Raynaud's Phenomenon
- What is Raynaud's phenomenon?
- What is Raynaud's phenomenon versus Raynaud's syndrome?
- What are the symptoms of Raynaud's?
- What is the cause of primary Raynaud's phenomenon?
- What conditions are associated with secondary Raynaud's?
- What medications/drugs can worsen Raynaud's?
- When should I see a doctor about Raynaud's?
- How is Raynaud's diagnosed?
What is Raynaud's phenomenon?
Raynaud’s phenomenon is an exaggerated constriction of blood vessels to the extremities. This condition occurs in more than 3% of the population and is more common in women than in men. Raynaud’s is generally broken down into two types: primary Raynaud's and secondary Raynaud's. Primary Raynaud’s occurs in individuals who are otherwise healthy, while the secondary type arises in association with another condition, most often one of a group of disorders called connective tissue diseases, such as scleroderma, lupus and myositis. Raynaud’s is named after the French physician Auguste Gabriel Maurice Raynaud, who first described its characteristics in 1862.
HSS has rheumatologists with special expertise with Raynaud's, including:
What is the difference between Raynaud's phenomenon and Raynaud's syndrome?
Raynaud’s phenomenon refers to episodic skin color changes caused by cold temperatures, most commonly found in the ends of the fingers. Sometimes, Raynaud’s is referred to as Raynaud’s syndrome. Raynaud’s syndrome, however, is when Raynaud’s phenomenon occurs as one of several other symptoms of an autoimmune condition. This is also referred to as secondary Raynaud’s phenomenon.
What are the symptoms of Raynaud’s?
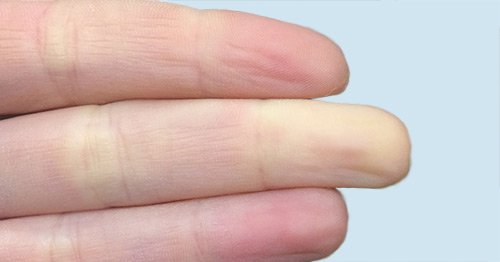
The main symptoms are color changes in the hands, fingers, and other extremities (often in the feet, sometimes, the ears and nose). Affected body parts will often first become white or lighter than a person's normal skin tone, and then turn blue. Discomfort or even severe pain may accompany the color change. Secondary Raynaud’s is more likely to be associated with other complications, such as ulcers on the fingers or fingertip infections, more so than primary Raynaud’s.
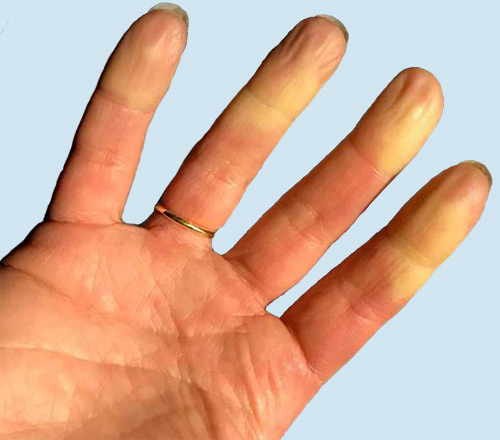
Raynaud’s is triggered by cold temperatures or emotional stress, but it is different from simply having cold hands. The condition involves both coolness and the characteristic white and blue color changes in the affected areas. Some people have only one color change in the cold – such as only white or only blue. These people are considered to have “possible” Raynaud's phenomenon.
What is the cause of primary Raynaud’s phenomenon?
The cause of primary Raynaud’s is unknown. Primary Raynaud’s is more common in females and tends to occur in early adulthood and among those with a family history of Raynaud’s.
Secondary Raynaud’s can be caused by certain medications as well as local trauma, but more commonly, it is related to an underlying connective tissue condition.
Is Raynaud’s an autoimmune disorder?
