Spinal Stenosis
Spinal stenosis is a pinched nerve condition that can cause pain in the back, neck and sometimes the arms and legs. It most commonly affects people between the ages of 50 and 60.

What is spinal stenosis?
Spinal stenosis refers to narrowing of the spinal canal or tunnel that houses the neural elements (nerves) that travel along the spinal column. The narrowing can be central stenosis (referring to the main channel) or it can be foraminal stenosis (referring to the “exit ramp” for each individual nerve root). The condition can occur in the cervical spine (neck), thoracic spine (mid back) or the lumbar spine (lower back). Cervical and lumbar stenosis are the most common forms, with lumbar spinal stenosis affecting more than 200,000 adults in the United States.
Anatomy of the spine and the mechanics of spinal stenosis
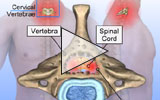
The spinal cord extends from the base of the brain and enters the spinal canal – a protective space inside the bony portions of the spine.
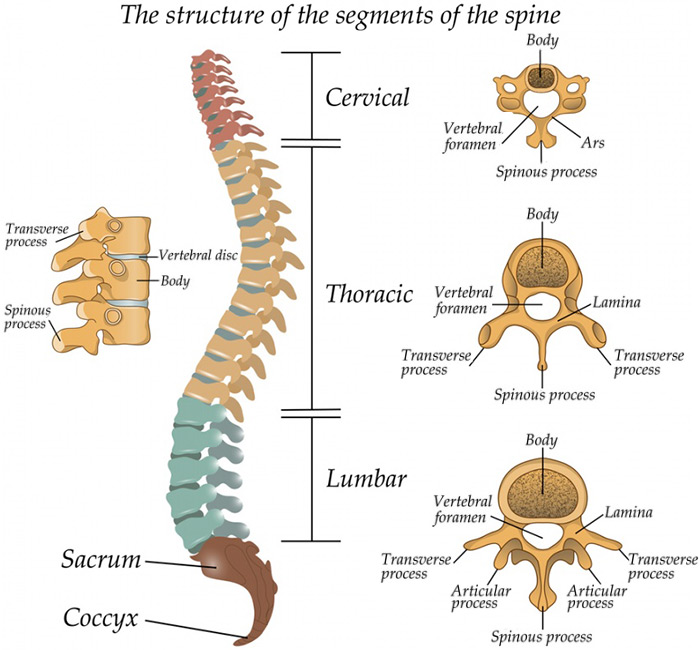
The spine is divided into three sections, named for their location and function:
- The cervical spine composes the body’s neck and allows body to turn the head in many directions.
- The thoracic spine supports the rib cage, protecting the heart, lungs, and large vessels.
- The lumbar spine connects the torso to the pelvis and allows the body to bend, flex, and twist around the torso.
In most cases, there is plenty of room inside the bony portion spine for the spinal cord and nerve roots to be housed comfortably and function normally. However, various conditions, including, degenerative arthritis of the spine (also called spondylosis), can cause narrowing of the spinal canal. This narrowing can, in some cases, eventually compress and damage the cord, and cause pain.
Animations illustrating cervical and lumbar spinal stenosis
What are the symptoms of spinal stenosis?
Spinal stenosis is a narrowing of the spinal canal which results in pressure on the nerves. The pressure on the nerves results in pain, numbness or weakness in the extremities. Cervical stenosis (in the neck) can affect the arms, legs and sometimes balance. Lumbar stenosis (in the low back) usually affects the buttocks and legs and can make standing or walking painful. Lumbar stenosis can put pressure on the sciatic nerve, and is one of the chief causes of sciatica.
What are some of the causes of spinal stenosis?
Stenosis can be caused by age-related degeneration of the spine or traumatic injury to the spine. In rarer instances, stenosis can be due to tumor, infection, or congenital anomaly (occurring at birth).
Stenosis can be congenital or developmental from a young age. It can also be caused by arthritic changes of the facet joints and narrowing of the discs between the spine bones with overgrowth of the ligaments that help stabilize the vertebrae. It can also be caused by slippage of one vertebra on the next or by scoliosis or curvature of the spine.
Who is at risk for spinal stenosis?
Patients in their 50’s and above are most commonly at risk for stenosis caused by arthritic changes to the spine. Developmental or congenital stenosis may affect patients in their late teens or twenties and above.
What is the treatment for spinal stenosis?
The early symptoms of stenosis can be treated with activity modification and anti-inflammatory medications. When symptoms become more significant, epidural steroid injections can be tried. If none of these give relief, then spinal decompression surgery may be required. Depending on the cause of the stenosis and where it is located, spinal fusion surgery may also be required. Learn more about spinal decompression and spinal fusion surgery.)
Articles on spinal stenosis and closely related conditions
Read about conditions causing low back pain, including a detailed overview of stenosis of the lower spine.
Articles on spinal stenosis treatments
Read about injection treatments and see animations of various surgeries for spinal stenosis.
- Epidural Steroid Injections: Frequently Asked Questions
- Spinal Cord Stimulator – A Compelling Treatment Technique for Chronic Pain
- ACDF Surgery: Anterior Cervical Discectomy and Fusion
- Spine Surgery: Posterior Cervical Laminotomy
- Cervical Laminoplasty
- Instrumented Cervical Laminectomy, Fusion
- Microdiscectomy: Surgical Treatment for a Herniated Disc
- Spine Surgery: Thoracic Laminectomy With Instrumentation, Fusion
- Lumbar Laminectomy: Spinal Decompression Surgery of the Lower Back
- Spine Surgery: Minimally Invasive Lumbar Discectomy / Percutaneous Disc Removal (PDR)
- ALIF Surgery: Anterior Lumbar Interbody Fusion
- PLIF Surgery: Posterior Lumbar Interbody Fusion
- TLIF Surgery: Transforaminal Lumbar Interbody Fusion
- Minimally Invasive Lower Back Surgery for Disc Degeneration: The Anterolateral (Side) Approach
Articles on other related conditions and issues
Spinal Stenosis Success Stories