Hip Resurfacing

Hip resurfacing, also called surface replacement, is an alternative to total hip replacement that is appropriate for some patients. This operation preserves more of your natural bone than does a total hip replacement. The hip joint can be thought of as a ball and socket joint between which lies a lubricating and protective layer known as cartilage. When cartilage loss occurs (a condition known as arthritis), the patient experiences pain as well as a loss of mobility and function. At that time, a hip replacement may be recommended.
A traditional total hip replacement involves the removal and replacement of the following with artificial implants:
- arthritic cartilage
- the acetabulum (hip socket)
- the head of the femur (thighbone), known as the femoral head
By contrast, hip resurfacing retains more of a person's natural bone.
What is hip resurfacing?
In a hip resurfacing procedure, a person's natural femoral head is retained. It may be appropriate for you to have hip resurfacing if you are an active person under the age of 60. Hip surface replacement has advantages and disadvantages, depending on each individual patient.
Hip resurfacing animation
Total hip replacement versus surface replacement
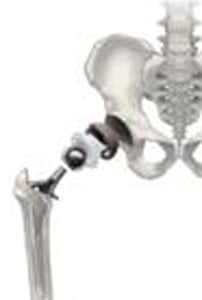
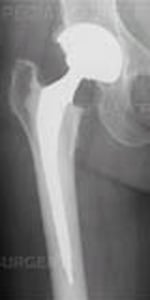
With both traditional hip replacement and surface replacement, the socket is inserted in a similar fashion. The two procedures differ in the way the femur is prepared. Whereas traditional hip replacement involves removing the head and neck of the femur, surface replacement preserves this bone. With a traditional hip replacement, after this bone is removed, a prosthetic ball attached with a stem is inserted within the thigh bone. With a surface replacement, the preserved bone is sculpted to accept a metal cap with a short stem.
Traditional total hip replacement
Hip resurfacing
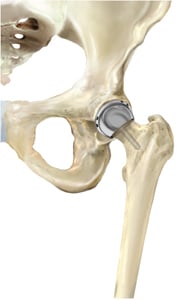
Image Courtesy of Smith and Nephew
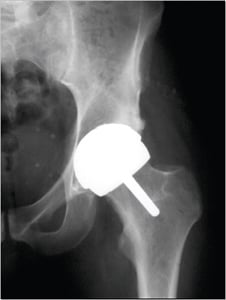
Image Courtesy of Smith and Nephew
Why should I have my hip resurfaced?
Having a hip resurfaced is a personal decision that must take into account the risks and benefits of the procedure. Most patients will elect to have a hip resurfacing procedure when they can no longer bear the pain associated with their arthritis. Others will decide to have the surgery when they feel that their hip arthritis is preventing them from participating in activities that they enjoy.
What are the advantages of hip resurfacing?
While every orthopaedic treatment has both risks and benefits, there are two specific advantages unique to surface replacement. The first is the preservation of more natural bone. The second is that resurfacing involves a larger diameter ball than a traditional hip replacement. This affords greater hip joint stability and a lower likelihood of dislocating your hip later on.
For younger patients who may outlive their implant, the preservation of bone is the largest advantage. Since bone is preserved at the initial operation, more bone is available for a future operation, should one be needed. Over time, any hip implant may loosen or show signs of wear. In a young, active population, there is a high likelihood that more than one hip replacement operation may be necessary over their lifetime. The more bone that remains after the first operation, the greater the chances of a good outcome if a hip revision (a second operation) is required years later. The preservation of more bone also facilitates the use of a much larger ball size, which creates greater stability of the hip joint. The rate of hip dislocations after a surface replacement has been shown in some studies to be about 10 times lower than for a traditional hip replacement.
What are the disadvantages of hip resurfacing?
Due to the unique nature of surface replacements and methods employed to perform the surgery, there are some risks which are either limited to surface replacements or occur at a somewhat greater frequency. These include:
Metal ion dispersal
The current generation of surface replacements are metal-on-metal bearings. That means both the ball and the socket are made entirely of metal. Although this cuts down dramatically on the wear and tear of the components, it has been shown to cause metal ions to be dispersed through the body. Cobalt and chromium ions are measurable in the blood stream, but have not been shown to cause cancer or any other disease in humans. Although the metal ions are measurable, no one knows what the "safe levels" are, as studies have been inconclusive. Generally speaking, people with functioning kidneys are able to excrete the ions through their urine. Metal-on-metal hip replacement implants have been around since the 1970s, and these have never been linked to an increase in cancer or other diseases. But, we still do not know for certain the “safe levels” of these metal ions in the blood. For this reason, it is not advisable to perform metal-on-metal hip resurfacing in patients who are on dialysis, have kidney transplants or renal failure.
Femur fracture
Because the bone of the femur is retained, it is possible to fracture it after surface replacement. Most of the fractures occur early in the post-operative period if too much weight is put on the leg too early. The body needs time to adapt to the new prosthesis. Post-operatively, crutches are used for 3-4 weeks to protect the amount of weight put on the leg. With current techniques and rehabilitation protocol, the risk of fracture is less than 2%.
Nerve injury
While not limited to surface replacement, working around the bone of the femur may cause extra pressure to be put on the nerves in the hip area. This may cause a transient weakness of some of the muscles of the leg in less than 1% of cases.
