Recurrent Leukocytoclastic Vasculitis Following mRNA COVID-19 Vaccination in a 76-Year-Old Woman with Previously Treated Hepatitis B Virus Infection
From Grand Rounds from HSS: Management of Complex Cases | Volume 10, Issue 2
Case Report
The coronavirus disease 2019 (COVID-19) messenger RNA (mRNA) vaccines have proven largely safe and highly effective in preventing hospitalizations and deaths from infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) [1]. In early 2021 we treated a 76-year-old woman with chronic hepatitis B virus (HBV) infection who developed a recurrence of leukocytoclastic vasculitis (LCV) within days of receiving her first dose of the Pfizer-BioNTech mRNA COVID-19 vaccine.
The patient was diagnosed with HBV in 1994 when she presented with hepatocellular carcinoma. She was started on lamivudine but in 2002 developed lamivudine resistance and LCV requiring corticosteroids. Adefovir and azathioprine were added in 2004, but in 2008, after developing adefovir resistance, she was switched to tenofovir, with suppression of HBV and resolution of LCV. Corticosteroids and azathioprine were discontinued, and in 2019 her HBV viral load was undetectable.
In late 2020 the patient received her first dose of the COVID-19 mRNA vaccine; 5 days later she developed a purpuric rash on her legs (Fig. 1), and her dermatologist diagnosed LCV.
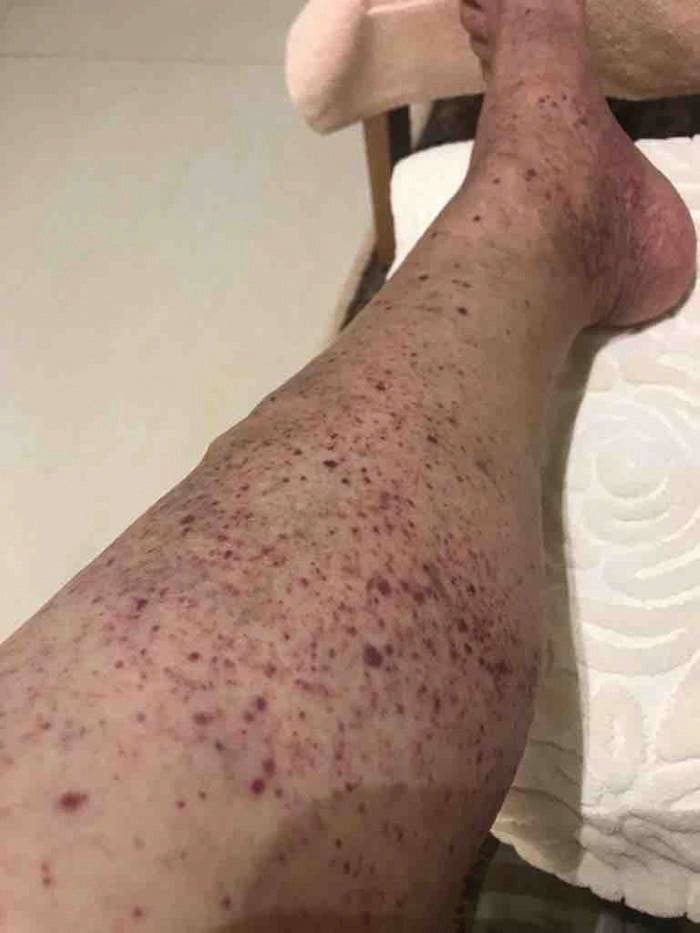
The day the rash appeared her internist instructed her to discontinue tenofovir, but it was resumed 3 days later. Laboratory test results revealed markedly elevated liver enzymes, coagulopathy, active HBV, and profound hypocomplementemia (see Table 1).
