Bunions
Medically reviewed by Jonathan T. Deland, MD
Summary: This article provides an overview of bunions, a deformity at the base of the big toe often linked with hallux valgus. It explains what causes bunions, how they are diagnosed, and the difference between mild cases that can be managed with shoe changes or medications and more advanced cases that may require surgery. Readers will also learn about the different surgical options, recovery timelines, and why choosing an experienced foot and ankle surgeon is important for lasting results.
On this page:
What is a bunion?
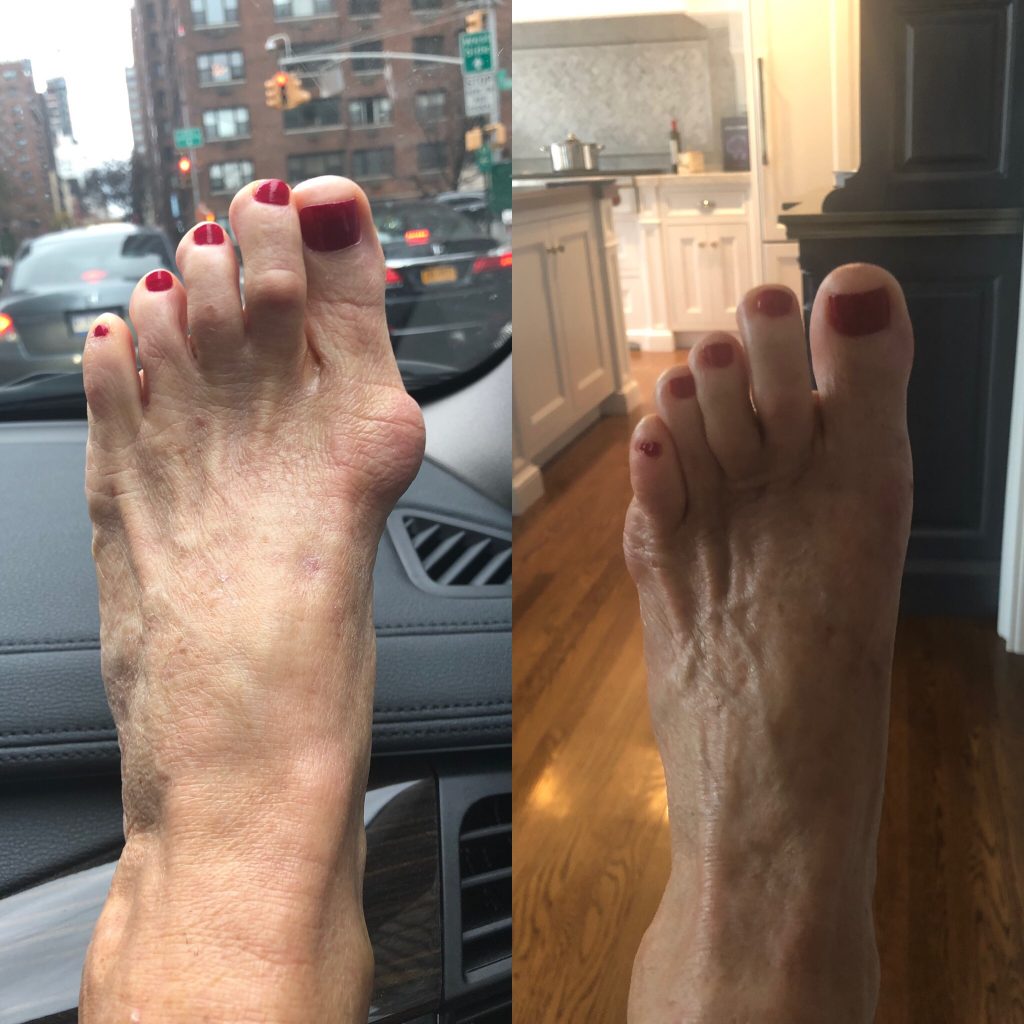
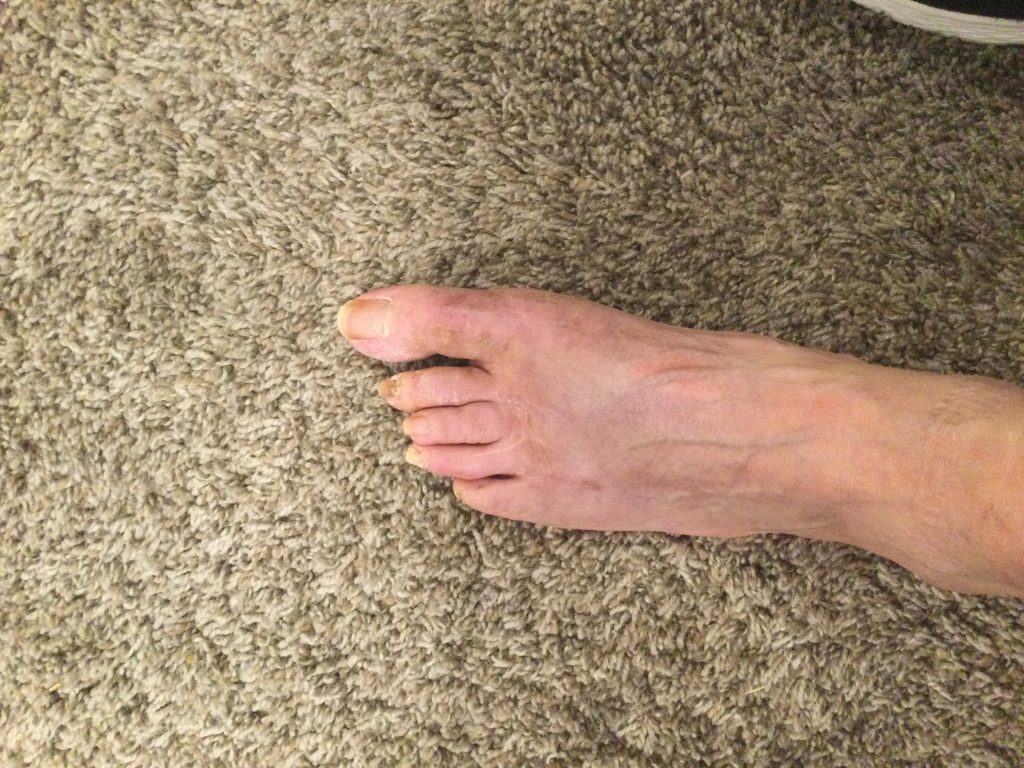
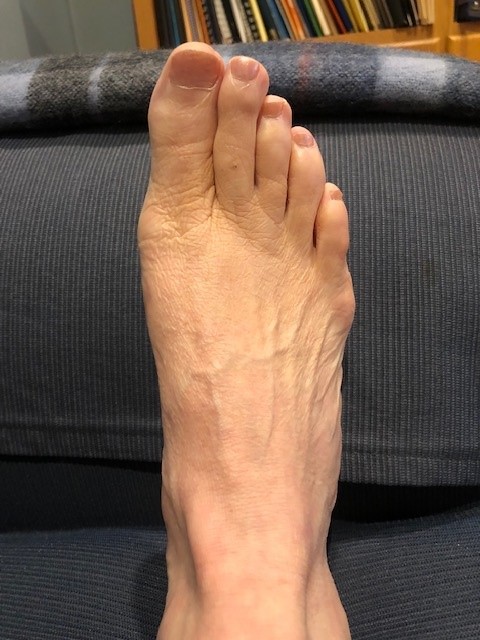
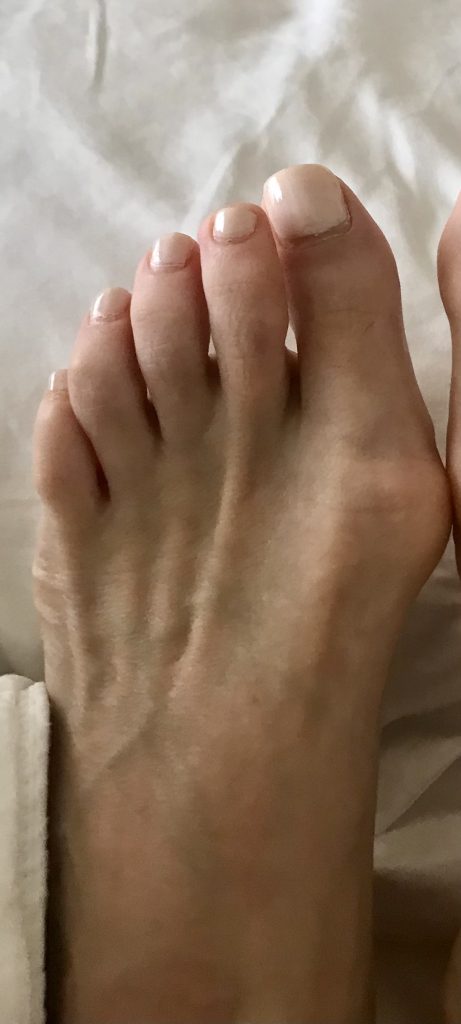
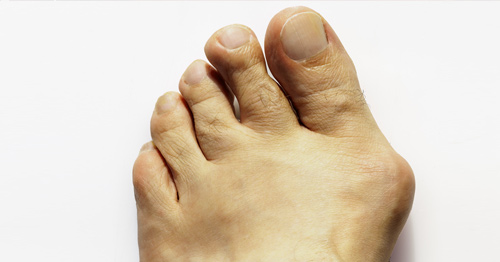
The term bunion, as it is popularly used, describes a variety of deformities involving a painful bump and swelling at the base of the big toe. Orthopedists use additional terms to describe the different individual deformities. A condition in which the big toe deviates from the normal position and angles inward toward the second toe is referred to as hallux valgus.
Technically speaking, the word bunion refers specifically to an enlarged bump made of bone and sometimes including an inflamed bursa. This inflammation is caused by the bony prominence (bump) and develops on the bursa of the first metatarsal head at the base of the big toe. Although a bunion can develop without