Open Repair of a Large Achilles Tendon Defect Using Quadruple Bundle Hamstring Autograft with Flexor Hallucis Longus Transfer
From Grand Rounds from HSS: Management of Complex Cases | Volume 8, Issue 2
Case Report
A 60-year-old man presented for evaluation a week after experiencing a “pop” with pain in the area of the left Achilles tendon while playing tennis. He reported a history of left Achilles tendon rupture over 30 years ago that was treated nonoperatively. The patient did well after this injury, resuming tennis until he experienced this sudden onset of pain and difficulty with plantarflexion of the left ankle. He reported a history of hypertension, osteoarthritis, and peripheral vascular disease.
On examination, the patient had pain over the musculotendinous junction of the Achilles tendon and a palpable gap in the tendon through an area of calcification from his previous rupture. The patient also had swelling, ecchymosis, and tenderness to palpation in the affected area. There was a positive result on the Thompson squeeze test. Lateral plain X-ray showed calcification at the site of the prior Achilles rupture and evidence of probable acute tendon rupture (Fig. 1).
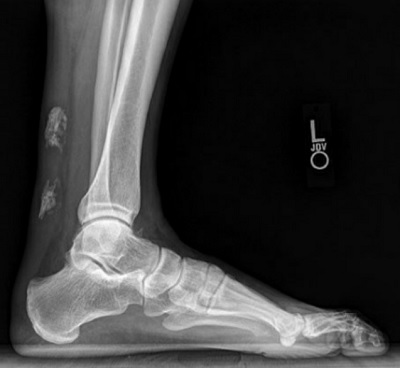
Figure 1: Lateral X-ray view of the left ankle at initial presentation demonstrating evidence of probable Achilles tendon rupture through chronic calcification at prior Achilles rupture site.
Given the large gap in the Achilles through this area of dense calcification, we determined that the patient would benefit from operative intervention. We recommended open Achilles repair with excision of the calcified tendon and harvest of the hamstring tendon for the repair, along with flexor hallucis longus (FHL) tendon transfer to the distal Achilles insertion to improve muscle recruitment [4, 5]. The patient agreed to this plan.
Intraoperatively, the patient was placed in the prone position. With the knee flexed, the hamstrings were harvested through an anterior approach to the proximal tibia at their insertion. The tendons were prepared on the back table, including the removal of residual muscle and tubularization of the graft. After we prepared the graft, we made a 7-cm incision just medial to the midline over the Achilles tendon. The ends of the tendon were mobilized. The patient had an approximately 6-cm area of tendinopathy, with a 5-6-cm area of calcified Achilles tendon. He had fractured through the calcification and had 2 cm of diastases between the calcified ends of the tendon. We then harvested the FHL tendon, taking care to open up the deep posterior compartment. After we excised the calcified portion of the tendon, we attached the hamstring tendon autograft to the base of the calcaneus. The FHL tendon was also placed in this tunnel. It was held in place using a Bio-Tenodesis Screw™ (Arthrex, Inc., Naples, FL). We then brought both limbs of the hamstring autograft proximally and performed a standard Pulvertaft-type maneuver, with approximately 10° to 15° of ankle plantarflexion [1]. The autograft was then tubularized with a suture tape (Fig. 2). We then brought the hamstring tendon back down distally and attached the new Achilles tendon reconstruction, with tension in about 10° to 15° of ankle plantarflexion. We were able to get the ankle to neutral, passive dorsiflexion. Thus, we had created a quadruple-bundle hamstring autograft to reconstruct the Achilles tendon, augmented with the FHL tendon (Fig. 2).
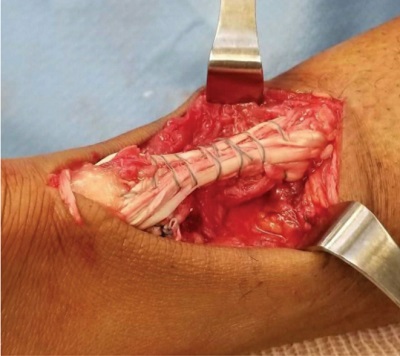
Figure 2: Intraoperative images showing hamstring autograft with Pulvertaft weave through proximal and distal Achilles stump, spanning the gap after the area of chronic calcification was excised.
Next, we placed a modified Bunnell stitch in the distal aspect of the tendon, exiting proximally and further tightening the repair [7]. At this point, we had excellent tension on our repair and negative Thompson squeeze test.
The patient adhered to the following postoperative protocol:
- Days 0–14: remain non-weight bearing in a splint with strict elevation
- Weeks 2–6: shift to non-weight bearing in a controlled ankle movement (CAM) boot with heel lift; active dorsiflexion range of motion to neutral position
- Weeks 6–12: begin formal physical therapy and partial weight bearing in a CAM boot
- Months 3–6: transition to a sneaker; return to activities of daily living; continue physical therapy
- Months 6–12: return to sports
Discussion
Large Achilles tendon defects can arise from a variety of causes and, along with chronic Achilles tendinopathy, can cause debilitating symptoms for patients and pose a difficult challenge for surgeons. The literature has noted rupture usually occurs 4–6 cm above the calcaneal insertion in a hypovascular region [2].
As this case demonstrates, hamstring autograft offers a viable surgical solution to address this difficult problem. Multiple reconstruction techniques have been described, including the use of Achilles allografts with or without attached calcaneal allograft and V-Y turndown [3, 6]. This case demonstrates the utility of using ipsilateral hamstring autograft with FHL augmentation to address large tendon defects and allow for return to pre-injury level of activity.
Posted: 7/1/2019
Authors
James Davies, MD
Orthopaedic Surgery Clinical Fellow
Hospital for Special Surgery
Medical Director, HSS Long Island, Hospital for Special Surgery
Attending Orthopedic Surgeon, Hospital for Special Surgery
References:
- Brown SH, Hentzen ER, Kwan A, Ward SR, Fridén J, Lieber RL. Mechanical strength of the sideto-side versus Pulvertaft weave tendon repair. J Hand Surg. 2010;35(4):540–545.
- Chen TM, Rozen WM, Pan WR, Ashton MW, Richardson MD, Taylor GI. The arterial anatomy of the Achilles tendon: anatomical study and clinical implications. Clin Anat. 2009;22(3):377–385.
- Elias I, Besser M, Nazarian LN, Raikin SM. Reconstruction for missed or neglected Achilles tendon rupture with VY lengthening and flexor hallucis longus tendon transfer through one incision. Foot Ankle Int. 2007;28(12):1238–1248.
- Hahn F, Meyer P, Maiwald C, Zanetti M, Vienne P. Treatment of chronic Achilles tendinopathy and ruptures with flexor hallucis tendon transfer: clinical outcome and MRI findings. Foot Ankle Int. 2008;29(8): 794–802.
- Karnovsky SC, Drakos MC. Revision Achilles reconstruction with hamstring autograft and FHL tendon transfer in an athlete. HSS J. 2017;13(3):302–306.
- Lee DK. Achilles tendon repair with acellular tissue graft augmentation in neglected ruptures. J Foot Ankle Surg. 2007;46(6):451–455.
- Saxena A. Surgery for chronic Achilles tendon problems. J Foot Ankle Surg. 1995;34(3):294– 300.