Table 1: Timeline and laboratory results, before and after first dose of the Pfizer-BioNTech mRNA COVID-19 vaccine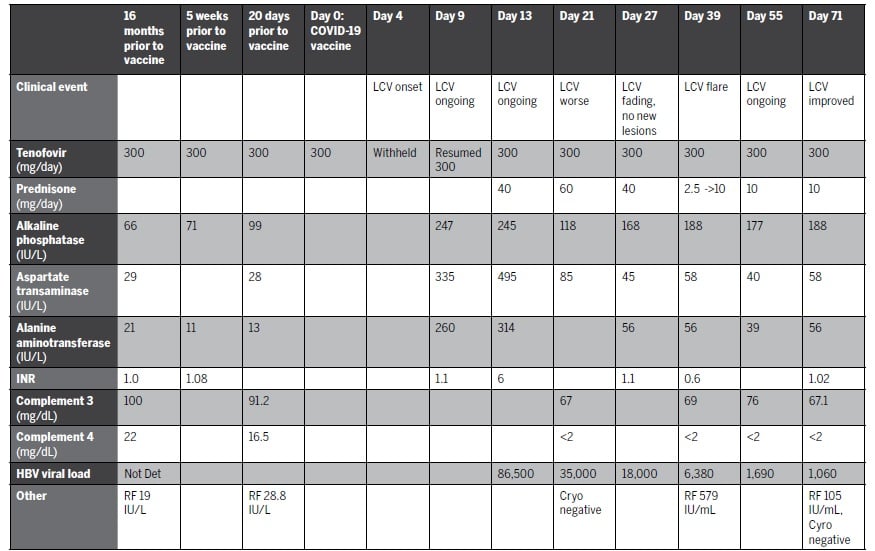
The patient improved with prednisone 40 mg, but LCV recurred when this dose was tapered. Her HBV viral load declined and LCV improved, but mild symptoms persisted several months post-vaccination.
Discussion
COVID-19 vaccination is recommended for people with autoimmune and inflammatory rheumatologic diseases, even though it may increase the risk of disease flares in some patients [2]. A few cases of LCV occuring after COVID-19 vaccination have been reported: 1 patient had psoriatic arthritis and 2 were otherwise healthy [3-5]; we believe we are the first to describe LCV recurrence along with HBV reactivation after COVID-19 vaccination.
Expert position papers from the EASL (European Association for the Study of the Liver) [6] and the AASLD (American Association for the Study of Liver Diseases) [7] note that patients with chronic liver disease are at high risk for COVID-19 sequalae and recommend COVID-19 vaccines for this population (although patients with significant liver disease were excluded from licensing trials). Some evidence suggests that patients with chronic liver disease mount a weaker vaccine response to the influenza, Streptococcus pneumoniae, and hepatitis A and B virus vaccines [6].
Our patient’s clinical picture was consistent with a reactivation of HBV infection, manifesting as LCV and compromised liver function. Her LCV had been quiescent for more than 10 years on tenofovir, and her HBV viral load was nil 15 months prior to receiving the vaccine. While we cannot establish causation, the timing of the rash suggests a possible relationship between COVID-19 mRNA vaccination and HBV recrudescence and LCV recurrence. Tenofovir was held for several days after vaccination, but it was not a likely cause of this degree of HBV reactivation.
LCV in patients with HBV can be due to either HBV-containing immune complexes or cryoglobulinemia [8]. Both mechanisms lead to complement activation and hypocomplementemia. Although the patient twice had negative cryoglobulin test results, high titer rheumatoid factor and profound hypocomplementemia could suggest cryoglobulinemia [9]. While there currently are no studies or case reports to support the hypothesis, we believe the vaccine could have led to HBV reactivation and in turn to recurrent immune-complex-mediated LCV.
This patient also experienced elevated liver enzymes and a high international normalized ratio (INR). We hypothesize several possible explanations. First, the vaccine may have caused autoimmunity directed against the SARS-CoV-2 spike protein–expressing liver cells; a study in mice showed that after mRNA vaccination there was uptake of mRNA-containing lipid nanoparticles and protein translation in the liver [10]. Second, the vaccine may have led directly to HBV reactivation and acute hepatitis through an unknown mechanism. Third, the vaccine may have induced only LCV, and the elevated liver enzymes could have developed due to stopping the tenofovir for several days.