hallux valgus, this article discusses only bunions that include hallux valgus. (Dorsal bunions are a completely different variety, in which the bump appears on the top of the base of the toe. These are often the result of arthritis in the toe joint.)
What causes bunions?
Doctors and scientists have not been able to identify a single cause or set of causes for bunions. However, heredity and gender each play a role. Bunions tend to run in families, and women develop bunions more frequently than men. In addition, the foot gradually widens with age as the ligaments that connect the bones in the forefoot become more lax.
Contrary to what many people believe, poorly fitting shoes do not cause bunions. In fact, bunions are found in populations all over the world, including among those who never wear shoes. Shoes that are too tight can, however, contribute to the progression of the condition. Bunions are often bilateral, that is, appearing in both feet. Although bunions are usually seen in people who are middle-aged or older, even teenagers sometimes develop them, usually as a result of a congenital condition.
How are bunions diagnosed?
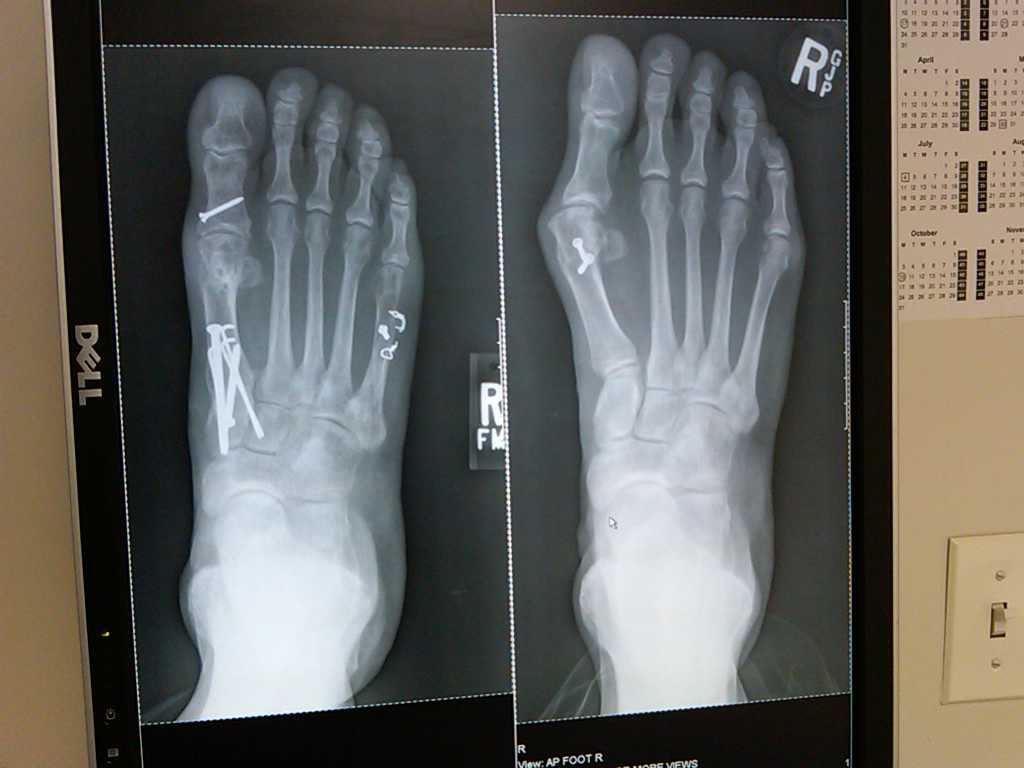
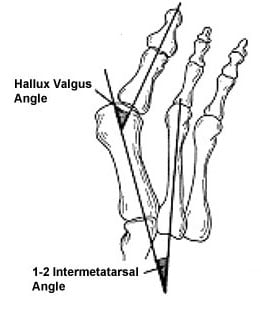
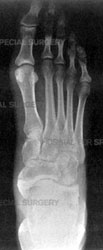
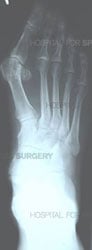
Orthopedic surgeons diagnose bunions on the basis of a physical examination and X-rays taken while the person is weightbearing (standing). Two angles are assessed:
