Patellofemoral Instability
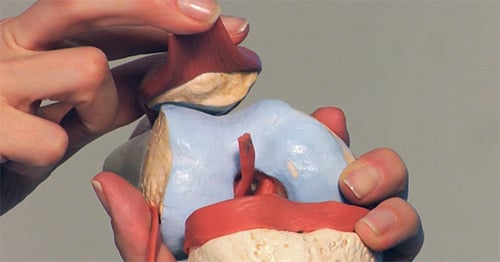
What is patellofemoral or patellar (kneecap) instability?
Patients who have a tracking problem in the patellofemoral joint, where the patella (kneecap) does not stay in the groove on the femur, are vulnerable to a spectrum of knee conditions. These include:
- Subluxations: in which the patella slips partially but not completely comes out of the trochlea. These partial dislocations can result in pain, swelling, a popping or cracking sensation or stiffness.
- Dislocations: a traumatic injury in which soft tissues are damaged as the patella completely “jumps” the track and then comes forcibly back into place. Because the bone always dislocates outward, the ligament on the inside – the medial patellofemoral ligament (MPFL) – tears or stretches.
Some patients who experience kneecap instability also have a malformation of the femur and tibia which places excessive stress on the medial patellofemoral ligament (MPFL). This condition, known as complex patellofemoral instability usually requires an interdisciplinary medical approach to treat.
What are the signs and symptoms of patellofemoral instability?
Physical signs of dislocation include significant swelling of the knee and an “apprehension sign," an anxious response to the orthopedic specialist guiding the patella outward and attempting to mimic the dislocation. An MRI after a kneecap dislocation reveals both damage to the ligament, bruises on the bone inside of the patella and on the outside of the femur that occur when the kneecap “re-locates” back in place. The MRI is also helpful in evaluating the knee for evidence of cartilage injury which is very common after dislocations.
What causes patellar instability?
People who experience a first-time patella dislocation frequently do so while participating in sports, causing the knee to suddenly buckle and they fall. Because ACL tears often happen in the same way, and because they are much more common than patella dislocations, it is important to rule out an ACL tear. In rare cases a patient comes in with an ACL tear and is found to have had a patella dislocation as well.
Who is at risk for kneecap dislocation and subluxation?
People at risk for dislocation and subluxation include both young women who are loose jointed, as well as female athletes who may experience a more traumatic dislocation while playing their sport. Subluxation and dislocations do occur in men and boys but much less frequently. Individuals in these groups share common risk factors, including
- a shallow (or even absent) groove on the trochlea or femur
- an abnormal insertion of the patellar tendon on the tibia (shin)
- knock knees
- high riding kneecap
In the case of a shallow groove (track), the patella is not as well-controlled as it is by the deep groove that is present in a normal patellofemoral joint. As a result, less energy is required to force the patella from its track.
Patients with malalignment that results from a knock kneed posture are subject to a greater than normal force on the patella, which pulls the bone outward, out of the trochlear groove, and toward the outside of the knee. In a normal knee, the tendon that connects the patella to the tibia maintains a force that is in line with the patella, (tracking in alignment with the trochlear groove). Orthopedists use an index called the TT-TG (tibial tuberosity trochlear groove) to measure the degree of malalignment present and guide treatment recommendations.
Individuals with patella alta, a patella or kneecap that is located higher up on the femur than normal are also at increased risk of dislocation, as the patella must travel a greater distance during flexion of the knee before engaging fully in the groove or track of the femur. The joint is particularly vulnerable to instability during this period.
Although dislocation is very painful, after the knee quiets down and returns to baseline, there may be little to no pain in between the instability episodes. Pain and instability don’t always go hand-in-hand. This can be problematic since patients who are pain-free may delay seeking treatment despite recurrent episodes of instability while cartilage damage continues to progress with each dislocation or subluxation.
What are treatments for kneecap instability?
The standard of care for first-time dislocations is non-operative treatment, where the torn ligaments can heal on their own. However, an MRI is important to evaluate the degree of damage that has occurred even after one dislocation. Surgery is necessary if a piece of bone or a piece of cartilage is a loose body (free floating in the knee) - as these can cause locking, buckling, or additional pain in the knee if left untreated. This type of injury may also be referred to as an osteochondral fracture. In these patients, surgery is performed to both remove the loose body or repair it and stabilize the patella at the same time.