Raynaud’s may be a symptom of an underlying autoimmune disorder and, in these cases, is known as secondary Raynaud’s or, sometimes, Raynaud’s syndrome. Raynaud’s may also occur in a primary form in the absence of an underlying autoimmune disorder.
What conditions are associated with secondary Raynaud’s?
Some examples of autoimmune conditions associated with Raynaud’s include:
- scleroderma* – which includes systemic sclerosis, and CREST syndrome
- lupus
- mixed connective tissue disease
- myositis
- Sjogren’s syndrome
- rheumatoid arthritis
*Learn about our Scleroderma Fast Track patient program
What medications/drugs can worsen Raynaud’s?
Some medications and/or substances that may worsen Raynaud’s include:
- beta blockers (such as metoprolol, propranolol)
- nasal decongestants (such as phenylephrine, pseudoephedrine)
- migraine medications (such as sumatriptan, ergotamine)
- ADHD medications (such as methylphenidate, dextroamphetamine)
- nicotine / tobacco use
- cocaine
When should I see a doctor about Raynaud’s?
A physician can help to diagnose primary versus secondary Raynaud’s phenomenon and to distinguish between Raynaud’s and other causes of low blood flow to the fingers. Color changes of the extremities can have other causes, especially if these changes are present only on one side of the body (Raynaud’s usually affects both sides of the body). Especially when the problem is not symmetrical, it’s important to rule out other causes, such as a blood clot in an artery or hardening of the arteries.
It is especially important to see a doctor if someone with Raynaud’s:
- develops ulcerations of the fingertips or toes
- has severe episodes of Raynaud’s
- has new onset Raynaud’s (particularly later in adulthood)
- experiences other symptoms that suggest the presence of an autoimmune condition (such as joint pain, rash, weakness, among others)
How is Raynaud’s diagnosed?
Raynaud’s can be diagnosed by a healthcare provider based on the description of a patient’s symptoms. Taking a photo during a typical attack to share with the doctor can also be very helpful to confirm the changes are characteristic of Raynaud’s. A physical exam is also performed and may include examination of the finger blood vessels using a microscope. Recording a patient’s medical history, conducting a physical exam, and ordering blood tests are helpful to distinguish between primary and secondary Raynaud’s.
For those whose Raynaud’s does not respond to behavior changes alone, medications can be added that dilate the blood vessels in the small extremities. These vasodilators help to prevent recurrences or to make them milder. In more severe cases, a nerve block that quiets the sympathetic nerves at the wrist can help the blood vessels dilate and end a painful episode. In the most severe cases that fail to respond to other treatments, a surgical procedure called a sympathectomy can allow the finger blood vessels to dilate. It’s especially important to seek treatment if the Raynaud’s is severe enough to cause major, continuing pain or is associated with ulcers or infections of the fingers.
Raynaud’s treatment at HSS
Hospital for Special Surgery’s specialists in rheumatology and pediatric rheumatology manage cases of both primary and secondary Raynaud's phenomenon. When needed, our anesthesiology specialists provide nerve blocks, and our Hand and Upper Extremity Service can provide surgical assistance for the most difficult cases. A rheumatologist can also help to separate primary from secondary Raynaud’s by searching for any clues to an associated inflammatory condition.
Articles related to Raynaud's phenomenon
- Scleroderma and Systemic Sclerosis (SSc): An Overview
- Scleroderma, Myositis and Vasculitis: Symptom Management and Activities of Daily Living
- Undifferentiated Connective Tissue Disease – In-Depth Overview
- Cutaneous Lupus and Lupus Rashes: What You Need to Know
- Lupus Blood Test Results Explained
- Lupus, Sexuality and Intimacy
- Telangiectasia and Autoimmune Disease
Raynaud's Phenomenon Patient Stories
Updated: 8/10/2023
Reviewed and updated by Jessica K. Gordon, MD and Kimberly (Showalter) Lakin, MD, MS