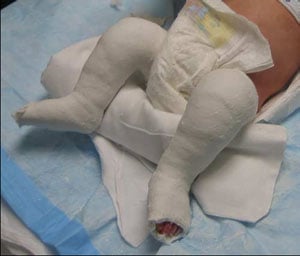
The third Ponseti cast. The Achilles tendon is stretched, bringing the outer edge of the foot into a more normal position as the forefoot is turned further outward.
When it is time to prepare final cast, most infants will require a procedure to gain adequate length of their Achilles tendon. The Achilles tendon is the cord behind the ankle that allows the ankle to move up and down. In children with clubfoot, this tendon is shortened, which prevents the ankle from bending up properly. In most of these children, the tendon must be lengthened to allow sufficient ankle motion. Prior to the application of the last cast, this is accomplished with a percutaneous surgical release (transection) of the tendon. This allows the ankle to be positioned at a right angle with the leg.
The percutaneous release is a quick, sterile procedure that is typically done through a small puncture through the skin (percutaneous), under local anesthesia. The tendon takes 3 weeks to heal in the newly lengthened position, therefore, the final cast is worn for 3 weeks.
The final cast
The foot and ankle are then casted in the final, corrected position. When the final cast is applied, the Achilles tendon is stretched farther with the forefeet pointed upward. This cast is typically applied in 2 stages, with the short-leg component extended up to the groin once the lower component has hardened.
A total of five or six casts are typically needed to correct the foot and ankle. More are needed in the most severe cases of clubfoot.

The final cast with Achilles tendon stretched farther and forefeet pointed upward.
Maintenance and prevention of clubfoot recurrence
Upon removal of the final cast, the infant is placed into foot abduction orthosis (FAO) also known as a Ponseti brace.
The FAO consists of Ponseti shoes (also called Ponseti boots) mounted to a bar. This maintains the feet in a corrected position, with the forefeet set apart and pointed upward.

Ponseti shoes mounted to the abduction bar.
The brace is worn 23 hours per day for the first 3 months following casting. The child will then continue to wear it at night while sleeping until 5 years old. Multiple studies have demonstrated the high risk for recurrence of clubfoot if the brace is not worn according to these guidelines. It is not known why. Regardless of the cause, recurrence of clubfoot appears to be close to zero when the bracing regimen is followed stringently.
How do I take care of my baby in the Ponseti cast?
While undergoing cast treatment, babies will need to be sponge bathed, as the casts are not waterproof. We place moleskin at the top of the cast, near the groin. This provides softness at the at the interface of the cast edge and thigh which mitigates skin irritation. Additionally, the moleskin can be replaced if there is a leaky diaper. Though the casts are a bit bulky, there is no difficulty putting a baby in an infant car seat, stroller, or carrier.
How successful is the Ponseti method?
Once cast treatment is complete, if the foot abduction orthosis fits properly and is worn diligently, the Ponseti method is successful in about 90% of cases.
How often does clubfoot relapse?
The risk of clubfoot recurrence persists for several years after the casting is completed, most notably if the foot abduction orthosis is not consistently used after casting. Early recurrences are best treated with several long-leg plaster casts applied at 2-week intervals. The first cast may require correction of recurrent foot deformity, with subsequent casts to correct ankle tightness.
A second Achilles tendon lengthening surgery may be necessary if there is insufficient correction at the ankle, and a tendon transfer (of the tibialis anterior tendon) may be performed in older children to help maintain the correction. Following this additional surgery, the child is then placed in a cast for four weeks with the foot in neutral position.
References
- López-Carrero E, Castillo-López JM, Medina-Alcantara M, Domínguez-Maldonado G, Garcia-Paya I, Jiménez-Cebrián AM. Effectiveness of the Ponseti Method in the Treatment of Clubfoot: A Systematic Review. Int J Environ Res Public Health. 2023 Feb 20;20(4):3714. Doi: 10.3390/ijerph20043714. PMID: 36834410; PMCID: PMC9965124.
- Scher DM. The Ponseti method for treatment of congenital club foot. Curr Opin Pediatr. 2006 Feb;18(1):22-5. doi: 10.1097/01.mop.0000192520.48411.fa. PMID: 16470157.
- Yau A, Doyle SM. Clubfoot for the primary care physician: frequently asked questions. Curr Opin Pediatr. 2020 Feb;32(1):100-106. doi: 10.1097/MOP.0000000000000860. PMID: 31815780.




