Partial Knee Replacement: A Treatment Option in Unicompartmental Knee Arthritis
Over the course of their lifetimes, approximately one in five Americans* will develop knee arthritis. Fortunately, a wide range of nonsurgical and surgical techniques are available to address the discomfort and disability that can accompany this condition. Total knee replacement is the most common surgical procedure for late-stage knee arthritis, but partial knee replacement is a surgical treatment option for some patients who have arthritis in only one portion of the knee.

What is unicompartmental knee arthritis?
Unicompartmental osteoarthritis of the knee is a condition in which degenerative arthritis affects only one part of the knee joint, while the other regions (or “compartments”) of the knee remain healthy or not significantly damaged.
Knee joint anatomy
The knee joint is composed of three bones: The femur (thighbone), the patella (kneecap) and the tibia (shinbone). Two knob-like protuberances on the bottom of the femur known as the femoral condyles make up the top of the knee. The upper portion of the tibia known, as the tibial plateau, makes up the bottom. The kneecap rests in front of the femoral condyles.
There are three compartments of the knee, each named for its relationship to these portions of bone:
- The medial (inner) compartment of the knee.
- The lateral (outer) compartment is formed by the articulation (or joining) of the lowest part of the thighbone (femur) and the highest part of the shinbone (the tibia).
- The patellofemoral compartment, located where patella rests in front of the femur.
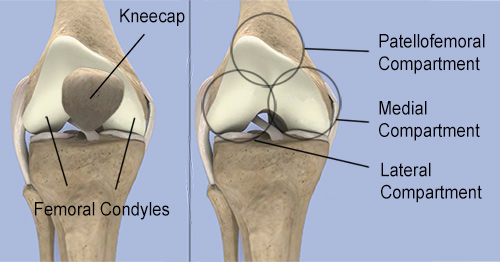
Arthritis of the knee may occur in any one of these compartments. However, the medial compartment is the most frequent site of knee osteoarthritis, followed by the lateral compartment. (Arthritis that is confined to the patellofemoral compartment of the knee is rare and may require a patellofemoral joint replacement.)
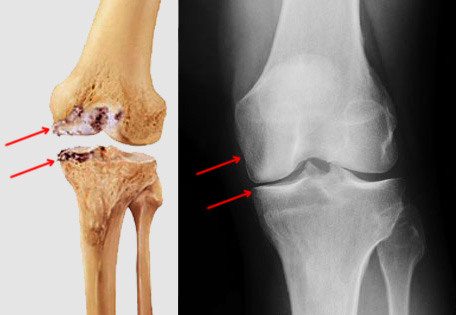
Illustration and X-ray images of medial compartment osteoarthritis of the knee
What is partial knee replacement surgery?
Partial knee replacement is where the bone surfaces of only one compartment of the knee joint are removed and replaced with implants, as compared to that of multiple compartments in the case of a total knee replacement. It is a common treatment for unicompartmental arthritis.
“Patients with unicompartmental knee arthritis have cartilage degeneration in only one section or compartment of the knee. In cases where nonsurgical techniques do not provide symptom relief, surgeons can remove damaged cartilage and bone in the diseased area only, while preserving the ligaments that help support the knee joint,” explains Friedrich Boettner, MD, Attending Orthopedic Surgeon at HSS. (Find a knee replacement surgeon at HSS to suit your specific condition, location and insurance.)
An implant − which may also be called a prosthesis − takes the place of the damaged area of the knee, leaving the other compartments intact. Improvements in surgical techniques and instrumentation have made partial knee replacement an increasingly viable option for a growing number of patients. In fact, recent data suggests that anywhere from 10% to 25% of all patients with osteoarthritis of the knee needing replacement surgery may be eligible for the procedure. (Find a surgeon at HSS who performs partial knee replacement.)
Is partial knee resurfacing the same thing as partial knee replacement?