Heterotopic ossification
Surface replacement may require a somewhat larger incision and exposure than that of total hip arthroplasty. As such, the hip resurfacing procedure may lead to extra bone forming around the hip, leading to stiffness, called heterotopic ossification. We take measures to prevent this, using either an anti-inflammatory medication or one dose of radiation to the hip area after surgery. The radiation treatment, known as XRT (external radiation therapy), is performed in the first 2 days after surgery and does not have any association with cancer. With preventative measures, the risk of extra bone forming is less than 2%.
Allergy to the metals
A very small percentage of patients (less than 1%) have been found to develop an allergy to the metals used in hip resurfacing. Unfortunately, there is no available test to determine this before surgery. Since all hip resurfacings are currently made of the same metals, there is a possibility of an allergic response to all resurfacing implants. If a patient develops an allergy to the metals used in hip resurfacing, he/she may have pain and swelling around the hip joint. Treatment may require the removal of the implant and revision surgery to a non-metal-on-metal hip replacement.
Unknowns in surface replacements
Activity resumption
At this time, it is not clear what limitations of activity patients with surface replacements should adhere to. With traditional bearing surfaces such as polyethylene or ceramics, repetitive impact has been associated with accelerated wear and even potential catastrophic breakage. Whether this will occur with the current metal-on-metal bearings such as those used in surface replacements is not known.
Longevity of Implant
The short term results (4-6 year follow-up) of hip resurfacing are encouraging. However, the early failures of hip resurfacing appear to be greater than for total hip replacement (2.2% vs 1.9%), with the majority of the early failures due to femoral neck fracture. Whether the newer forms of hip resurfacing will be successful long term is unknown. We are carefully tracking the results of hip resurfacing in our hip replacement outcome study: "Prospective Evaluation of the Clinical and Economic Outcomes of Total Joint Replacement: The HSS Hip Arthroplasty Cohort." We will be reporting our results at significant intervals of follow-up. However, it may require 10 years or longer to determine whether this newer form of hip resurfacing is as good as total hip replacement at comparable time intervals.
Recommendation
Improvements in hip implant design as well as materials are frequent in joint replacement. Extensive prospective clinical trials over many years are necessary to determine the long term outcome and the true benefits and risks of new innovations. Should you be a candidate for hip replacement, a discussion regarding your options for treatment with your physician is recommended. Only your surgeon can advise you on the option best suited for your unique circumstances and, if necessary, which procedure is best for you.
Who should have hip resurfacing vs. a total hip replacement?
Hip resurfacing and hip replacement are both designed to improve your activity, function, and decrease your pain. The difference lies in the way this is accomplished. For some patients, there is a large difference between a hip resurfacing and a hip replacement because of your age and activity level. For others, there is not such a large difference. For example, a young patient who may outlive their first hip replacement may be more willing to have a hip resurfacing because of the preservation of bone. A patient who would like to return to impact activities or activities requiring a high range of motion may have a greater benefit from a hip resurfacing. On the other hand, a patient for whom a total hip replacement can last the rest of their life would be a better candidate for a traditional total hip replacement.
What are the specific risks of hip resurfacing?
The general risks of hip resurfacing are the same as with traditional total hip replacement. These include infection, dislocation, blood clots, nerve injury, and extra bone formation around the hip that could make the hip stiff. The risk of infection with hip resurfacing is no different than with total hip replacement. The risk of dislocation is 10x lower, because of the larger diameter ball. The risk of nerve injury and extra bone formation around the hip are slightly higher with a hip resurfacing because of the need to work around your bone in an enclosed space.
A risk unique to hip resurfacing that is not present in traditional hip replacement is that of femoral neck fracture. The femoral neck is a vulnerable area of bone that connects the ball of your hip joint to the rest of your thighbone. When elderly people fall and “break their hip”, this is the area that breaks. With a traditional hip replacement is done, this bone is removed, so it cannot break. With a hip resurfacing, the femoral neck is preserved, so there is a risk of fracture. We believe the risk of fracture in this area is between 1-2%. It is because the surgical exposure, preparation of bone, and placement of the component with cement may cause this bone to be more vulnerable.
The risk of femoral neck fracture is why crutches are necessary for 4 weeks post-operative and impact activities are not recommended for 6 months. If you have a femoral neck fracture after hip resurfacing, you will need another operation to convert it to a traditional total hip replacement.
What will happen when the hip resurfacing wears out?
When a hip resurfacing wears out, it is generally because the femoral cap loosens from the underlying bone. If this happens, it can be converted to a traditional total hip replacement with a stem in the thigh bone, utilizing a big metal ball to match your socket. Generally, the socket is firmly attached to your bone and will not need to be revised. The end result is a metal-on-metal hip replacement with a big metal ball.
In the news
- Inside the surgery that changed Patrick Kane’s career and the rehab that changed more
- Hip Resurfacing vs. Total Arthroplasty: New Data
- MRI tracks soft-tissue complications after hip replacement
- Isaiah Thomas ready to contribute to an NBA roster after undergoing a hip procedure five months ago
- WWE Undertaker documentary: Review of second episode, ‘The Redemption’
Hip Resurfacing Success Stories
Medically reviewed by Edwin P. Su, MD, and Douglas E. Padgett, MD on behalf of the Adult Reconstruction and Joint Replacement Service
