Arthroscopic Surgery for ACL Reconstruction, Meniscal Repair, and Other Knee Injuries
Knee arthroscopy is a minimally invasive technique that allows orthopedic surgeons to assess – and in most cases, treat – a range of conditions affecting the knee joint. In particular, it is commonly used for ACL reconstruction and meniscus surgery, sometimes at the same time.
During the procedure, the orthopedic surgeon makes small incisions or portals in the affected joint, and then inserts a tiny camera and fiber optics to light the interior space. Pictures obtained with the camera are then projected onto a screen in the operating suite.
While many people are now familiar with the technique, it might come as a surprise that the first arthroscopic evaluation of a knee actually took place back in 1918 by Japanese surgeon Dr. Kenji Takagi. The procedure involved the insertion of a scope into a joint to visualize it but without the benefit of additional lighting. In the following decades, subsequent efforts to apply the technique met with limited success. In 1962, Takagi's former student, Dr. Masaki Watanabe, performed the first clinical arthroscopic meniscectomy in 1962.
It wasn't until the advent of fiber optics in the 1970s and 1980s, that arthroscopy became a useful and "user-friendly" technique for physicians. Today, thanks to the availability of sophisticated instrumentation, use of arthroscopy, particularly in the knee, is widespread.
What are the advantages of arthroscopic knee surgery?
The primary advantage afforded by arthroscopy is the ability to gain multiple views inside the joint. In the past, gaining access to some of these areas required an arthrotomy – a surgery in which an open incision was made – and dislocation of the patella or knee cap. That procedure required additional trauma to the knee and carried the risk of additional injury to the joint.
In contrast, arthroscopic examination of the knee joint usually does little damage to surrounding soft tissues. While most orthopedic surgeons continue to rely on radiographs (X-rays) and MRI to provide important preliminary information, many agree that arthroscopy is the best diagnostic tool available.
Arthroscopy offers pieces of information that the other tests don't, including that which is derived by probing the affected tissue. MRI is a wonderful tool to evaluate the structure of the soft tissues, but does not provide the tactile information acquired by probing the soft tissues and evaluating them with direct visual observation.
Here at Hospital for Special Surgery, general anesthesia is rarely indicated for arthroscopic surgery of the knee which is generally performed with regional anesthesia or, occasionally, local anesthesia.1
Therapeutic applications of arthroscopy can also eliminate the need for large incisions.
Arthroscopic ACL and meniscus surgery
Reconstruction of the ACL (anterior cruciate ligament) and repair of a torn meniscus are among the most commonly performed arthroscopic surgeries.
Within the knee, these structures perform distinct functions. The ACL helps stabilize and support the joint. There are two menisci in the knee. These C-shaped "cushions" of cartilage help protect the articular cartilage, the lining of the bones that allows them to glide smoothly against one another during motion. (Injury or loss of articular cartilage results in arthritis.) These structures also act as shock absorbers, distributing load across the knee.
Injuries, including tears, to both the ACL and the meniscus are common, particularly in athletes. (Torn menisci are also seen in older patients as the result of a degenerative process.) Moreover, surgeons often see them in conjunction with one another. This may be the result of injuries suffered at the same time, or in sequence; that is, a person with a torn ACL is at greater risk of injuring the menisci. Statistics show that more than 60% of patients diagnosed with an ACL tear also have a torn meniscus. A gender specific difference in ACL injuries among young female athletes has been demonstrated in recent years. Females are 2 to 6 times more likely to tear their ACL than their male cohorts, depending upon the sport.2
Some ACL and meniscus injuries can be treated nonsurgically with rest, physical therapy, and activity modification. However, in a young active person, choosing to forgo ACL reconstruction or meniscus repair is likely to result in persistent instability and pain in the knee, as well as setting the stage for degenerative arthritis if they are unwilling to modify their sport-related activities significantly.
What is the recovery process for knee arthroscopy?
Arthroscopic surgery takes place only after the immediate post-injury swelling and inflammation has diminished, and the patient has recovered almost complete range of motion.
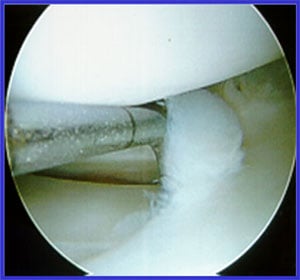
Arthroscopic photo showing meniscus tear.
When the ACL is sustains a complete tear, the surgeon must replace it with a graft. Grafts can be obtained from the patient’s own knee (termed an autograft), or from donated tissue (termed an allograft, but sometimes referred to as a cadaver graft). Generally, autografts are used in the adolescent and young population of athletes, and allografts are used in the older patient population. The autograft sources include the bone-patellar tendon-bone graft, the hamstring tendon graft or the quadriceps tendon graft. When an autograft is used, it is retrieved through a small open incision.
The general success rate following ACL reconstruction is 85 to 90%. In recent years the revision ACL surgery rate has increased, often as a result of recurrent injury to the knee sometime after the original surgery.3
Recovery time from an ACL reconstruction varies, with a period from about 6 to 9 months representing an average time required before the athlete returns to collision sports. During that period the patient participates in a rehabilitation program designed to restore range of motion, strengthen muscles, and regain balance and sports-specific skills.