Yes. Partial knee replacement is also referred to as "partial knee resurfacing surgery," "unicompartmental knee replacement," "unicondylar knee arthroplasty" or "unicondylar knee replacement." Colloquially, it is also sometimes called a "uni." (People sometimes also refer to it as a “half knee replacement,” however this is not accurate, since the procedure involves only one of the knee’s three major compartments.)
If I have partial knee replacement, does that mean that I will no longer have arthritis of the knee?
Partial knee replacement will address the arthritis that is present in the particular compartment of the knee that is already affected. In addition, the knee is typically rebalanced by the procedure, which improves its stability. While rare, there is no guarantee that arthritis will not progress elsewhere in the knee. Should this occur, a surgical revision to a total knee replacement may be necessary.
Who can benefit from partial knee replacement?
Partial knee replacement is appropriate for patients with arthritis that is confined to a single compartment of the knee and is generally restricted to patients who are not morbidly obese (BMI greater than 40). The surgery is not appropriate for patients with marked stiffness in the knee or for those with a significant angular deformity. Generally, a patient must have intact knee ligaments to be a candidate. For example, patients who have had an untreated torn ACL are often not considered for partial knee replacement. People with rheumatoid arthritis of the knee may not be candidates either, since inflammatory arthritis typically affects the entire joint.
Additional considerations are evaluated on a case-by-case basis with the surgeon and patient determining together whether partial knee replacement is the best treatment option. Selecting the right patient is considered one of the most important steps to ensuring a good functional outcome and longevity for a partial knee replacement. Since it involves less of a trauma than does a total knee replacement, this surgery is sometimes favored for patients over the age of 80, even when they do not meet all eligibility criteria.
Are there any age restrictions for getting partial knee replacement surgery?
There are no strict recommendations, but in general, partial knee replacements are appropriate for patients over 40 years old who meet other eligibility criteria.
What happens during partial knee replacement?
During partial knee replacement, the orthopedic surgeon makes a small incision to gain access to the affected compartment of the knee. He or she gently moves supporting structures of the knee out of the way and removes damaged cartilage and bone tissue from the surfaces of the tibia and the femur in the arthritic area. The surgeon then prepares these surfaces for the insertion of the prosthesis components, which are specifically sized for each individual patient’s joint.
Cement is usually used to secure these components, but non-cemented knee replacement implants (also called "uncemented" or "cementless" implants) are also now being used. All surrounding structures and tissues are restored to their anatomic position and the incision is closed.
Some surgeons at HSS apply computer-assisted navigation techniques and robotic tools to perform partial knee replacement. “This technology allows the surgeon to create and manipulate a 3D image of the patient’s knee in advance of surgery, a process that allows for highly precise removal of damaged tissue and refined positioning of the prosthesis during the actual procedure,” says Andrew D. Pearle, MD, Attending Orthopedic Surgeon at HSS.
Is robotic knee replacement technology used in partial knee replacement?
Frequently, yes. For many cases of total knee replacement, the use of robotics for surgery are not necessary to achieve optimal results. But for the inherent technical challenges of partial knee replacements, robotic assistance has been transformative. Using traditional surgical methods, manual insertion of the implant for a partial knee replacement that perfectly matched the patient's anatomy was challenging. With robotic-assisted knee replacement technology, placement of the implant is very precise, matches that person's anatomy exactly, and can be done more quickly.
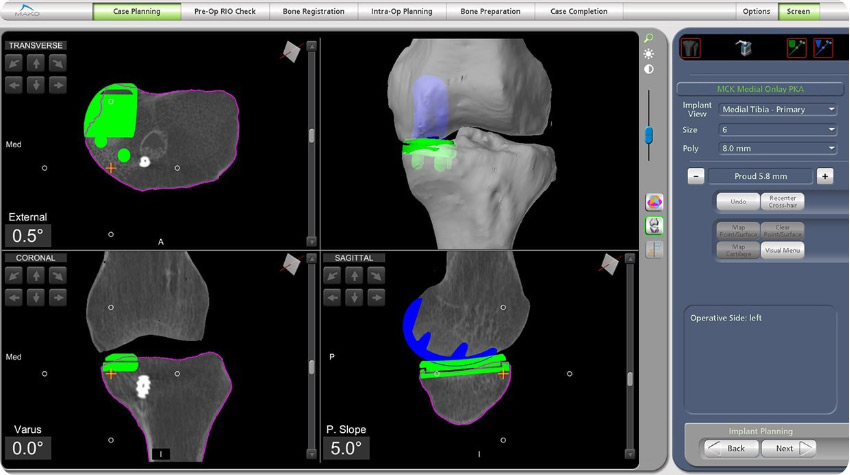
Preoperative planning for a robotic partial knee replacement.
