Registries Advance Patient Care
Adapted from the Fall 2012 issue of Discovery to Recovery
For almost 150 years, HSS physicians and scientists have developed new orthopedic devices and treatments to help patients live the most active lives possible. In the 1960s and 70s, we pioneered the modern artificial knee replacement, developing design concepts and surgical techniques that are now used throughout the world. Back then, investigating how well patients did with a new implant meant manually combing through patient charts and entering data into spreadsheets.
Today, electronic databases called patient registries have vastly improved the way clinical research is conducted at HSS – 84,000 people have been enrolled across 43 registries focused on specific diseases or treatments. Tracking thousands of patients over time through questionnaires and office visits allows researchers to gather valuable information about how well patients are doing months and years after the initial injury, surgery, or diagnosis, answering questions about a specific implant, procedure, or patient characteristic with speed and efficiency, so that physicians can continue to provide patients with the safest, most effective treatment options.
“Our registries allow our surgeons to gain a better understanding of what works best for our patients. This information guides practice decisions and allows us to continuously improve patient care,” says Thomas Sculco, MD, surgeon-in-chief.
Total Joint Registries: Current Findings
HSS’s total joint replacement registries are the Hospital’s largest, enrolling more than 20,000 patients. Douglas Padgett, MD, chief of the Adult Reconstruction and Joint Replacement Division (ARJR), says: “The only way to really know what patients’ outcomes are after surgery is to follow large groups of patients in a registry. HSS now has a rigorous infrastructure in place to collect data about every hip and knee replacement patient, and how they are doing over time. When a patient enrolls in a registry, our goal is to keep in touch with them over the long-term, to really understand how we have helped them achieve their goals, and how we could improve.”
HSS is uniquely situated to study joint replacement outcomes because our surgeons perform more than 8,000 joint replacements per year – more than any other hospital in the United States.
Squeaky Hips
Registry data enable surgeons to evaluate how well patients do with a specific type of implant. For example, surgeons recently noticed that a small percentage of patients with ceramic-on-ceramic hip implants (in which both implant parts – the ball and socket – are made of ceramic) complained of a “squeaking” sound coming from their hips. While the squeak was not accompanied by pain or discomfort, it was embarrassing. Because squeaking is uncommon following hip replacement, a team of ARJR surgeons led by Geoffrey Westrich, MD, co-director of Joint Replacement Research at HSS, investigated if these implants were also associated with increased complications.
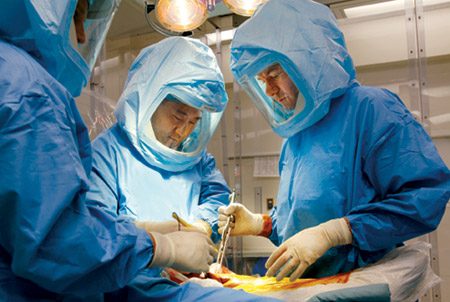
HSS surgeons use registry findings to improve patient care.
Because 364 patients with ceramic-on-ceramic implants were enrolled in the ARJR registry, the surgeons were able to achieve significant findings in less than a year. To complete this study, a “noise survey” was simply added to the usual registry questionnaire.
The study found excellent results associated with these implants, with patients moving comfortably and with less pain. In addition, fewer than two percent of patients reported a squeak. While ceramicon-ceramic implants have become less popular over time, this research confirmed them as an excellent choice for appropriate patients.
When Women Wait
A grant from the Agency for Healthcare Research and Quality was used to support the expansion of the ARJR registries to include self-reported information from patients about how they were feeling (e.g., “How easily can you go up and down stairs?” and “How much pain do you have?”).
Dr. Westrich and his team recently analyzed these unique self-reported data. Looking at 5,945 patients who had joint replacements at HSS, they discovered that women were significantly more likely to live alone, experience severe pain, and have limited activity prior to surgery, placing them at possible increased risk for complications and worse outcomes following surgery.
The authors see these findings as a call-to-action to educate patients about their options so they will seek help sooner. “When women live alone, they might wait until they suffer from severe pain and disability before getting the surgery they need, putting themselves at greater risk. The more fit someone is before surgery, the easier their follow-up therapy is going to be,” says Dr. Westrich. “We need to reach out to people and tell them – if you have arthritis, if you’re suffering, don’t wait. Even if you live alone there are options for rehabilitation that will work for you.”
Aligning Expectations
HSS surgeons recently used registry data to learn whether patients and physicians report post-surgical complications in the same way. They wanted to find out if patients know what to expect in their postsurgical experience, since previous research has shown that patients with realistic expectations achieve better results following surgery. They also had questions about the accuracy of patient-reported data. The new HSS studies, published in the Journal of Arthroplasty, involved 3,278 knee and 3,976 hip replacement patients. Whenever a patient reported a complication in their registry questionnaire, a physician followed up with a chart review, a clinical exam, and a review of the patient’s x-rays.
Patients and physicians reported most complications similarly, pointing to how well most patients understand what normal side effects and complications to expect after surgery. However, patients over reported “major bleeding,” sometimes confusing a normal post-surgical level of bleeding or bruising with this more serious complication.
These studies point to the continued importance of patient education, physician-patient communication prior to total joint replacement surgery, and constant refinement of the methods used to gather registry data. “We need to continue to take the time to educate patients about what to expect after surgery as part of the normal healing process,” says HSS surgeon and study co-author Michael Alexiades, MD.
Improving Care for Patients
Registries allow our doctors and scientists to identify long-term trends and quickly evaluate how well patients do with a specific implant or surgery. These findings help drive the way we practice medicine, since providing patients with the best results is always our top priority.
Read the full Discovery to Recovery Fall 2012 issue.
Posted: 5/29/2013
Authors
Success Stories
In-person and virtual
physician appointments
Or call
+1.877.606.1555