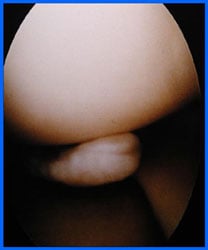
Arthroscopy photo showing meniscus tear.
The treatment goal for a torn meniscus is preservation of the structure. The meniscus serves a purpose - to transmit load across the joint. Depending upon the type of tear, the location of the tear, the quality of the torn fragment, and the age of the patient, repairing the meniscus is the surgeon’s priority. It has been demonstrated that when an athlete sustains a tear that cannot be (or is not) repaired, they are at increased risk for developing articular cartilage damage – early arthritis. 4
Where possible, the surgeon sutures the torn meniscus together using one of a variety of techniques. The sutures are placed using arthroscopic techniques. When the meniscus tear cannot be repaired because of the location, tear type, poor quality of tissue, or inadequate blood supply (usually associated with the location of the tear), the meniscus is partially excised – termed a partial meniscectomy – while preserving as much of the normal structure as possible. In some cases, when the tear is complex or severe, the orthopedic surgeon must remove the majority of the meniscus. In these cases, it is often appropriate to transplant an allograft meniscus from donor tissue at a later date to prevent degenerative deterioration of the joint.
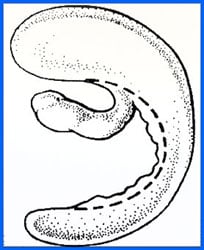
Illustration showing tear and area of resection.
Approximately 70% to 90% of arthroscopic meniscus repairs are successful. Interestingly, those patients who have injured both their ACL and their meniscus, and who undergo treatment for both injuries at the same time, have higher success rates. In reconstructing an ACL, small tunnels are placed in the tibia and the femur (through which the graft is placed), which results in a small amount of blood. The belief is that the blood carries factors that may actually stimulate healing of the meniscus."
Recovery time for these surgeries varies, with an average range of 3 to 6 weeks with respect to partial meniscectomy and 12 to 16 weeks regarding meniscus repair. Patients are enrolled in a rehabilitation program during this period.
Other applications of arthroscopic knee surgery
In addition to ACL reconstruction and meniscus repair, arthroscopy is used for:
- reconstruction of other ligaments that support the knee, such as the medial collateral ligament (MCL) and posterior cruciate ligament (PCL)
- articular cartilage repair and regeneration
- Arthritis of the knee to provide relief from symptoms of clicking or locking
Using arthroscopic techniques, the orthopedic surgeon can smooth defects or remove small pieces of loose tissue that may be causing these problems. In general, the arthroscopic treatment of knee arthritis has limited indications and is considered only after exhausting other non-operative treatments in special circumstances.
Arthroscopy can also help in the treatment of fractures in combination with an open procedure to repair the bone. When a patient has a fracture in the knee, arthroscopy allows us to see these areas without disrupting the joint. Doctors can set the bone and place any necessary pins, screws, or additional hardware with minimal risk of additional injury to the patient.
If you are considering an arthroscopic procedure, it's important to be sure that the orthopedist is qualified. Most orthopedic surgeons have the appropriate training to perform diagnostic arthroscopy, that is the use of the technique to evaluate the knee. However, operations such as ligament reconstructions, meniscus repairs, meniscal allograft transplantations, and articular cartilage restoration techniques, require specialized training in sports medicine or arthroscopic surgery.
References
- Dunn WR, Cordasco FA, Flynn E, Jules K, Gordon M, Liguori G. A prospective randomized comparison of spinal anesthesia versus local anesthesia with propofol infusion for knee arthroscopy. Arthroscopy. 2006;22(5):479-83. PMID: 16651155. https://pubmed.ncbi.nlm.nih.gov/16651155/
- Toth AP, Cordasco FA. Anterior cruciate ligament injuries in the female athlete. J Gend Specif Med. 2001;4(4):25-34. PMID: 11727468. https://pubmed.ncbi.nlm.nih.gov/11727468/
- Battaglia MJ 2nd, Cordasco FA, Hannafin JA, Rodeo SA, O'Brien SJ, Altchek DW, Cavanaugh J, Wickiewicz TL, Warren RF. Results of revision anterior cruciate ligament surgery. Am J Sports Med. 2007 Dec;35(12):2057-66. doi: 10.1177/0363546507307391. Epub 2007 Oct 11. PMID: 17932401. https://pubmed.ncbi.nlm.nih.gov/17932401/
- Williams RJ 3rd, Warner KK, Petrigliano FA, Potter HG, Hatch J, Cordasco FA. MRI evaluation of isolated arthroscopic partial meniscectomy patients at a minimum five-year follow-up. HSS J. 2007 Feb;3(1):35-43. doi: 10.1007/s11420-006-9031-2. PMID: 18751768; PMCID: PMC2504089. https://pubmed.ncbi.nlm.nih.gov/18751768/