What kind of anesthesia is used during partial knee replacement surgery?
At HSS, patients undergoing partial knee replacement surgery are usually given regional anesthesia, which numbs the lower half of the body and allows the patient to remain awake during the procedure. Nerve blocks are also given to minimize postoperative pain, and the surgeon also injects a local anesthetic “cocktail” around the knee to minimize pain in the first 48 hours after surgery. This cocktail may contain a local anesthetic plus one or more pain medications, corticosteroids or other agents. Throughout partial knee replacement surgery, patients are carefully monitored to minimize the risk of complications.
Is partial knee replacement painful?
All surgeries result in some pain. While pain after partial knee replacement varies by patient, typically patients experience less pain and stiffness following partial knee replacement than they do after total knee replacement. At HSS, we have robust systems and resources dedicated to address post-operative pain management. After partial knee replacement surgery, most patients receive 7 to 14 days of prescription pain medication but HSS also offers a limited opioid pathway for patients who do not tolerate opioid medications well. In addition, clinicians and researchers at HSS are currently using treatment protocols that limit the amount of pain medicine needed after partial knee replacement surgery, utilizing nerve block injections to deliver medication locally.
What is a partial knee replacement prosthesis made of?
All knee replacement prostheses or implants are made of metal and plastic. These surfaces are designed to glide smoothly against one another, just as cartilage does in a healthy knee. Depending on which compartment is affected and whether the patient’s anterior cruciate ligament (ACL) is intact, the surgeon will use either a unicondylar fixed-bearing knee replacement − the most commonly used prosthesis − or a mobile-bearing unicondylar knee replacement.
What is the recovery time for partial knee replacement?
Most patients can expect to be back to their daily activities within three to six weeks. Many patients find that after undergoing physical rehabilitation, they are able to return to sports such as golf within 6 to 10 weeks. Patients can usually expect to go home the same day of surgery, unless they have a medical condition that requires an overnight stay. At HSS, most patients are also able to walk with assistance, or independently, on the same day as their surgery. Typically, the patient is given a cane within days of surgery to allow for increased independence and begins outpatient rehabilitation. Patients are often finished taking prescription pain medication within one to two weeks after surgery.
Will I be able to return to playing sports after my partial knee replacement?
Although not all patients are able to return to unrestricted sports activity, most patients are able to resume biking, golf, tennis and skiing.
What kind of problems can occur with partial knee replacement surgery?
Partial knee replacement usually involves minimal blood loss and is associated with a low rate of complications. As with any joint replacement surgery, complications may include instability of the knee, loosening of the implant, infection, nerve injury and deep vein thrombosis. Generally, complications occur less frequently after partial knee replacement than they do following total knee replacement. Be sure to discuss any concerns you have regarding these or other issues with your surgeon.
Patients who have been properly screened for the procedure can expect to experience a low level of complications and a rapid recovery. However, as with other types of knee surgery, in a small percentage of cases, revision surgeries are required. Results obtained with revision surgery may not be as good as those achieved with primary surgery.
How long does a partial knee replacement last?
A well-done partial knee replacement in an appropriately selected patient can have an implant survival rate that is comparable to that achieved with a total knee replacement in the first decade following surgery. The literature suggests that after the second decade, the revision rate may be somewhat higher for partial knee surgery than for total knee surgery.