The Pfizer-BioNTech COVID-19 vaccine phase 2/3 trial enrolled 43,448 individuals; of those in the vaccine arm, 125 had mild liver disease and 1 had moderate or severe liver disease [1]. Although the phase 1/2 trials excluded those with known HBV infection, such patients were eligible for the phase 2/3 trial if they were negative for hepatitis B e antigen (HBeAg), had persistently normal alanine aminotransferase and aspartate transaminase (ALT and AST) levels, and had a serum HBV DNA level of less than 2000 IU/mL. US Food and Drug Administration documents from the Vaccines and Related Biological Products Advisory Committee show no increase of hepatic enzymes in the vaccinated group [11]. Still, our case suggests that in patients with chronic HBV infection it may be prudent to check the HBV viral load and liver enzyme levels before COVID-19 vaccination and maintain HBV control and continue antiviral agents after vaccination.
References
- Polack FP, Thomas SJ, Kitchin N, et al.; C4591001 Clinical Trial Group. Safety and efficacy of the BNT162b2 mRNA Covid-19 Vaccine. N Engl J Med. 2020;383(27):2603–2615.
- Curtis JR, Johnson SR, Anthony DD, et al. American College of Rheumatology Guidance for COVID-19 Vaccination in Patients With Rheumatic and Musculoskeletal Diseases: Version 3. Arthritis Rheumatol. 2021 Aug 4. doi: 10.1002/art.41928.
- Cohen SR, Prussick L, Kahn JS, Gao DX, Radfar A, Rosmarin D. Leukocytoclastic vasculitis flare following the COVID-19 vaccine. Int J Dermatol. 2021 Aug;60(8):1032-1033. doi: 10.1111/ijd.15623
- Erler, A, Fiedler, J, Koch, A., Schütz, A. and Heldmann, F. A case of leukocytoclastic vasculitis after vaccination with a SARS-CoV2-vaccine – a case report. Arthritis Rheumatol. 2021. Accepted Author Manuscript. https://doi.org/10.1002/art.41910
- Bostan E, Gulseren D, Gokoz O. New-onset leukocytoclastic vasculitis after COVID-19 vaccine. Int J Dermatol. 2021 Jul 9. doi: 10.1111/ijd.15777.
- Bornberg M, Buti M, Eberhardt CS, Grossi PA, Shouval D. EASL position paper on the use of COVID-19 vaccines in patients with chronic liver diseases, hepatobiliary cancer and liver transplant recipients. J Hepatol. 2021 Apr;74(4):944–951.
- Fix OK, Blumberg EA, Chang KM, et al; AASLD COVID-19 Vaccine Working Group. AASLD Expert Panel Consensus Statement: Vaccines to Prevent COVID-19 Infection in Patients with Liver Disease. Hepatology. 2021 Feb 12:10.1002/hep.31751. doi: 10.1002/hep.31751
- Sunderkötter C, Bonsmann G, Sindrilaru A, Luger T. Management of leukocytoclastic vasculitis. J Dermatolog Treat. 2005;16(4):193–206.
- Chen KR, Carlson JA. Clinical approach to cutaneous vasculitis. Am J Clin Dermatol. 2008;9(2):71–92.
- Pardi N, Tuyishime S, Muramatsu H, et al Expression kinetics of nucleoside-modified mRNA delivered in lipid nanoparticles to mice by various routes. J Control Release. 2015;217:345–351.
- Vaccines and Related Biological Products Advisory Committee. December 10, 2020, meeting: sponsor briefing document. Silver Spring, MD: US Department of Health and Human Services, Food and Drug Administration; 2020. https://www.fda.gov/media/144246/download

