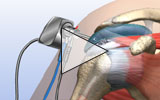
Rotator Cuff Surgery: Arthroscopic Repair of a Torn Rotator Cuff
The rotator cuff is a set of a four small muscles in the shoulder that allow the upper arm to rotate. When a rotator cuff is torn, the tendon part of the muscle tears away from the bone of the upper arm. A rotator cuff tear can result from an injury such as a fall or heavy lifting, or from normal wear-and-tear and repetitive activities over many years. Some minor tears may be treated without surgery. Many, however, require surgical intervention to heal properly.
What is the surgery for a torn rotator cuff?
To repair a torn rotator cuff, an orthopedic surgeon reattaches the tendon to the humerus (upper arm bone) using an absorbable suture anchor. The surgery’s success is dependent on how well this interface between the tendon and bone heals.
How is rotator cuff surgery performed?
Rotator cuff surgery is performed arthroscopically. In a shoulder arthroscopy, small incisions are made and an arthroscope − a small tube fixed with a camera – is navigated to the site of the tear. We then use specially designed instruments that allow us to repair the rotator cuff with minimal trauma to the surrounding muscles and tissues.
Patients at Hospital for Special Surgery have this procedure done under a nerve block (regional anesthesia) and partial sedation rather than under general anesthesia. This minimizes the amount of pain and anesthesia medications that are given, thereby reducing nausea and vomiting. These improvements in minimally invasive techniques and anesthesia allow most of our patients to go home only a few hours after their procedure.
First, an arthroscopy of the glenohumeral joint (the ball-and-socket portion of the shoulder joint) is performed to identify and treat other associated problems, such as a biceps tendon injury, loose bodies or a torn labrum. (The shoulder labrum is a rim of cartilage that surrounds the glenoid, the cup portion of the shoulder joint.) A partial rotator cuff tear (a tear through less than 50% of the thickness of the rotator cuff tendon) can be trimmed with a shaver at this time.
The arthroscope is then placed in the subacromial space (below the acromion, a bony portion at the top of the scapula or shoulder blade), under which the rotator cuff tendon passes. A subacromial decompression is then performed to open up the subacromial space. This procedure, called an acromioplasty, involves removing a bone spur and irregularities on the underside of the acromion, which can be a cause of rotator cuff irritation and tearing. The torn tendon is then reattached to the bone with the use of suture anchors and sutures.
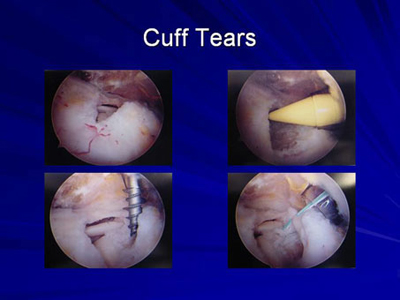
Rotator cuff tears
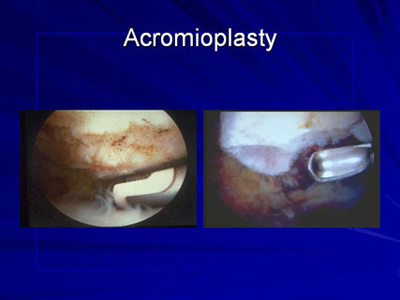
Acromioplasty
When is rotator cuff surgery recommended?
Surgery is recommended for a full thickness tear, or in those patients with a partial thickness tear who have failed conservative treatment (two months of physical therapy). If a patient tries conservative treatments and continues to have pain and difficulty with activities after two or three months, he or she may consider surgery to repair the tear.
Is there an alternative to rotator cuff surgery?
Small or partial rotator cuff tears may be treated with two months of physical therapy.
Do you need surgery for partial rotator cuff tears?
If physical therapy has not effectively restored strength and function, then surgery is the only option. Physical therapy is considered effective if a patient feels their shoulder function and strength has improved.
What is the risk of waiting to have rotator cuff surgery?
Tears tend to get larger with time. The results of repairing large or massive tears are not as good as repairing smaller tears, Delaying surgery in patients who need it can result in progression of a partial tear to a full tear, the propagation of a small tear to a larger one, fatty infiltration of the damaged tendon and muscle, and muscle atrophy and weakness.
Most patients will still initially undergo a trial of physical therapy to see if surgery can be avoided, but for those who do not respond, we recognize the value of initiating surgery sooner rather than later.
How do you select a doctor for rotator cuff surgery?
It is important to select an orthopedic surgeon who has experience repairing rotator cuff tears, preferably one who completed a fellowship in sports medicine. Find a doctor at HSS who treats rotator cuff tears.
Is rotator cuff surgery done outpatient?
Yes. The surgery takes less than a half hour, and the patient is placed in a sling and can return home on the day of surgery.
How long does it take to recover from rotator cuff surgery?
It takes six to eight weeks for the tendon to heal to the bone. Complete recovery time varies by size of the tear. For a small tears, full recovery time is about four months, for large tears, six months. For severe, massive tears, a complete recovery can take anywhere from 6 to 12 months.
Patients can often return to most activities after about 12 weeks after surgery, but participation in vigorous sports may be restricted for four to six months. The goal is to achieve full range of motion and full strength.
How many weeks of physical therapy do you need for rotator cuff surgery?
Generally, a patient wears a sling for the first two to three weeks and begins physical therapy one week after surgery. The physical therapy program typically lasts for three to four months. Strengthening exercises begin after the 6- to 10-week healing period.
Do's and don'ts after rotator cuff surgery?
Protecting the repair for the first six to eight weeks is essential to allow healing to the bone. Because patients may feel well quickly, it's particularly important that they exercise care in protecting the joint during the healing period. Shoulder surgeons prescribe a very specific and detailed rehabilitation program following surgery which must be strictly followed.
What are the best exercises after rotator cuff surgery?
A licensed physical therapist can guide the patient on appropriate exercises. These may differ from case to case.
How long before you can drive after rotator cuff surgery?
Typically, patients can return to driving after two to four weeks.
What is the success rate for rotator cuff surgery?
Rotator cuff surgery has more than a 95% success rate for small tears. For two tendon tears, the success rate is still greater than 70%. Untreated tears tend to get bigger, so it is best to repair tears while they are small.
However, even those patients with very large tendon tears may benefit from surgery. In some cases, we can use a technique called margin conversions. This involves covering the humeral head with grafted tissue to hold the tendon in place in the joint. When the tendon tissue is insufficient for direct repair, we place a patch of donated tissue in the area. When these tissue grafts are required, shoulder surgeons usually perform a mini-open repair, rather than an arthroscopic repair.
Updated: 12/20/2021
Arthroscopic images provided courtesy of Russell F. Warren, MD.
Authors
Associate Attending Orthopedic Surgeon, Hospital for Special Surgery
Associate Professor of Clinical Orthopedic Surgery, Weill Cornell Medical College