Nonsurgical Treatments
In patients who do not require surgery, the knee is commonly immobilized in a splint or brace for a few days to weeks to allow the knee to calm down and for swelling and pain to subside. The orthopedist may also drain fluid from the knee to reduce discomfort at the first office visit if there is considerable swelling. Physical therapy is the primary course of treatment after a first time dislocation and is started within the first 1-2 weeks after the dislocation, to achieve normal range of motion and strength. Physical therapy after a dislocation usually continues for between 2-3 months and it can take as long as 4 -5 months for some athletes to return to their pre-injury level of play.
Once a patient has dislocated his or her patella or knee cap, he or she is at an increased risk of it happening again whether it is in the form of subluxation or a full dislocation. Although injured ligaments do “fill in” and heal during recovery, these structures are generally stretched from the injury and are less able to control the patella - further contributing to the risk of another instability episode.
Statistics show that this risk of having another dislocation or subluxation after a first time dislocation is somewhere between 20-40%; and that after the second dislocation the risk of recurrence goes up to greater than 50%. Younger patients (under the age of 25) are at even greater risk, especially those in whom the growth plates (a site at the ends of the bone where new tissue is produced and bone growth continues until skeletal maturity) are still open with redislocation rates reaching 70%.
When do you need surgery for kneecap instability?
Surgery to stabilize the kneecap is recommended for individuals who have experienced more than one dislocation. Stabilizing the knee will not only help the patient get back to sports or daily activities, but will also protect the cartilage underneath the kneecap in order to prevent arthritis from developing in these generally young patients.. Cartilage damage can occur with every instability event and statistics show that some damage is apparent on MRI in more than 70% of cases.
Depending on the underlying risk factors for instability, the orthopedic surgeon may perform either a soft tissue or a bony procedure. Soft tissue procedures involve either repair - or more frequently reconstruction - of the torn medial patellofemoral ligament (MPFL).
Repair of the ligament may be possible if the patient seeks treatment promptly and has not experienced any previous dislocations. But in most cases, the orthopedic surgeon takes tissue from elsewhere (usually a hamstring tendon) either from a donor or from the patient’s own body and constructs a new ligament.
Bony procedures or realignment surgery is advised when the patient has an anatomical abnormality in which the patella tendon attaches to the tibia in such a way that there is a severe pull on the patella sideways or laterally. In order to correct the alignment, the orthopedic surgeon moves a small portion of bone where the tendon attaches and repositions it to a location on the tibia that eliminates the lateral stress and allows the tendon to guide the patella effectively into the groove. This surgery is called an osteotomy or a tibial tubercle transfer.
Osteotomy also helps to compensate for the risk associated with a high patella (patella alta). By repositioning the tendon to a more optimal placement, the surgeon can “lower” the patella to the proper level, thus bringing the patella closer to the upper trochlear groove, reducing the distance it has to travel to enter the groove. This minimizes the risk of patellofemoral subluxation or dislocation at the early stages of flexion.
This type of surgery produces good results but is not a procedure that can be performed in young people with open growth plates. For these patients, the surgeon may choose to brace the patient until the growth plates close or if they feel the patient to be at significant risk for repeated dislocations then they may choose to do the soft tissue operation to reduce the risk and then wait until the growth plates close to do the tibial tubercle transfer (bony surgery). In some patients, both a soft tissue and a bony procedure may be appropriate. Both surgeries yield very reliable results in stabilizing the knee with an 85-90% success rate, Dr. Shubin Stein notes.
Patients with patellar instability due to mal-alignment usually have problems in both knees, whether they have dislocated both joints or not. If the patient has experienced a dislocation in both knees, the orthopedist will address the knee that is more severely affected first, and then stabilize the other one later in order to prevent cartilage damage.
What is the recovery like for kneecap surgery?
Recovery from knee stabilization surgery takes from 6 to 9 months, and involves both extensive physical therapy and activity modification.
In patients who have damaged or lost some cartilage as a result of one or more instability events, the orthopedic surgeon may recommend a procedure to repair or regenerate the damaged cartilage that lines the joint. While no method works perfectly, patients with cartilage defects resulting from instability are actually more likely to benefit from current cartilage repair techniques than patients with generalized osteoarthritis of the knee.
In a traumatic event like a dislocation, if cartilage damage occurs, it usually means that an isolated chunk or piece of cartilage has come off and that the rest has remained pristine. Filling in this defect with either cartilage from another part of the patients’ knee or from donor tissue can be an effective treatment option.
The comparatively predictable good results of knee stabilization procedures, are just one reason orthopedic surgeons emphasize the importance of stabilizing the knee before cartilage damage occurs or progresses. However, research in cartilage regeneration continues to be active and is showing promising results.