- Intermetatarsal angle – the angle between the first and second metatarsals (the bones that lead up to the bases of the big toe and second toe). If this angle is wider than nine degrees (9º), it is abnormal and referred to as metatarsus primus varus.
- Hallux valgus angle – the angle of the big toe as it drifts toward the small toe. An angle that exceeds 15º is considered to be a sign of hallux valgus.
How is bunion pain treated?
Although some people feel that their bunion is unattractive, the condition is not always painful. If you have only minor discomfort due to a bunion, your toe and foot pain may be eased by wearing wider shoes made of soft leather and/or with the aid of spacers – padding placed between the toes to correct alignment. You may need no additional treatment.
More serious cases may require one or both of the following:
- Anti-inflammatory medications – to alleviate temporary discomfort at the site of a bursa.
- Surgery – for those who continue to experience pain on a daily basis and who cannot wear most types of shoes comfortably. Orthopedic foot and ankle specialists at HSS perform more than 400 bunion surgeries a year.
When is bunion surgery recommended?
There are different reasons to consider bunion surgery. Cosmetic concerns alone are not a sufficient reason to have surgery. If a person has pain in reasonable shoes, has tried wearing wider shoes with no relief and pain been a long-term problem or is worsening, surgery should be considered. Also, if the big toe is pushing against or overlapping the second toe and causing pain in that toe, the bunion must be addressed in order to take care of the painful second toe.
Another symptom that may require surgery is instability in the first ray (a combination of the medial cuneiform bone and first metatarsal bones, which nestle together and connect to the bones of the big toe) with pain on the ball of the foot (the portion of the foot at the base of the toes under the metatarsals from the tip of the toe, back up to the midfoot).
Surgical treatment for bunion deformities usually involves an osteotomy to restore proper alignment. Different techniques are used, depending on the type of deformity. The technique your foot surgeon will select is guided by considering the:
- Degree of deformity in the foot.
- Strategic goal of preventing a future recurrence of the bunion.
- Way to achieve the quickest possible recovery.
Some of the more common bunion surgery procedures are:
- Distal chevron osteotomy – in which a v-shaped cut is made at the toe end of the first metatarsal. This surgery is appropriate for individuals who have a painful prominence (bump) at the base of the big toe, but where the joint is still well aligned. To maintain alignment during the healing process absorbable orthopedic pins (also called "bioabsorbable pins," these are implants that eventually dissolve away) are placed in the first metatarsal.
