Basal Thumb Arthritis: An Overview
Diagnosing and treating arthritis joint pain at the base of the thumb - an interview with Dr. Robert N. Hotchkiss
Overview
Arthritis at the base of the thumb is one of the most common locations and can be very disabling. Because the strength and motion of the thumb is required for nearly every activity - whether writing, opening a jar, or buttoning a shirt - pain from this condition may impede the most basic everyday tasks.
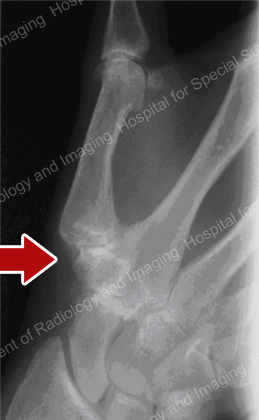
Figure 1: Radiograph (X-ray) of the hand, with an arrow pointing to an arthritic basal joint of the thumb.
Like other forms of osteoarthritis, basal thumb arthritis develops when cartilage on the surfaces of the bones that meet at the joint wears away and the metacarpal bone begins to slip out of the joint. This loss of alignment often creates the appearance of a bump near the wrist. For reasons that remain unclear, the degree of inflammation and associated pain can fluctuate.
Arthritis in this location generally begins in patients from 40-50 yrs old, often with the X-ray appearance in advance of the symptoms. In fact many people—especially women, in whom the condition is more prevalent –may have some degree of basal thumb arthritis by X-ray without being aware of it, according to Robert N. Hotchkiss, MD, Associate Attending Orthopaedic Surgeon at Hospital for Special Surgery (HSS).
“What we are able to see on X-ray does not necessarily correspond to what the patient feels,” Dr. Hotchkiss explains. “We may see relatively advanced arthritis in the joint, yet the patient reports very little pain.”
Part of the explanation for this lies in the tendency to adapt to the painful thumb by altering one’s activities. Unfortunately, this can result in a cycle of diminished use and resulting lessening of strength in the hand.
Basal thumb arthritis is almost always bilateral (occurring in both hands), but contrary to what a patient might expect may only cause symptoms in the non-dominant hand. “The condition is not related to specific activities that the individual has participated in,” Dr. Hotchkiss says, “Instead, there appears to be a genetic or anatomic component in its origin.”
Diagnosing and Managing Basal Thumb Arthritis
Orthopedic surgeons diagnose basal thumb arthritis based on the history and physical examination that includes evaluation of pinch strength between the thumb and index finger. The surgeon also checks to see whether there is arthritis in any of the adjacent joints by X-ray.
Determining the appropriate treatment for a patient with basal thumb arthritis is a highly individualized process, according to Dr. Hotchkiss, in which the physician and patient must factor in the degree to which the arthritis interferes with activities of daily living, pain experienced by the patient, and patient expectations.
In addition, the natural course of the condition can dictate treatment. “Some patients feel they can live with the condition, but want temporary pain relief so that they may participate in or enjoy a specific event such as a sports tournament or a wedding,” says Dr. Hotchkiss. In fact, over time, if the joint has not subluxated (displaced) significantly, it may stiffen in position and therefore become less painful.
Moreover, increasing longevity and activity in later years has changed the way this condition is approached. “Where we might once have looked at an older patient and thought that we need only consider the next four to five years, now we have to think about how we can get ten to twenty years’ more durability and use from the joint. This is a question we haven’t fully answered,” Dr. Hotchkiss says.
Nonsurgical Treatment Options
Nonsurgical treatment options for basal joint arthritis include the use of oral medications or the injection of corticosteroid into the joint. These injections can be quite helpful and often provide relief for several months. Patients commonly worry about the frequency or quantity of these injections. However, with well documented safety, many patients have benefited from multiple, but infrequent injections over several years. Many patients do not proceed to the need for surgery.
The use of viscosupplementation, or hyaluronic acid (HA) injections, has shown promise in other joints and is undergoing studies. There is anecdotal evidence that some patients have benefited from the "off-label" injection of HA, who no longer benefited from corticosteroid injection. As Dr. Hotchkiss affirms, he has treated patients who, after showing no response to treatment with a corticosteroid and scheduling surgery, had “remarkable improvement” after an injection of hyaluronic acid.
(It is important to note that hyaluronic acid injections are administered "off label," which means that the FDA has not approved this treatment for use in basal thumb arthritis, and that healthcare insurance will not provide reimbursement. Hyaluronic acid injections are approved by the FDA for use in osteoarthritis of the knee.)
Surgical Treatment Options
Patients who do not respond to non-operative treatment and/or have significant subluxation of the joint may be advised to consider surgery for basal thumb arthritis. According to Dr. Hotchkiss, orthopedic surgeons have yet to reach consensus on the optimal approach. For some patients, particularly those individuals who want to maintain a strong grip, fusion of the two bones may be appropriate. While this procedure also offers effective pain relief, it limits mobility to a considerable degree.
Another surgical option is partial or total removal of the trapezium (the bone that forms the base of the joint), accompanied by rerouting an expendable tendon near the thumb. The tendon is re-routed to provide a cushion and stabilize the base of the metacarpal joint. “Surgery usually provides excellent pain relief,” Dr. Hotchkiss says, “but the degree of function and strength that is restored varies.”
Unfortunately, joint replacement with prosthetic components - of the type that has been so successful in the hip or knee - has not been reliable for this condition. However, orthopedic surgeons and researchers continue to look at new devices and materials that might be helpful. “We want to give patients the widest array of choices possible to achieve a good outcome,” Dr. Hotchkiss says.
Looking to the future
Considerable research on basal thumb arthritis and its treatment is underway. At HSS, Dr. Hotchkiss is presently involved in a number of studies, including those in which treatment with viscosupplementation (hyaluronic acid) is being compared to corticosteroid injections and to administration of a placebo.
He and his colleagues at HSS also maintain a thumb registry that allows them to follow almost 900 patients with the condition, in order to assess the success of various modes of treatment. They also continue to work on refining outcome instruments, tools that are intended to yield reliable information as patients are followed over time.
If you would like more information about the treatment of basal thumb arthritis at HSS, please visit the Physician Referral Service or call 1.877.606.1555.
Summary prepared by Nancy Novick
Authors
Medical Director of Clinical Research, Hospital for Special Surgery
Associate Attending Orthopaedic Surgeon, Hospital for Special Surgery
