Broken Hip (Hip Fracture)
Although related, there are differences between the terms "hip fracture" and "pelvic fracture." A portion of the pelvis makes up the hip joint, but not all pelvic fractures affect the hip joint. A fracture of the hip may occur at the top of the femur where it meets the pelvis, the acetabulum (the portion of the pelvis that connects to the femur to form the hip), or both.
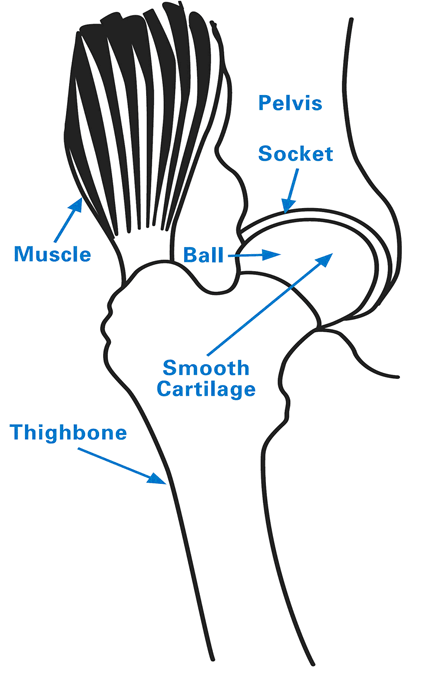
Anatomy of the hip
The hip is a ball-and-socket joint. The ball, at the top of your femur (thighbone) is called the femoral head. The socket, called the acetabulum, is a part of your pelvis. The ball moves in the socket, allowing your leg to rotate and move forward, backward and sideways. A hip fracture is a break in either the upper portion of the femur or of the pelvis.
Femoral hip fractures
The term "broken hip" usually refers to a fracture of the ball side of the hip joint, that is, a break in the upper femur, generally in one of three areas:
- the femoral neck (just below the femoral head) – called an intracapsular fracture (most common)
- immediately below the femoral neck – called an intertrochanteric fracture
- the upper femoral shaft below the femoral neck – called a subtrochanteric fracture (least common)
Hip fractures frequently occur in the elderly, people affected by disease, or from direct trauma. Femoral hip fractures can be treated relatively easily, with our without surgery, depending on the severity of the injury.
Pelvic and acetabular hip fractures
A fracture of the acetabulum or other portion of the pelvis is often a more serious injury that requires prompt surgery (in some cases, multiple surgeries). These types of breaks are often the result of high-impact trauma such as a car vehicle accident or a bad fall. However, they can occur during a lower-impact fall, primarily in older adults who have fragile bones due to osteoporosis.
In fractures of this type, the femoral head is often driven through the acetabulum because of the impact of the fall or accident. If the fracture causes the femoral head to pop outside the acetabulum, this is known as a dislocated hip.
Treating acetabular fractures is complex because this section of bone is very close to:
- the major blood vessels to the legs
- the sciatic nerve (the major nerve that arises from the lower spine and provides sensation and movement to the leg and foot)
- the intestines, the ureter and the bladder
What is the most common cause of a pelvic fracture?
The most common type of pelvic fracture is towards the front (the pubic bones), which occurs in older patients, usually due in part to thinning of the bones from osteoporosis. Commonly, a person will loses their balance, land awkwardly, breaking the pelvis. People can also lose their balance and cause their muscles to pull so hard against each other that they can pull the pelvis apart.
Most of these fractures will heal themselves with time.
Do pelvic fractures always require surgery?
Many pelvic fractures are treated without surgery. Some patients don’t need surgery because the type of fracture (meaning, where it is located in the pelvis) is not dangerous, and the fracture is likely to heal of its own accord. There are also fractures that are not severe in that the broken bones are very close together and again are likely to heal on their own. In contrast, a patient may have fractures that are very severe or there may be other severe injuries that require surgery.
In many cases, the patient’s health may be too precarious to permit safe completion of an orthopedic surgery, even though it might be recommended.
Is a cast or brace needed for a pelvic fracture to heal?
Most pelvic fractures heal on their own without any bracing or casting for a full recovery. The local tissues in the area of the fracture frequently keep the fracture pieces in order and the bones heal with a little rest and good nutrition. This tends to occur a little more slowly in older people, but the same cells that heal fractures when you are young do the same when you are older. Rarely, orthoses may be used around the pelvis.
How long is recovery from a pelvic fracture?
Pelvic fractures usually start to heal about four weeks after the fracture. Some patients may notice less pain as soon as a few days after a fracture, depending on the severity of the fracture, but most patients take pain medication for four to six weeks after the injury. Final resolution of pain and restoration of function can take six to 12 weeks.
In terms of activity, patients can be bedbound for days or up to a week. Most patients, however, start transferring to a chair in a couple of days and start getting around the bedside with a walker in another couple of days.
Why do some pelvic fracture patients need more than one surgery?
There are a variety of reasons for multiple surgeries:
- There may be several different fractures in different areas of the pelvis requiring separate surgical procedures either under one anesthetic or under several anesthetics.
- The patient may have suffered many injuries and is only able to withstand one operation at a time.
- Some patients are stabilized after a severe trauma with a smaller operation to save their life and allow comfortable further non-orthopedic life-saving care. When they are sufficiently stabilized, they can then return to the operating room for the definitive surgery.
- Some patients have implants inserted, which are removed at a separate operation after healing because the implants may cause or are causing pain or other problems.
Learn more from the articles below.