- Scarf osteotomy (also known as the percutaneous proximal oblique osteotomy or Ludloff osteotomy) – in this procedure, a more extensive cut is made higher up in the metatarsal to correct a moderate incongruent deformity and metatarsus primus varus. Screws are used to maintain alignment during healing.
- Crescent osteotomy – in which a curved cut is made at the base of the metatarsal. This is appropriate for patients with more severe metatarsus primus varus, which requires more correction. Screws or pins are used to maintain alignment.
- Lapidus procedure – a joint fusion for people who have severe deformity, instability of the first ray, with a loose metatarsal-tarsal joint (located in the midfoot), where an osteotomy alone may not be enough to correct the problems. The looseness of the joint may lead to bunion recurrence or cause pain on the ball of the foot because the first metatarsal is floating up, allowing for excessive weight to go to adjacent metatarsals (commonly the second and the third). In such cases, the metatarsal-tarsal joint is fused to provide lasting stability. Screws are used to maintain alignment. The loss of motion from the fusion is small and does not significantly limit motion of the big toe.
Patients undergoing bunion surgery are given a regional anesthesia ankle block, which anesthetizes the foot from the ankle down. Depending on individual preference, a sedative may be given as well and the patient can be as sedated as they wish. The ankle block administered as anesthesia provides pain relief for up to 12 hours following surgery. Strong pain relievers are provided and anti-inflammatories can be used as well. Bunion surgery has a reputation for being painful. But with appropriate pain management and elevation of the foot, this can be minimized.
All bunion surgeries can be done on an ambulatory (outpatient) basis, eliminating the need to stay overnight at the hospital. HSS offers minimally invasive bunion surgery options.
What is the recovery time for bunion surgery?
Length of recovery from bunion surgery varies according to the nature of the procedure.
- Those who have had a distal chevron procedure are able to bear some weight on the foot on the day following surgery.
- Those who have had a scarf procedure can bear partial weight at about weeks. Crutches are used to assist in walking.
- People who have a Lapidus procedure must wear a cast and use crutches for eight weeks. Regardless of the procedure used, swelling will persist for some time with a gradual reduction over the course of the post-surgery year.
- Patients who undergo either a distal chevron, scarf or crescent osteotomy should be able to wear some type of shoe or sneaker after 6 to 7 weeks.
- Those undergoing the lapidus fusion will probably need to wait 10 to 12 weeks before they are able to wear shoes.
Formal physical therapy is most often not necessary. Patients are given range of motion exercises for the toe. Therapy is used only if progress with the motion is slow.
Overall, outcomes for bunion surgeries are quite good. However, orthopedic surgeons on the Foot and Ankle Service at HSS often treat patients who have had unsatisfactory outcomes from surgery at other institutions. While the problems resulting from these surgeries can be addressed, the success rates are better when the proper procedure is expertly done the first time.
If you are considering surgery to correct a bunion, consult an orthopedic surgeon who is experienced in a wide range of surgical techniques – the simpler procedures as well as those that are complex. You should feel confident that you are getting the right surgery for your condition, and that the recovery and rehabilitation process will be appropriate and effective. Avoid committing to any procedure in which the bunion is simply "shaved down" rather than correctly addressing the metatarsal deformity. Shaving a bunion may only provide a temporary solution. A shaved bunion may come back in the future.
Key takeaways
- A bunion is a bony bump at the base of the big toe, usually with hallux valgus (toe angling inward).
- Genetics, aging, and ligament laxity play a larger role than footwear, though tight shoes can aggravate bunions.
- Diagnosis relies on physical exam and X-rays measuring toe angles.
- Non-surgical care includes wide shoes, padding, and anti-inflammatory medication.
- Surgery is recommended for ongoing pain or significant deformity, not cosmetic reasons alone.
- Multiple surgical options exist (chevron, scarf, crescent osteotomy, Lapidus fusion), chosen based on severity.
- Recovery times vary by procedure, but outcomes are generally very good when surgery is performed appropriately.