Setting the stage for a successful outcome: Surgery at HSS
Partial knee replacement is widely recognized as a technically demanding surgery. As demonstrated in the scientific literature, data shows that choosing an orthopedic surgeon and institution with extensive experience with this procedure can help ensure a good result. In fact, at high-volume institutions like HSS, in well-selected patients, surgeons achieve the same longevity for partial knee replacement as that reported for total knee replacement. “It’s important to understand that partial knee replacement is a challenging procedure to perform,” says Michael M. Alexiades, MD, Attending Orthopedic Surgeon at HSS. “At HSS, we collect data on partial knee replacement patients on an ongoing basis. This allows us to continuously refine screening and surgical techniques to achieve predictable results and the best outcome possible.”
Orthopedic surgeons at world-renowned HSS perform more hip surgeries and knee replacements − including partial knee replacements − than any other hospital in the United States. (View surgeons at HSS who perform partial knee replacement.)
Updated: 2/3/2022
Authors
Michael M. Alexiades, MD
Attending Orthopedic Surgeon, Hospital for Special Surgery
Professor of Orthopedic Surgery, Weill Cornell Medical College
Chief, Sports Medicine Institute, Hospital for Special Surgery
Attending Orthopedic Surgeon, Hospital for Special Surgery
Related articles
References and additional reading
- Burger JA, Kleeblad LJ, Laas N, Pearle AD. Mid-term survivorship and patient-reported outcomes of robotic-arm assisted partial knee arthroplasty. Bone Joint J. 2020 Jan;102-B(1):108-116. doi: 10.1302/0301-620X.102B1.BJJ-2019-0510.R1. PMID: 31888356.
- Cui A, Li H, Wang D, Zhong J, Chen Y, Lu H. Global, regional prevalence, incidence and risk factors of knee osteoarthritis in population-based studies. EClinicalMedicine. 2020 Nov 26;29-30:100587. doi: 10.1016/j.eclinm.2020.100587. PMID: 34505846; PMCID: PMC7704420.
- Christ AB, Pearle AD, Mayman DJ, Haas SB. Robotic-Assisted Unicompartmental Knee Arthroplasty: State-of-the Art and Review of the Literature. J Arthroplasty. 2018 Jul;33(7):1994-2001. doi: 10.1016/j.arth.2018.01.050. Epub 2018 Mar 16. PMID: 29555499.
- Chawla H, van der List JP, Christ AB, Sobrero MR, Zuiderbaan HA, Pearle AD. Annual revision rates of partial versus total knee arthroplasty: A comparative meta-analysis. Knee. 2017 Mar;24(2):179-190. doi: 10.1016/j.knee.2016.11.006. PMID: 27916580.
- Gruskay J, Richardson S, Schairer W, Kahlenberg C, Steinhaus M, Rauck R, Pearle A. Incidence and safety profile of outpatient unicompartmental knee arthroplasty. Knee. 2019 Jun;26(3):708-713. doi: 10.1016/j.knee.2019.02.002. Epub 2019 Mar 8. PMID: 30853161.
- Heaps BM, Blevins JL, Chiu YF, Konopka JF, Patel SP, McLawhorn AS. Improving Estimates of Annual Survival Rates for Medial Unicompartmental Knee Arthroplasty, a Meta-Analysis. J Arthroplasty. 2019 Jul;34(7):1538-1545. doi: 10.1016/j.arth.2019.02.061. Epub 2019 Mar 6. PMID: 30954408.
- HSS Annual Report 2021.
- van der List JP, Sheng DL, Kleeblad LJ, Chawla H, Pearle AD. Outcomes of cementless unicompartmental and total knee arthroplasty: A systematic review. Knee. 2017 Jun;24(3):497-507. doi: 10.1016/j.knee.2016.10.010. Epub 2016 Dec 4. PMID: 27923627.
- Waldstein W, Kolbitsch P, Koller U, Boettner F, Windhager R. Sport and physical activity following unicompartmental knee arthroplasty: a systematic review. Knee Surg Sports Traumatol Arthrosc. 2017 Mar;25(3):717-728. doi: 10.1007/s00167-016-4167-1. Epub 2016 May 21. PMID: 27209192; PMCID: PMC5332483.

